Facial Scar Revision — MCQs

Wound contraction can be most effectively minimized by:
At what time is significant fibrous scar formation complete in myocardial infarction?
When osseous defects amenable to reconstruction are present, technique of choice is?
Which anatomical structure is most commonly the target of incisions during major gynecological surgical procedures?
What is the ideal angle for Z-plasty?
Gold standard procedure to reduce recurrence of pterygium after surgical excision is
Most common complication of mastectomy is:
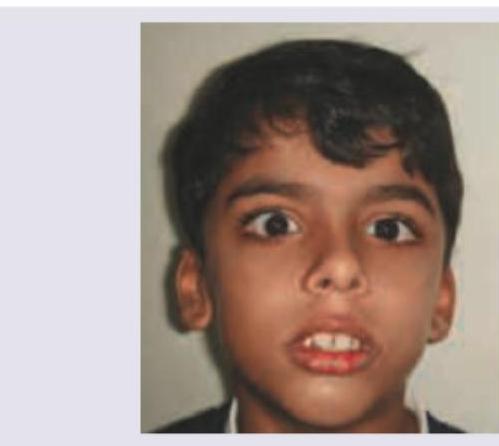
The facial features shown in the image are characteristic of:
A 35-year-old woman underwent rhinoplasty 6 months ago and now presents with nasal valve collapse and breathing difficulty. Examination shows pinched nasal tip and alar retraction. Preoperative photos show she had thin skin and weak lower lateral cartilages. Evaluate the most likely cause and best preventive strategy.
A 40-year-old man with total nasal reconstruction using paramedian forehead flap develops partial flap necrosis at the tip on post-op day 5. Doppler shows absent flow in distal 1 cm. Previous history reveals he is a heavy smoker (20 cigarettes/day). What would be the best surgical strategy if this procedure were to be revised?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
