Audiology and Speech Disorders — MCQs

On this page
Which is the best screening test to evaluate hearing in a neonate?
Pendred syndrome is due to a defect in:
Which cells of the Organ of Corti are vulnerable to noise-induced damage?
At which sound level is pain experienced?
All of the following are subjective tests for audiometry except:
A tympanometry graph is shown below. An arrow indicates a shallow peak at pressure = 0 daPa. What is the most likely diagnosis based on the tympanometry result shown?
A patient presents to the OPD with hearing loss. On examination: - Rinne test - Positive in the left ear and negative in the right ear - Weber's test - lateralization towards the left - Bone conduction test - Reduced in the right ear and similar in the left ear. Interpret the findings.
Choose the most appropriate candidates for cochlear implants: 1. Ototoxicity 2. Congenital hearing loss 3. Ossicular fixation 4. Otosclerosis
Which of the following is true about the image provided?

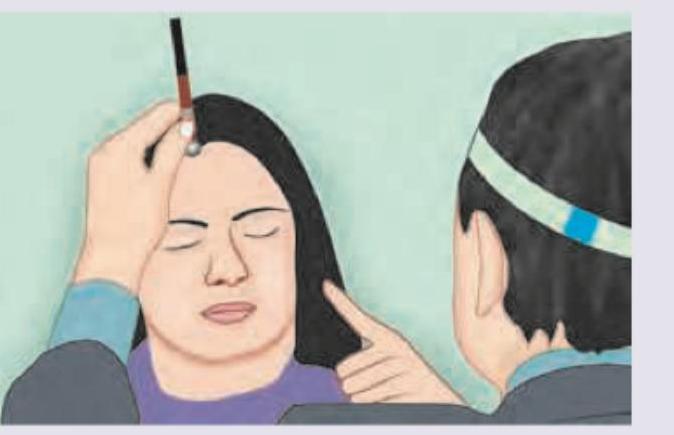
Which of the following best describes the principle of the test being performed?
Practice by Chapter
Hearing Assessment Techniques
Practice Questions
Tympanometry and Acoustic Reflexes
Practice Questions
Otoacoustic Emissions
Practice Questions
Auditory Brainstem Response
Practice Questions
Hearing Aids
Practice Questions
Cochlear Implants
Practice Questions
Bone-Anchored Hearing Devices
Practice Questions
Speech and Language Development
Practice Questions
Articulation Disorders
Practice Questions
Stuttering
Practice Questions
Dysphonia
Practice Questions
Rehabilitation of Hearing-Impaired Children
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
