Audiology and Speech Disorders — MCQs

On this page
All of the following structures are involved in conductive deafness except?
In the Bing test, upon alternately compressing and releasing the external acoustic meatus, if the sound increases, what does this indicate?
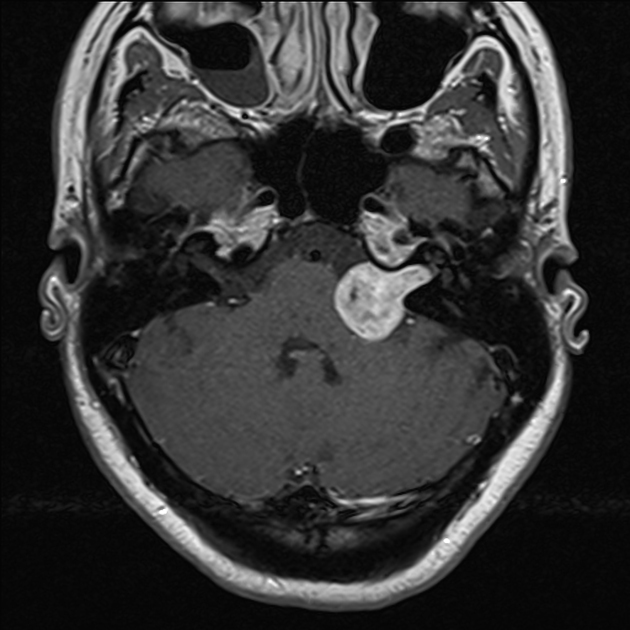
A patient presents with unilateral sensorineural hearing loss and the MRI findings are as shown. What is the most probable diagnosis?
What is the sound intensity required to elicit stapedial reflexes?
Which frequency is primarily affected in noise-induced hearing loss?
Which of the following conditions will result in the maximum conductive hearing loss?
Cochlear implants are used for which of the following conditions?
The Bing test is used to assess which of the following?
Otoacoustic emissions arise from?
Intensity of sound is measured in:
Practice by Chapter
Hearing Assessment Techniques
Practice Questions
Tympanometry and Acoustic Reflexes
Practice Questions
Otoacoustic Emissions
Practice Questions
Auditory Brainstem Response
Practice Questions
Hearing Aids
Practice Questions
Cochlear Implants
Practice Questions
Bone-Anchored Hearing Devices
Practice Questions
Speech and Language Development
Practice Questions
Articulation Disorders
Practice Questions
Stuttering
Practice Questions
Dysphonia
Practice Questions
Rehabilitation of Hearing-Impaired Children
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
