Viral Skin Infections — MCQs

On this page
A 45-year-old male has multiple grouped vesicular lesions present on the T10 dermatome associated with pain. What is the most likely diagnosis?
Which of the following lesions is NOT an infection caused by human papilloma virus?
In Tzanck smear, multinucleated cells are seen in which of the following conditions?
What is the causative agent of hairy leukoplakia, a condition characterized by severe discomfort on the lateral part of the tongue?
A 69-year-old man presents with a gradual onset of pain, tingling, and hyperesthesia in the medial aspect of his right arm. Subsequently, he develops erythema and an outbreak of vesicles on the medial aspect of his right arm, extending from his medial epicondyle to the wrist. After several days, the lesions crust over and resolve, but he is left with a residual "burning" pain in the same distribution as the lesions, with occasional sharp pain provoked by touch. The infectious agent responsible for this condition resides in which part of the neuraxis?
Scrum pox is typically seen in athletes participating in which sport?
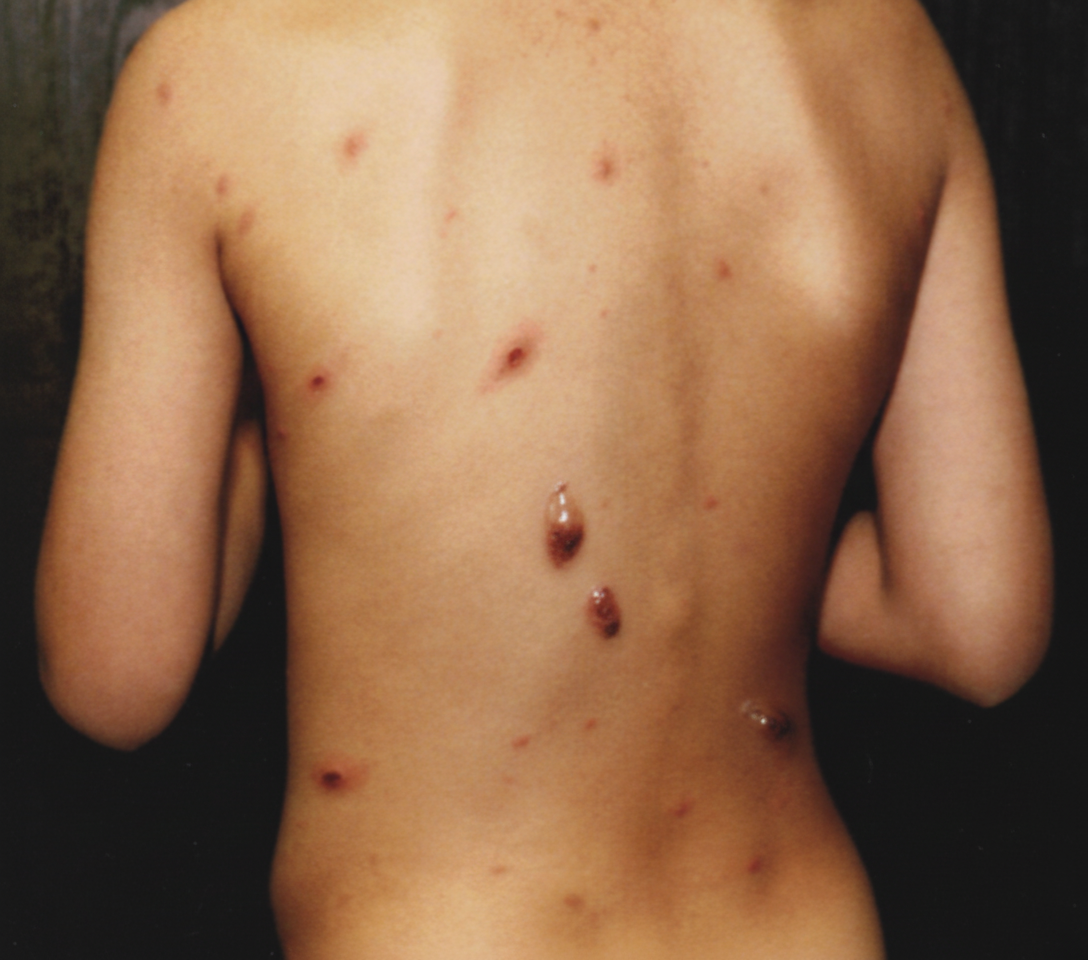
Infection by which virus gives rise to the following skin lesions?
What is the treatment of choice for genital warts in pregnancy?
A 23-year-old, sexually active man has been treated for Neisseria gonorrhoeae infection 6 times during the past 5 years. He now comes to the physician because of the increasing number and size of warty lesions slowly enlarging on his external genitalia during the past year. On physical examination, there are multiple 1- to 3-mm sessile, nonulcerated, papillary excrescences over the inner surface of the penile prepuce. These lesions are excised, but 2 years later, similar lesions appear. Which of the following conditions most likely predisposed him to the development of these recurrent lesions?
Tzank smear helps in the diagnosis of which of the following conditions?
Practice by Chapter
Herpes Simplex Virus Infections
Practice Questions
Varicella-Zoster Virus Infections
Practice Questions
Human Papillomavirus Infections
Practice Questions
Molluscum Contagiosum
Practice Questions
Viral Exanthems
Practice Questions
Hand, Foot, and Mouth Disease
Practice Questions
Orf and Milker's Nodule
Practice Questions
Cytomegalovirus Cutaneous Manifestations
Practice Questions
Epstein-Barr Virus Manifestations
Practice Questions
Poxvirus Infections
Practice Questions
HIV-Related Dermatoses
Practice Questions
Viral Infections in Immunocompromised Hosts
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
