Neurotology — MCQs

On this page
A false positive fistula test is associated with which of the following conditions?
A 10-year-old boy presented with sensorineural deafness not benefited with a hearing aid. What is the next treatment?
A glomus tumor is invading the visceral part of the carotid canal. It is classified as which type?
Common presenting manifestations of Meniere's disease are all except?
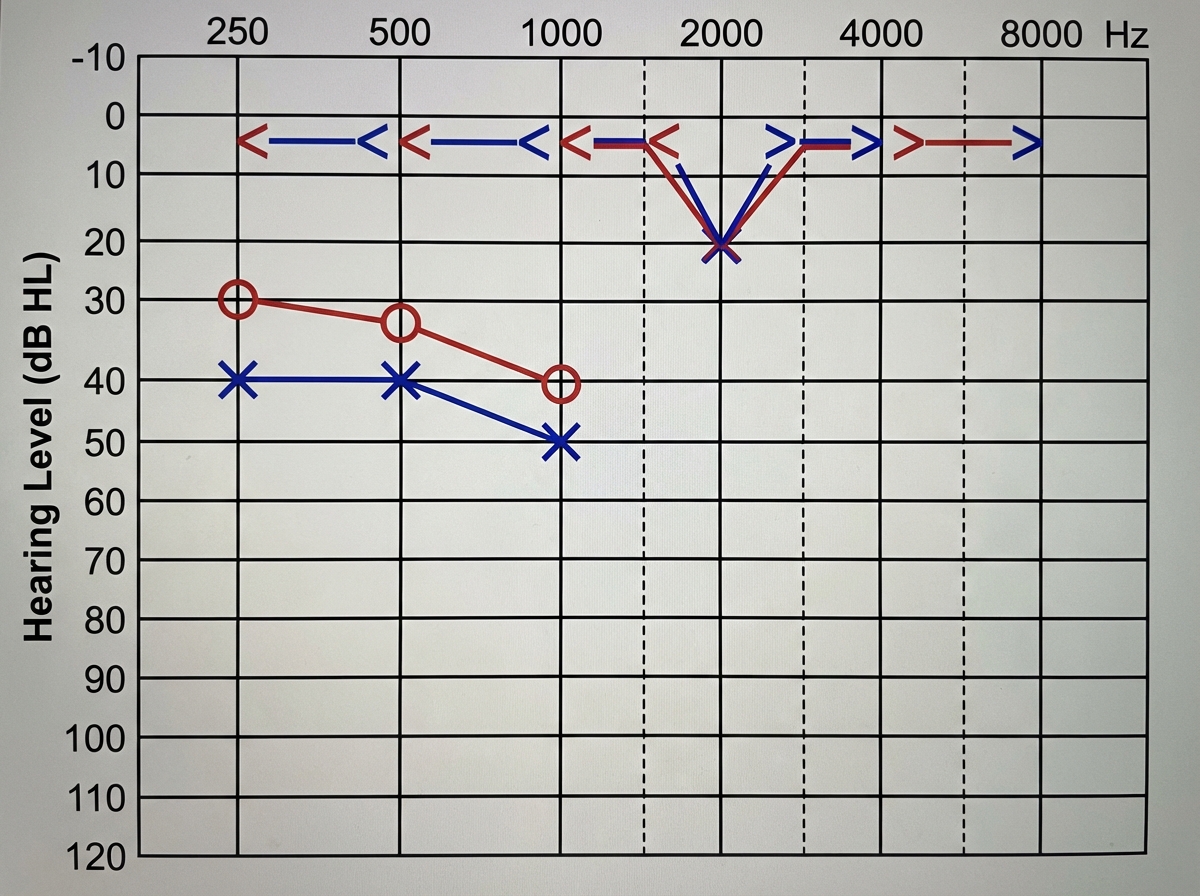
A 28-year-old female presents with a history of bilateral hearing loss and tinnitus. She reports hearing better in noisy environments. Examination reveals intact ear drums bilaterally, and the Rinne test is negative bilaterally. Pure tone audiometry findings are provided below. What is the most probable diagnosis?
Practice by Chapter
Vestibular System Anatomy and Physiology
Practice Questions
Vestibular Testing
Practice Questions
Benign Paroxysmal Positional Vertigo
Practice Questions
Ménière's Disease
Practice Questions
Vestibular Neuritis
Practice Questions
Labyrinthitis
Practice Questions
Acoustic Neuroma
Practice Questions
Other Cerebellopontine Angle Tumors
Practice Questions
Facial Nerve Disorders
Practice Questions
Skull Base Surgery
Practice Questions
Cochlear Implantation
Practice Questions
Vestibular Schwannoma Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
