Body Fluid Identification — MCQs

Which test is most sensitive for detecting semen in forensic investigations?
What test is used to detect the presence of semen in the vaginal secretions of a rape victim?
Disputed maternity can be solved by using the following tests, EXCEPT:
Enzyme that can be traced in semen sample of 8-10 weeks is:
Which of the following methods is used for demonstrating old washed bloodstains?
Best site for DNA extraction from a 2-month-old decomposed body?
A 50 kg patient has 40 % burn of the body surface area. Calculate the ringer lactate solution to be given for first 8 hours of fluid:
In adults, circulatory collapse occurs after what percent of burns of total body surface area?
To calculate the initial fluid requirement in a burn patient, the best approach is:
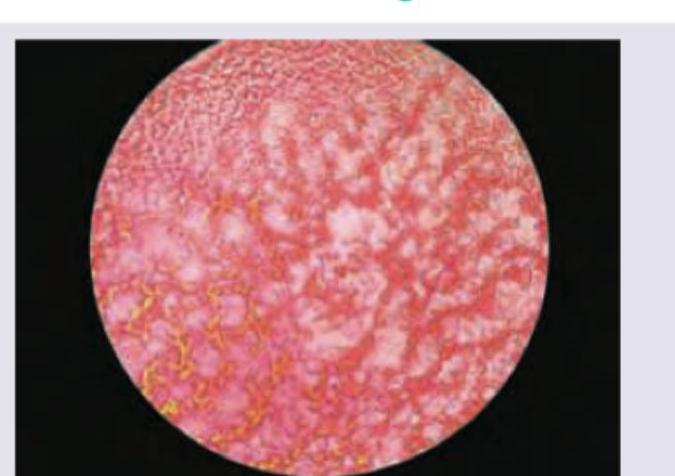
Which of the following tests for identifying blood stains is shown in the image below?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
