Congenital Heart Disease in Adults — MCQs

Which is the most common congenital cardiac defect?
Which of the following is a manifestation of Tetralogy of Fallot?
Reversal of shunt is not possible in natural history of?
Tetralogy of Fallot presents with one of the following:
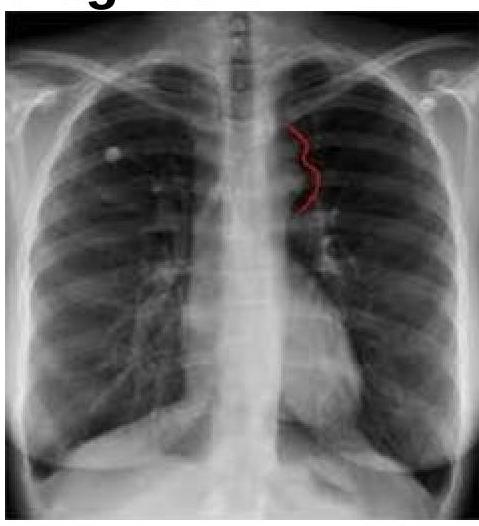
The chest radiograph shown below is from a 25-year-old male patient presenting with hypertension. The image demonstrates bilateral inferior rib notching. What is the most likely diagnosis?
True about Ebstein anomaly is ?
Eisenmenger syndrome-True are All except ?
A 9 year old boy with Fallot's tetralogy, had high grade fever followed by focal seizure 2 days prior to hospital admission. His blood counts were increased and predominantly polymorphs. CT scan of the head showed a focal lesion suggestive of an abscess. Where would be the commonest location of brain abscess in this patient?
Which of the following is the most appropriate true statement regarding ostium primum atrial septal defect (ASD)?
Pressure difference of 5 mm Hg between the two upper limbs occurs in which congenital heart disease?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
