Tonsillitis — MCQs

A patient presented with 2 days history of fever. On examination there was a swelling in the neck and one side tonsil was pushed to midline. What is the most likely diagnosis:-
Acute tonsillitis affects which nerve:
A 21-year-old college student presents with hot potato voice and trismus. Clinical diagnosis is?
What is the most common cause of acute tonsillitis?
A 12-year-old boy develops a sore throat of 4-day duration. On examination, a yellow-grayish patch is seen over both tonsils, and a foul smell is coming from his mouth. Which non-suppurative complication is most commonly associated with streptococcal throat infections?
A patient presents with fever and dysphagia. An image shows a tonsil that is pushed medially. What is the most likely diagnosis?
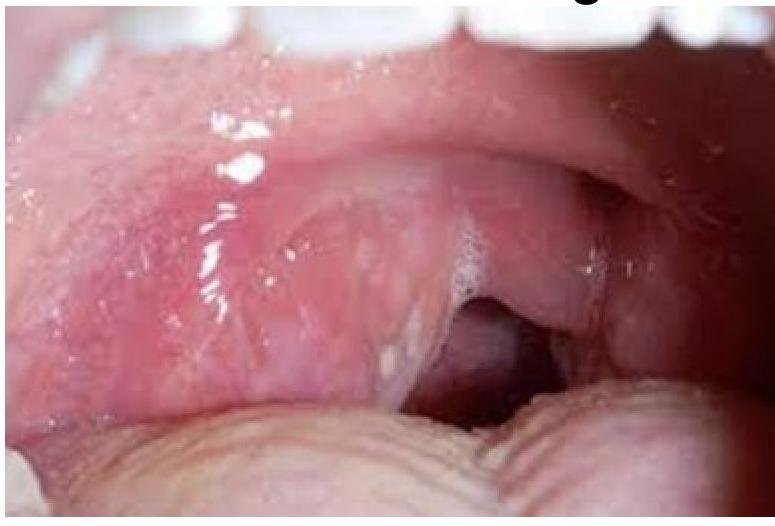
A 3-year-old boy presents with fever, throat pain, and difficulty swallowing. On examination, there is unilateral tonsillar swelling with deviation of the uvula. What is the most likely diagnosis?
A 15 years old Male presented with history of fever since 2 days, unable to swallow the food with muffled voice. On examination it is noted right tonsil is shifted to midline. What is the diagnosis:
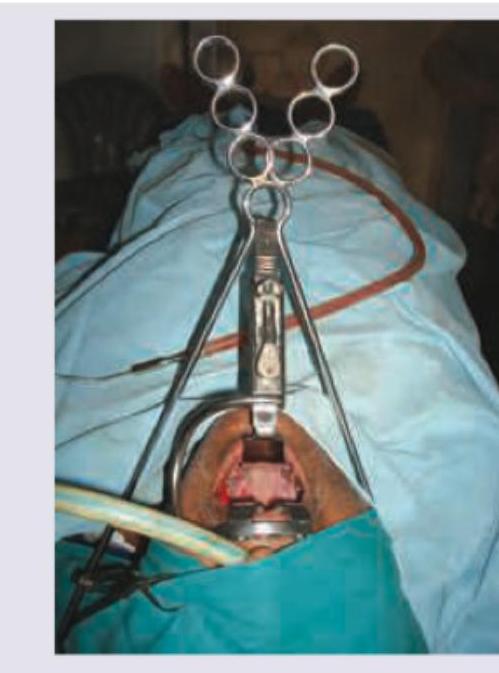
Which is incorrect about the instrument shown?
Lingual tonsils arise from which of the following processes?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
