Gastroenterology — MCQs

On this page
Pigment gallstones are usually not seen in which of the following conditions?
Child-Turcotte-Pugh classification is used in the assessment of which condition?
A 60-year-old patient presents with bright red blood per rectum. The bleeding started abruptly several hours prior to visit. The patient reports lightheadedness when standing up rapidly but denies abdominal pain, cramping, fever, nausea, or vomiting. He has no history of previous bleeding or abdominal pain but has a history of coronary artery disease and takes aspirin. He is afebrile, slightly hypotensive and tachycardic, but hemodynamically stable. Examination reveals decreased skin turgor and dry mucous membranes. There is no abdominal tenderness. Rectal examination is positive for gross blood. What is the most likely diagnosis?
Cobalamin absorption may be abnormal in all conditions EXCEPT:
A 55-year-old male patient presenting with gastritis symptoms was diagnosed with a gastric ulcer three years ago and underwent partial gastrectomy. He is currently on high-dose omeprazole. A follow-up endoscopy reveals two ulcerative lesions in the gastric mucosa. What is the next step in management?
Which of the following conditions leads to the endoscopic appearance shown in the image?
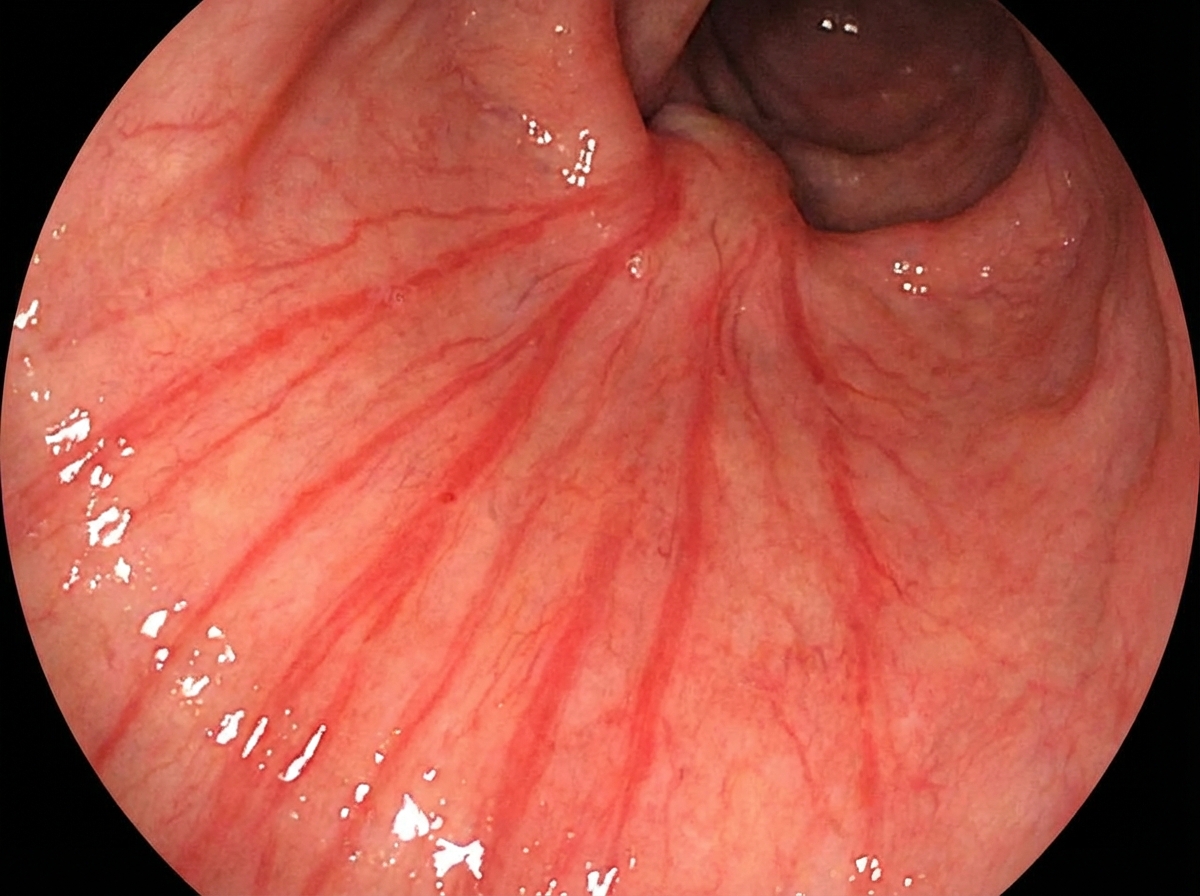
A 65-year-old male presents with abdominal pain and distension. He reports maroon-colored stools and has a past medical history of cerebrovascular accident and myocardial infarction. What is the most probable diagnosis?
A 45-year-old male complains of weakness. He is obese, a type 2 diabetic, and hypertensive. General examination reveals hepatomegaly. Icterus is visible on the sclera, and pale coloration of the skin is present. Which of the following liver diseases can be seen in this patient?
Which of the following statements about pleural effusion in cirrhosis is FALSE?
Sustained virologic response to antiviral therapy (IFN + Ribavirin) in hepatitis C is indicated by which of the following?
Practice by Chapter
Esophageal Disorders
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Irritable Bowel Syndrome
Practice Questions
Malabsorption Syndromes
Practice Questions
Pancreatitis (Acute and Chronic)
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Liver Diseases and Cirrhosis
Practice Questions
Viral Hepatitis
Practice Questions
Biliary Tract Disorders
Practice Questions
Gastrointestinal Motility Disorders
Practice Questions
Gastrointestinal Malignancies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
