Diseases of the Ear — MCQs

On this page
External auditory canal atresia has been associated with all of the following except?
What condition is characterized by a pulsatile tumor in the external auditory meatus that bleeds on touch?
External auditory canal exostosis occurs due to?
Which of the following ear ossicles is the first to be affected in otitis media?
Which condition is characterized by endolymphatic hydrops?
What is the earliest symptom of a glomus tumor?
Lateral sinus thrombosis is associated with all of the following except:
A 35-year-old patient presents with 6 weeks of ear discharge that is not foul-smelling. Which of the following management options is NOT indicated?
Cholesteatoma commonly perforates which structure?
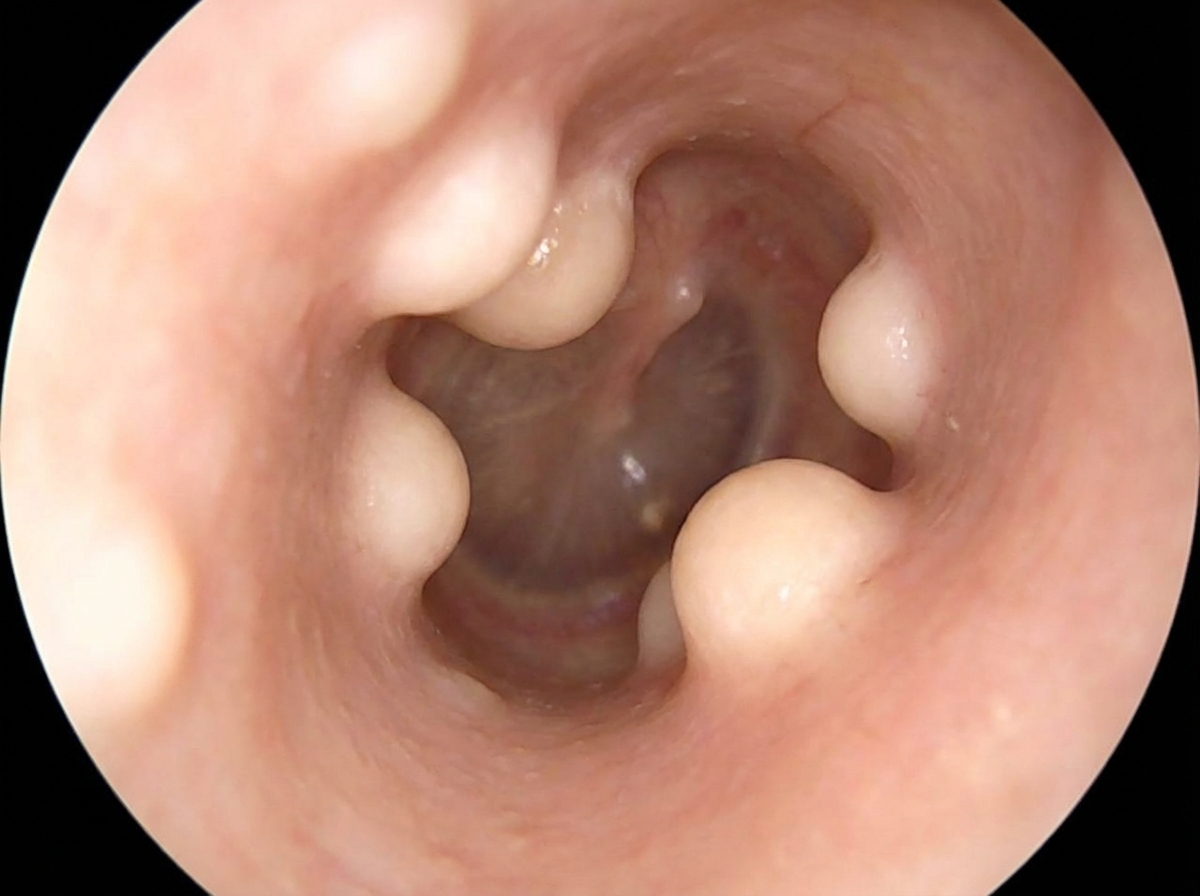
What is the diagnosis?
Practice by Chapter
Otitis Externa
Practice Questions
Acute Otitis Media
Practice Questions
Chronic Otitis Media
Practice Questions
Complications of Otitis Media
Practice Questions
Otosclerosis
Practice Questions
Presbycusis
Practice Questions
Sudden Sensorineural Hearing Loss
Practice Questions
Noise-Induced Hearing Loss
Practice Questions
Ménière's Disease
Practice Questions
Benign Paroxysmal Positional Vertigo
Practice Questions
Vestibular Neuritis
Practice Questions
Tumors of the Ear and Temporal Bone
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
