Audiology and Speech Disorders — MCQs

On this page
Carhart's notch is typically observed at which frequency?
What is the initial screening test for newborn hearing disorder?
All are true about electrocochleography except?
All are true about stapedial reflex except?
Which of the following conditions causes the maximum hearing loss?
Otoacoustic emissions arise from which structures?
Auditory fatigue commonly occurs at which frequency range?
Rinne's test negative is seen in which of the following conditions?
Which of the following is not a cause of conductive hearing loss?
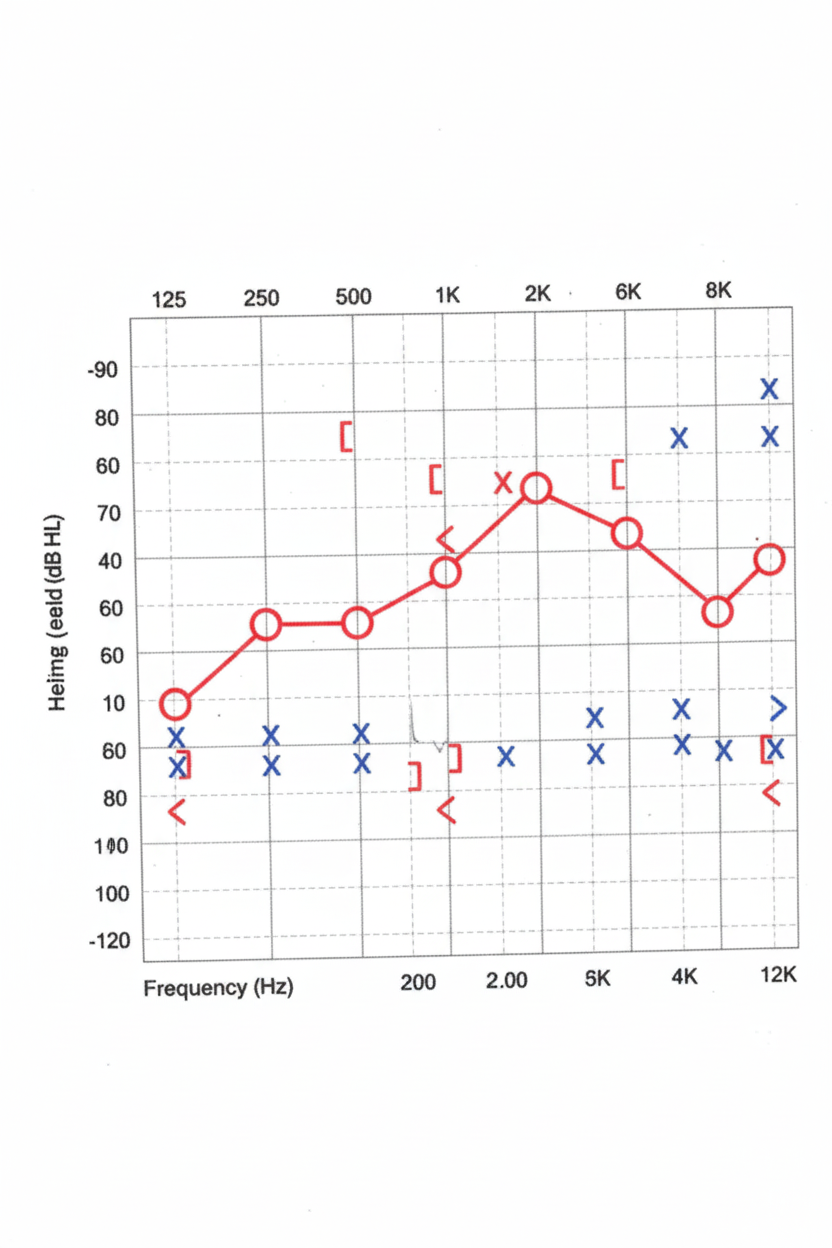
A 30-year-old female presents with hearing loss. An audiogram is obtained. What is her most likely diagnosis?
Practice by Chapter
Hearing Assessment Techniques
Practice Questions
Tympanometry and Acoustic Reflexes
Practice Questions
Otoacoustic Emissions
Practice Questions
Auditory Brainstem Response
Practice Questions
Hearing Aids
Practice Questions
Cochlear Implants
Practice Questions
Bone-Anchored Hearing Devices
Practice Questions
Speech and Language Development
Practice Questions
Articulation Disorders
Practice Questions
Stuttering
Practice Questions
Dysphonia
Practice Questions
Rehabilitation of Hearing-Impaired Children
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
