Cochlear Implantation — MCQs

To distinguish between cochlear and post-cochlear damage, which test is done?
Which of the following would be the most appropriate treatment for rehabilitation of a patient, who has bilateral profound deafness following surgery for bilateral acoustic schwannoma?
Arrange the following in the sequence of auditory pathway: 1. Cochlear nucleus 2. Spiral ganglion 3. Superior olivary nucleus 4. Inferior colliculus 5. Medial geniculate body
A child aged 3 yrs, presented with severe sensorineural deafness was prescribed hearing aids, but showed no improvement. What is the next line of management:
Site for placing an electrode in auditory brain stem implant is?
Electrode of cochlear implant is placed in:
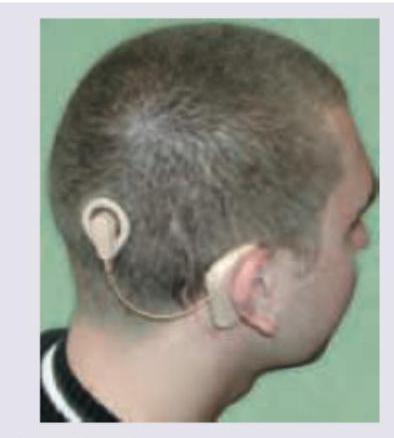
Which device is depicted below?
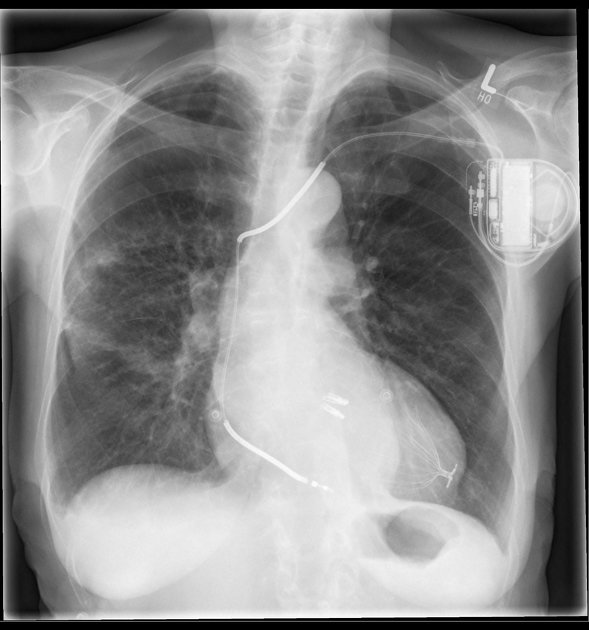
Identify the device shown in the image below:
Which of the following devices typically requires the most stringent safety protocols before MRI scanning?
A false positive fistula test is associated with which of the following conditions?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
