Neurotology — MCQs

On this page
Gelle's phenomenon is absent in which of the following conditions?
What anatomical feature causes the "cone of light" observed during otoscopy?
The organ of Corti is the sensory organ for which sense?
All of the following conditions will produce nystagmus to the left except?
A congenital fistula that opens externally on the side of the neck, anterior to the sternocleidomastoid muscle, is an abnormality of which developmental structure?
What complication results from mastoid infection that erodes through the outer table of the bone?
Gradenigo's triad is caused due to involvement of which structure?
What is the investigation of choice for an acoustic neuroma of 1 cm diameter?
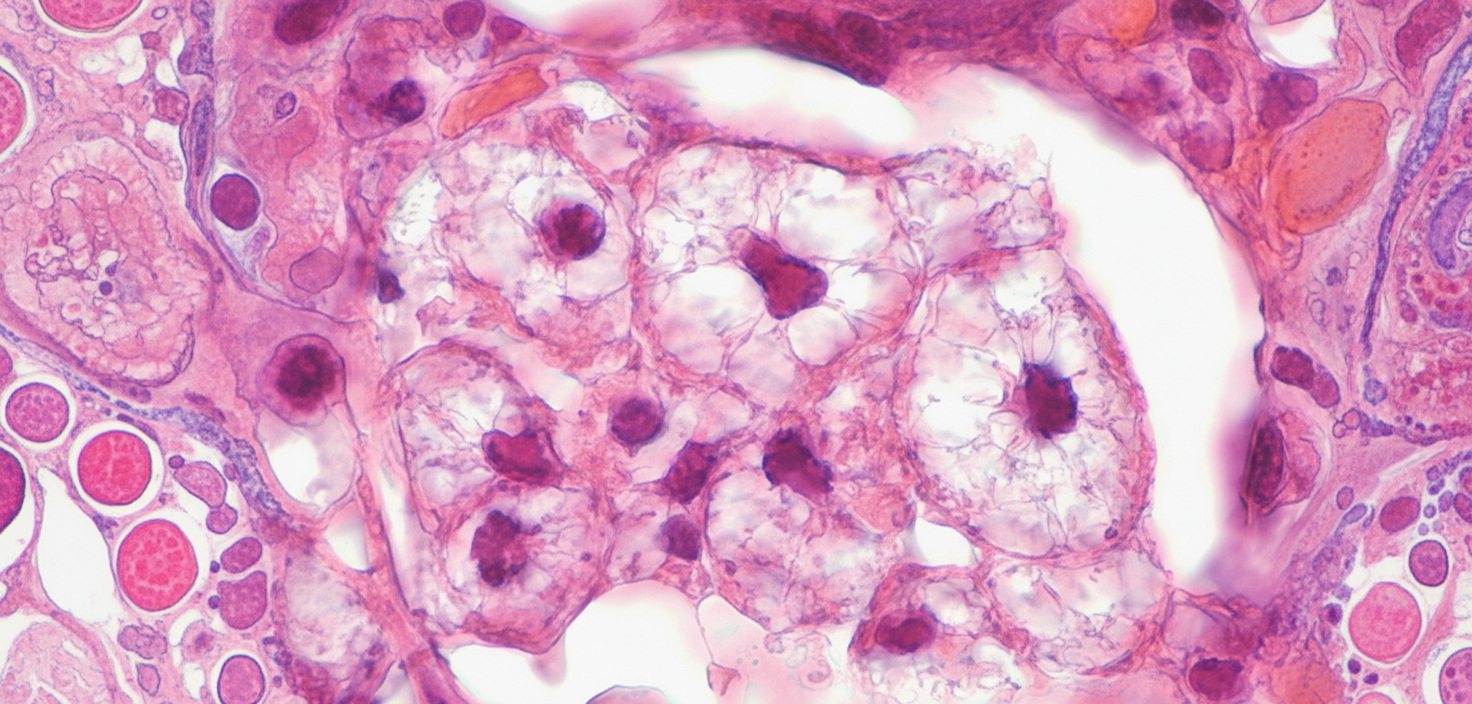
Which of the following statements are true regarding the disease depicted here?
Cottel's test is used for which of the following conditions?
Practice by Chapter
Vestibular System Anatomy and Physiology
Practice Questions
Vestibular Testing
Practice Questions
Benign Paroxysmal Positional Vertigo
Practice Questions
Ménière's Disease
Practice Questions
Vestibular Neuritis
Practice Questions
Labyrinthitis
Practice Questions
Acoustic Neuroma
Practice Questions
Other Cerebellopontine Angle Tumors
Practice Questions
Facial Nerve Disorders
Practice Questions
Skull Base Surgery
Practice Questions
Cochlear Implantation
Practice Questions
Vestibular Schwannoma Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
