Neurotology — MCQs

On this page
Which of the following tests is recommended for neonatal screening of hearing?
Angular movement is sensed by which structure?
A 70-year-old male presents with loss of sensation in the external auditory meatus (Hitselberger sign positive). What is the likely diagnosis?
Auditory neurotherapy is an effective modality of treatment for which of the following abnormalities of hearing?
A laparoscopic intranasal approach is used for accessing all of the following EXCEPT?
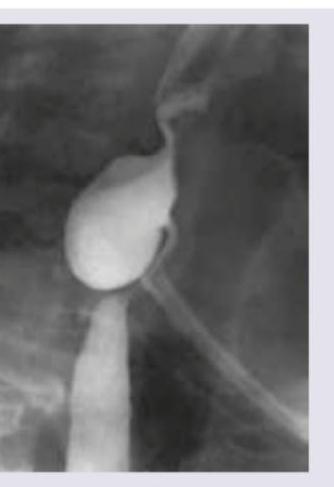
An 80-year-old female presents with complaints of difficulty swallowing and foul breath for 4 months. On auscultation, her lung fields have crepitations. A barium swallow finding is shown. What is your diagnosis?
Fluctuating deafness is a characteristic symptom of which condition?
Malignant otitis externa is caused by:
Scanty, foul-smelling, painless discharge from the ear is a characteristic feature of which of the following lesions?
The organ of Corti is located within which part of the inner ear?
Practice by Chapter
Vestibular System Anatomy and Physiology
Practice Questions
Vestibular Testing
Practice Questions
Benign Paroxysmal Positional Vertigo
Practice Questions
Ménière's Disease
Practice Questions
Vestibular Neuritis
Practice Questions
Labyrinthitis
Practice Questions
Acoustic Neuroma
Practice Questions
Other Cerebellopontine Angle Tumors
Practice Questions
Facial Nerve Disorders
Practice Questions
Skull Base Surgery
Practice Questions
Cochlear Implantation
Practice Questions
Vestibular Schwannoma Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
