Complications in Head and Neck Surgery — MCQs

One of the most important complication of tracheostomy is:
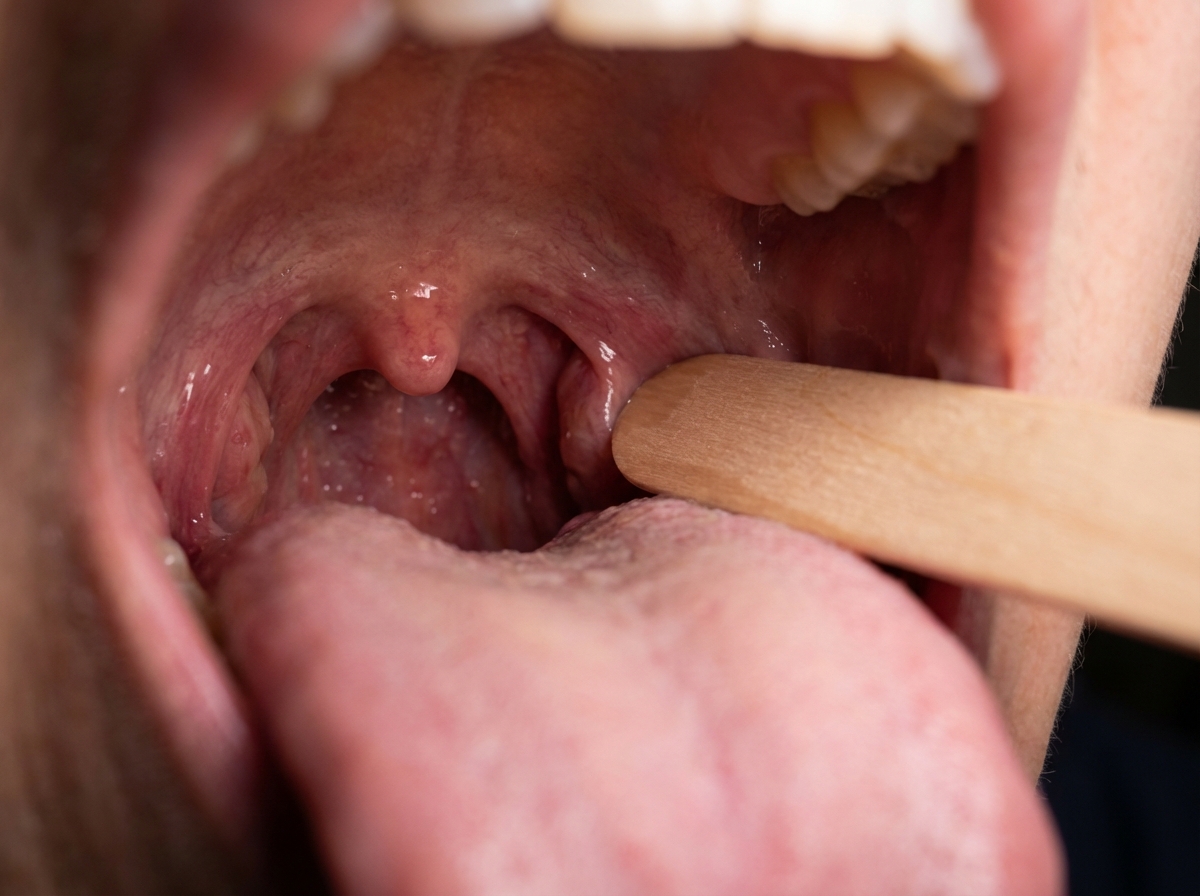
A patient was admitted with skull base trauma. The doctor was testing the marked structure in the pharyngeal region. Which of the following nerves was being tested?
A patient has a lacerated, untidy wound of the leg and attended the casualty department after 2 hours. His wound should be:
Frey's syndrome is associated with-
Which of the following statements is false regarding postpartum hemorrhage and pelvic hematomas?
Reactionary Hemorrhage occurs due to?
Carcinoma of pyriform fossa usually presents with :
In patient of head injuries with rapidly increasing intracranial tension without hematoma, the drug of choice for initial management would be :
Which of the following is not directly implicated as a cause of squamous cell carcinoma of the head and neck?
Burns involving the head and neck region are particularly dangerous because :
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
