General Medicine — MCQs

On this page
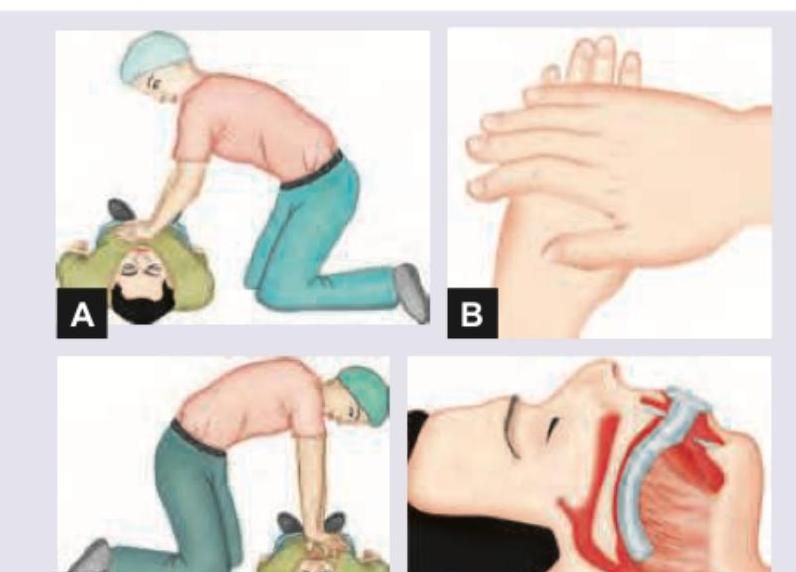
Which of the following is the correct technique of giving CPR?
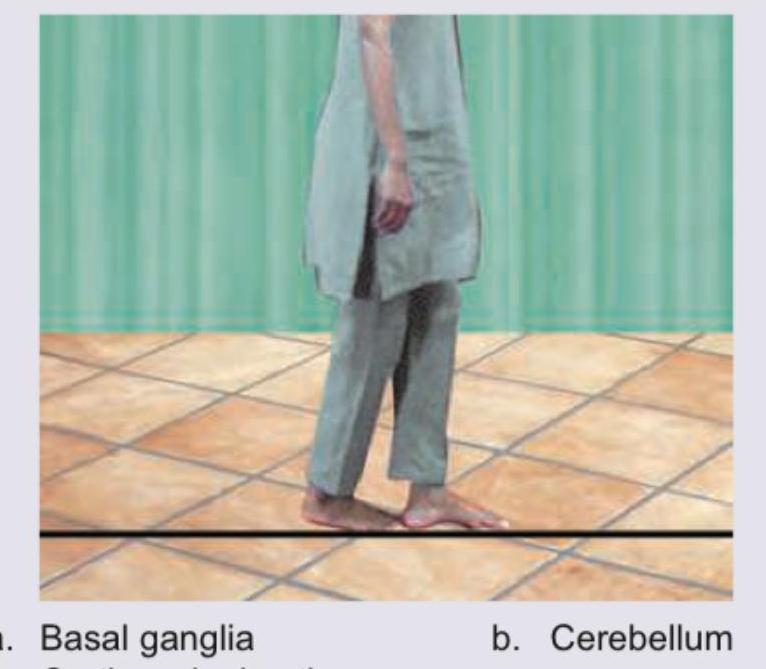
The following test is performed for evaluating the integrity of: (Recent NEET Pattern 2016-17)
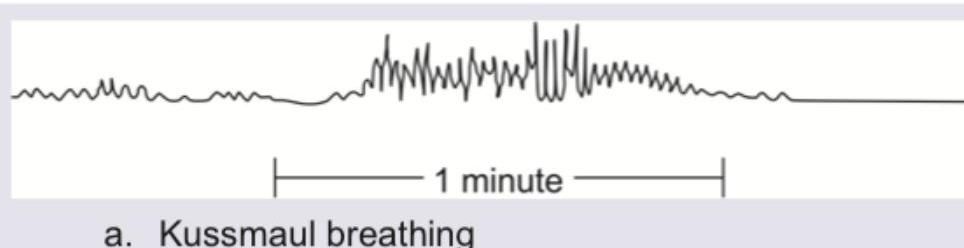
Which pattern of breathing is shown below?
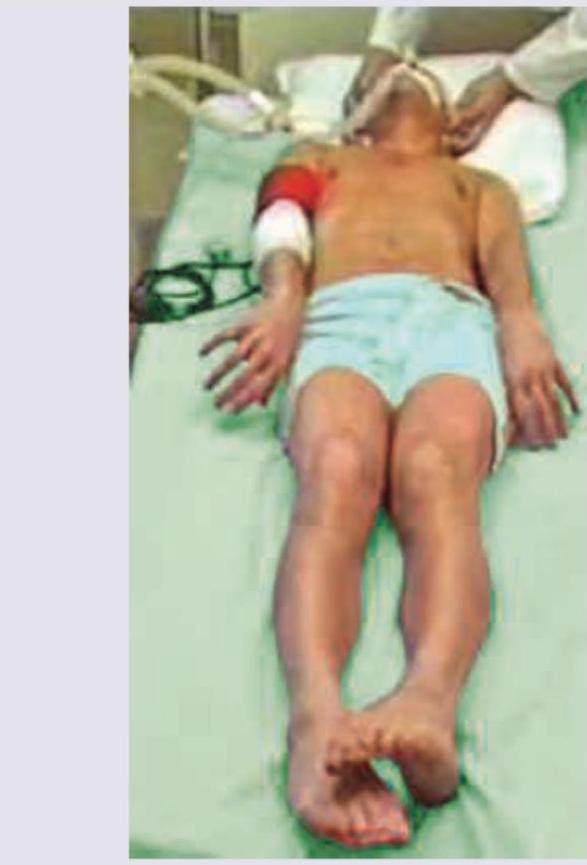
A head trauma patient is shown below. Diagnosis is?
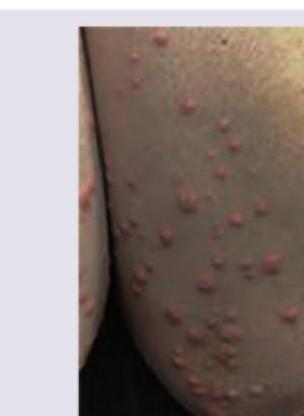
A patient presents with the following lesions on the elbows and his blood work shows lactescent plasma. Which is correct about the lesions?
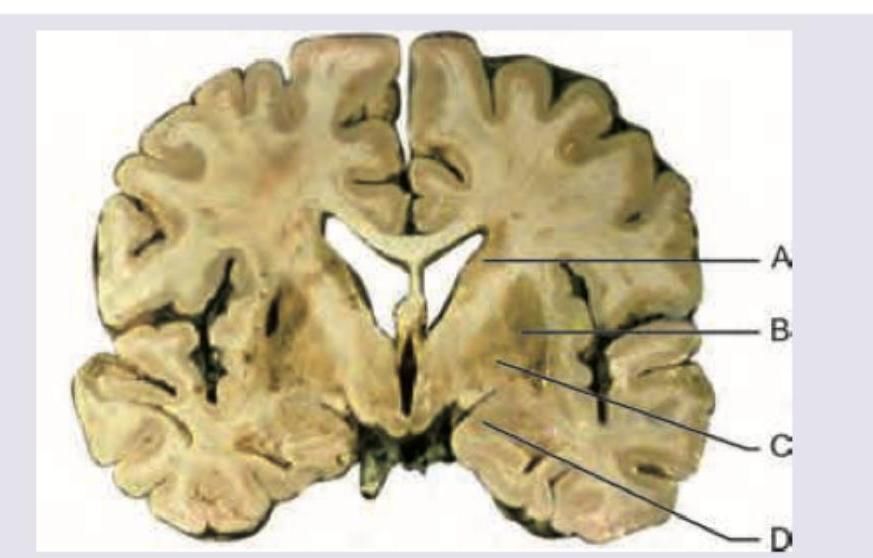
Which of the following sites in the most common site of intraparenchymal bleeding?
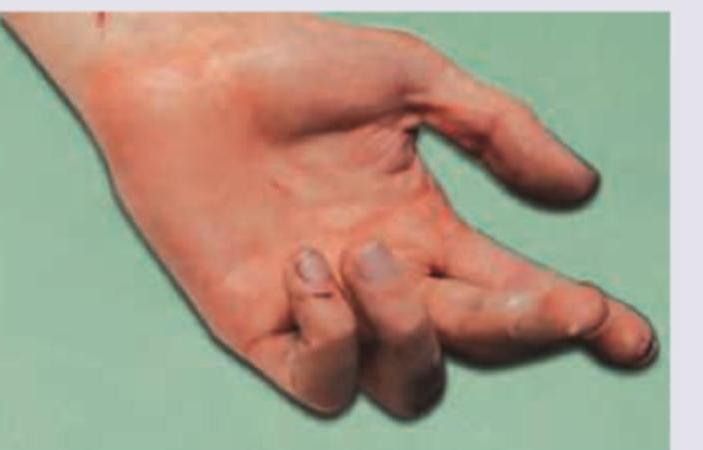
The deformity shown below can be due to involvement of: (AIIMS May 2016)
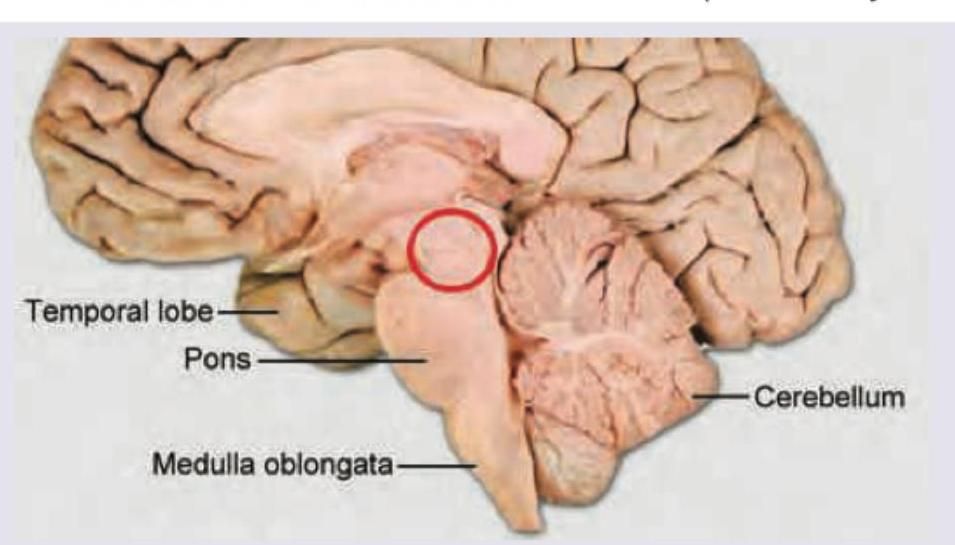
Which disease occurs due to involvement of the structure marked in red? (AIIMS May 2018)
What is the function of the tube shown below?

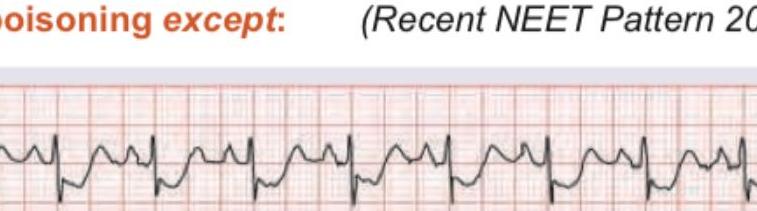
A 40-year-old farmer tried committing suicide by consuming two Sulphas (aluminium phosphide) tablets. On admission pulse is 110 bpm with BP of 80 / 60 mm Hg and GCS of 7 / 15 . SpO2 in room air is 80 %. ECG was performed. All are true about this poisoning except:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
