Otolaryngology Basics — MCQs

On this page
What is the most common presentation of glottis carcinoma?
Which of the following statements is true regarding congenital subglottic stenosis?
What is the most common mode of treatment for laryngomalacia?
What is the term for a young man whose voice has not broken?
What is the most common benign tumor of the larynx in a child between 2-5 years of age?
Which of the following is indicative of a foreign body in the tracheobronchial tree in a child?
In direct laryngoscopy, which of the following structures can be visualized?
What is the most common congenital abnormality of the larynx?
The Heimlich maneuver is used for what condition?
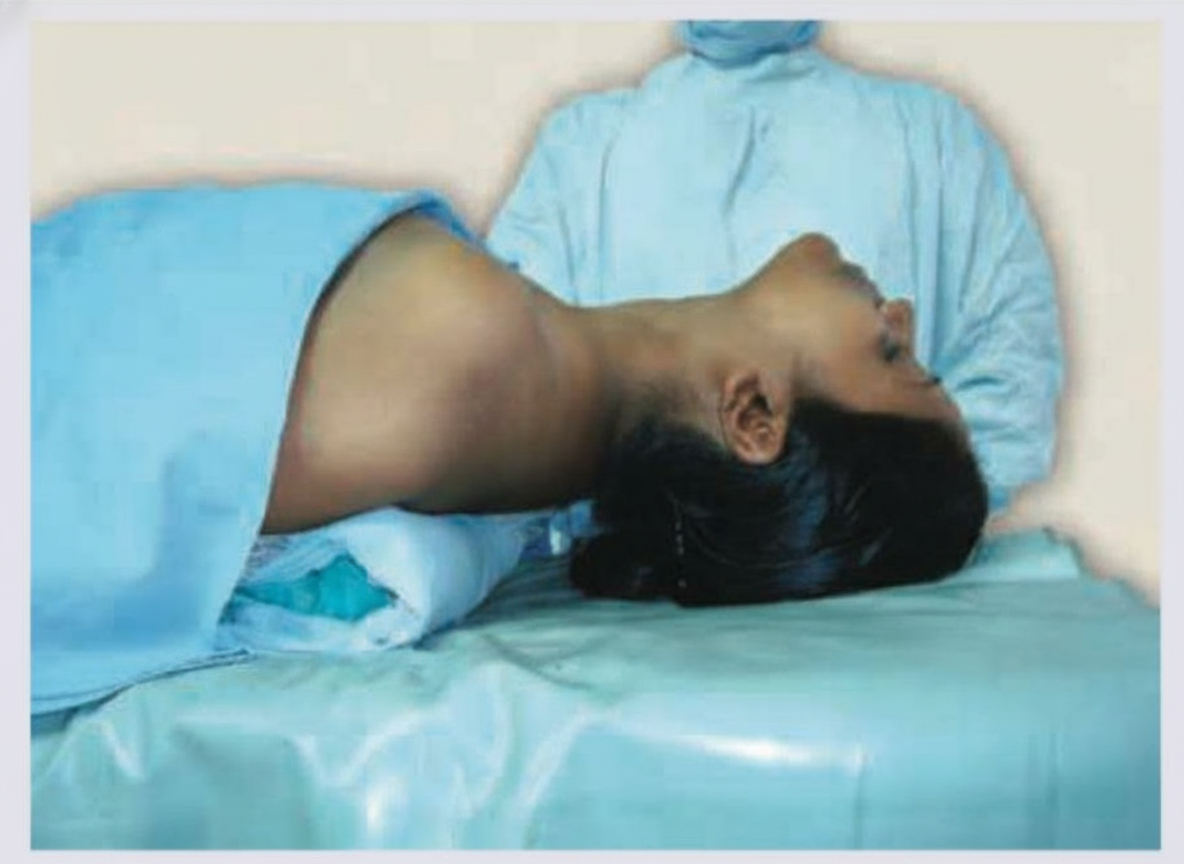
Tonsillectomy is being performed in the given patient. What position is being used?
Practice by Chapter
Embryology of the Ear, Nose, and Throat
Practice Questions
Anatomy of the Ear
Practice Questions
Anatomy of the Nose and Paranasal Sinuses
Practice Questions
Anatomy of the Oral Cavity and Pharynx
Practice Questions
Anatomy of the Larynx
Practice Questions
Physiology of Hearing
Practice Questions
Physiology of Balance
Practice Questions
Physiology of Smell and Taste
Practice Questions
Physiology of Speech and Swallowing
Practice Questions
Clinical Examination in ENT
Practice Questions
Diagnostic Investigations in ENT
Practice Questions
Surgical Principles in Otolaryngology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
