Preventive Cardiology — MCQs

For a patient diagnosed with dyslipidemia characterized by elevated LDL cholesterol levels, what is the most appropriate treatment?
True about Cardiovascular disease (CVD)
Primordial prevention in myocardial infarction is all except -
Atorvastatin is used as an anti-dyslipidemic drug. These drugs inhibit their target enzyme by:-
According to WHO guidelines, to decrease both coronary heart disease and diabetes, triple treatment involves:
In which of the following clinical conditions does the use of anticoagulants provide maximum benefit?
An adolescent with type 1 diabetes returns for a follow-up visit after his annual check-up last week. You note that his serum glucose is elevated, and his glycosylated hemoglobin (hemoglobin A1C) is 16.7%. This finding suggests poor control of his diabetes over at least which of the following time-periods?
Common cause of chronic pancreatitis:
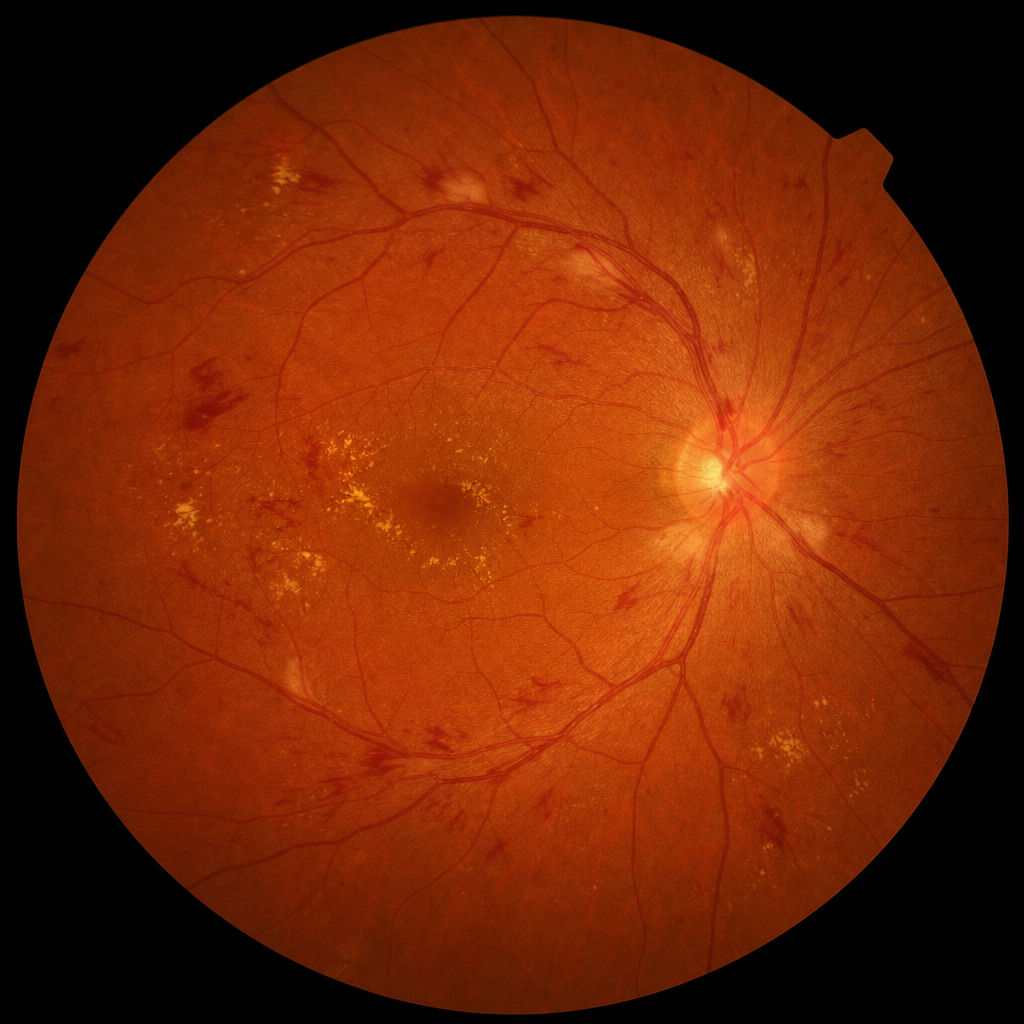
A 62-year-old hypertensive male presents to the emergency department with sudden-onset tearing chest pain radiating to the back. BP is 180/110 mmHg in the right arm and 150/90 mmHg in the left arm. ECG shows no ST changes. The patient is hemodynamically stable. The chest X-ray is shown in Image 2. What is the most appropriate immediate next investigation?
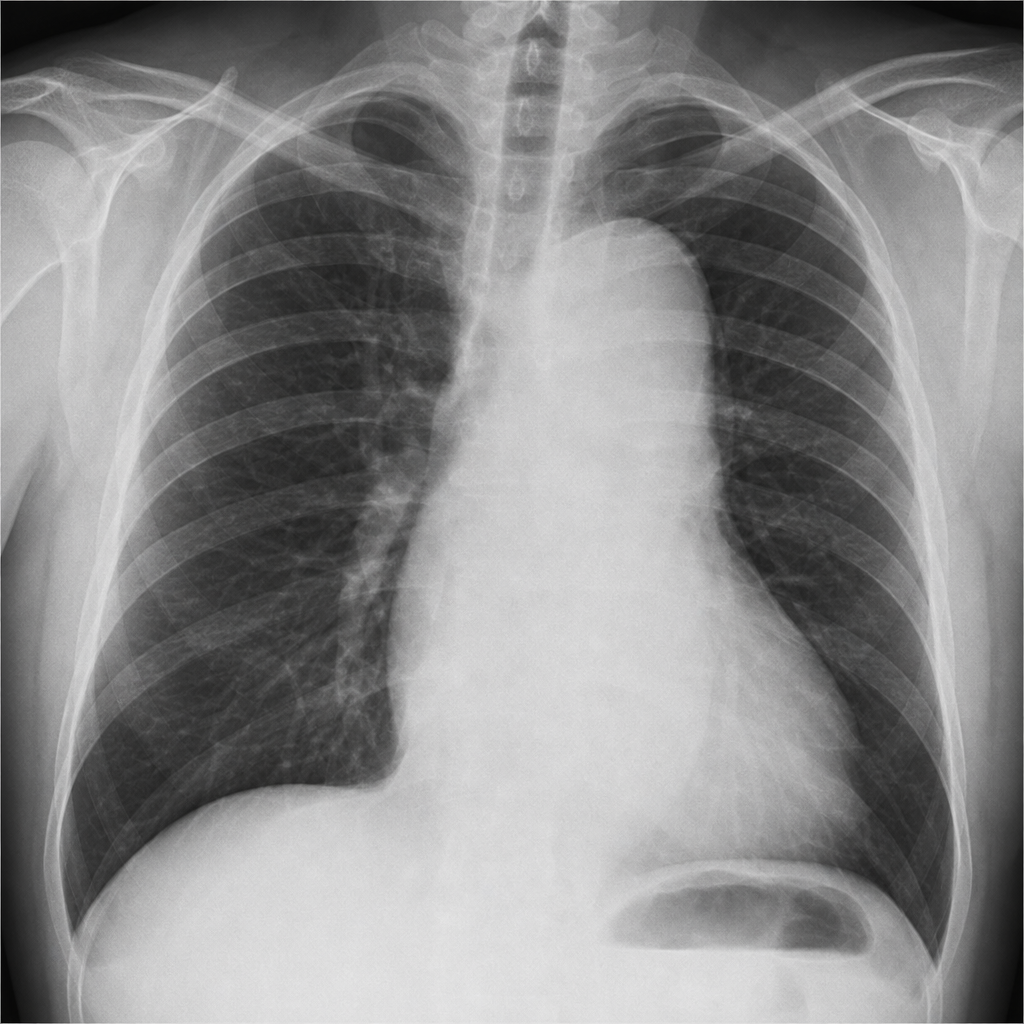
A 45-year-old man with no prior medical history presents to the emergency department with a 3-day history of severe headache, blurred vision, and nausea. His blood pressure is 240/140 mmHg. Neurological examination is intact. Fundoscopy is performed (Image 1). Which of the following is the most appropriate immediate management target for blood pressure reduction over the first hour?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
