Otolaryngology Basics — MCQs

On this page
Masculine voice in females is treated by which of the following procedures?
What is the most common cause of chronic laryngeal stenosis?
Which of the following conditions does NOT present with pain similar to trigeminal neuralgia?
In laryngeal cancer, if the anterior commissure is involved, what is the best management?
What is the sensory nerve supply of the larynx below the level of the vocal cord?
Identify the instrument used in ENT surgery.
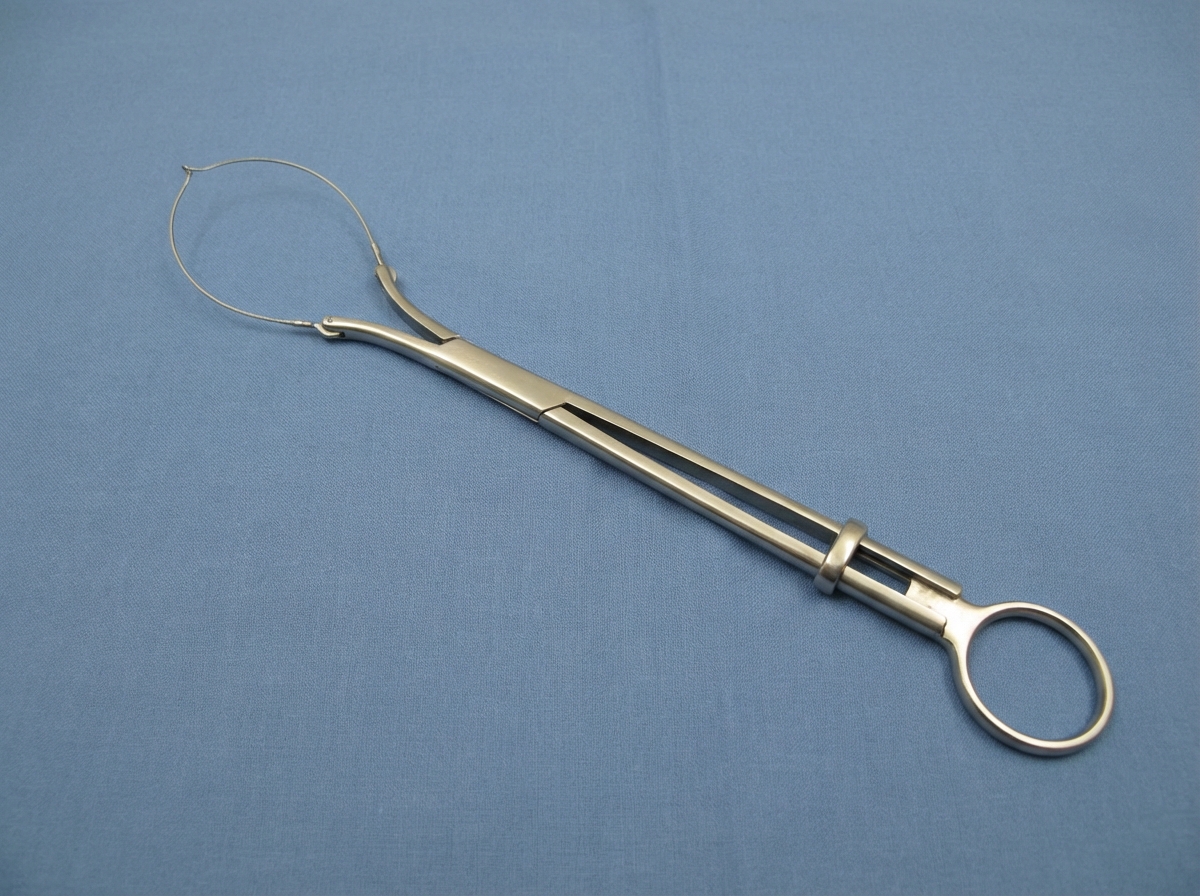
All of the following laryngeal muscles are adductors of vocal cords except?
Singer's nodule is due to:
Cricothyrotomy is converted to tracheostomy at an early stage to:
The recurrent laryngeal nerve supplies all laryngeal muscles except which one?
Practice by Chapter
Embryology of the Ear, Nose, and Throat
Practice Questions
Anatomy of the Ear
Practice Questions
Anatomy of the Nose and Paranasal Sinuses
Practice Questions
Anatomy of the Oral Cavity and Pharynx
Practice Questions
Anatomy of the Larynx
Practice Questions
Physiology of Hearing
Practice Questions
Physiology of Balance
Practice Questions
Physiology of Smell and Taste
Practice Questions
Physiology of Speech and Swallowing
Practice Questions
Clinical Examination in ENT
Practice Questions
Diagnostic Investigations in ENT
Practice Questions
Surgical Principles in Otolaryngology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
