Tropical Dermatology — MCQs

On this page
A 65-year-old beggar comes to your OPD with following presentation in upper part of foot Gram stain of discharge was performed. All are true about the condition shown except:
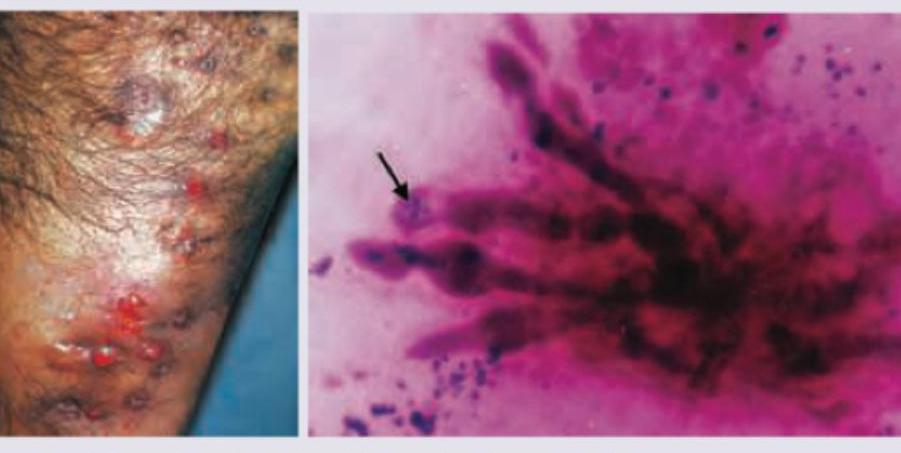
A young male presented with an anesthetic patch on the right forearm. A thickened nerve was palpable on examination. Skin biopsy shows the image below. What is the diagnosis?
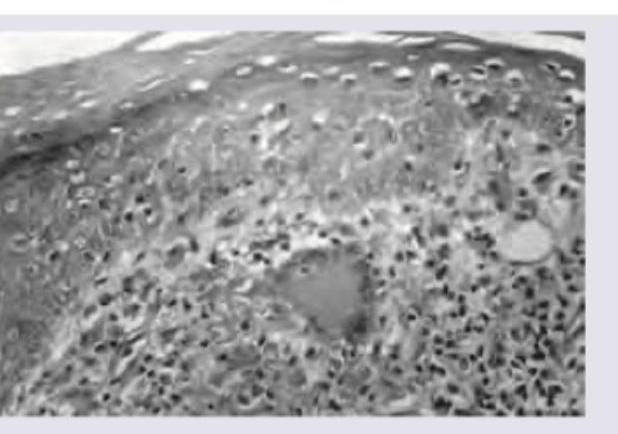
All are true about the lesion shown except:
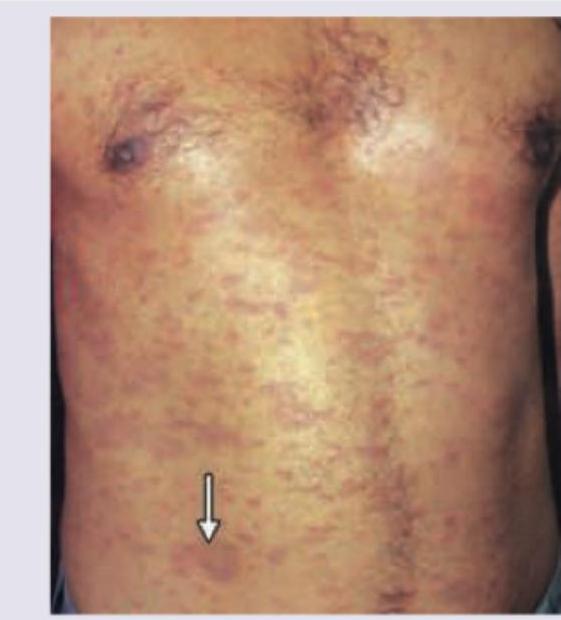
A patient lives in an urban slum and practices open-air defecation. He presented with continuous itching over the sole. The image shows presence of:
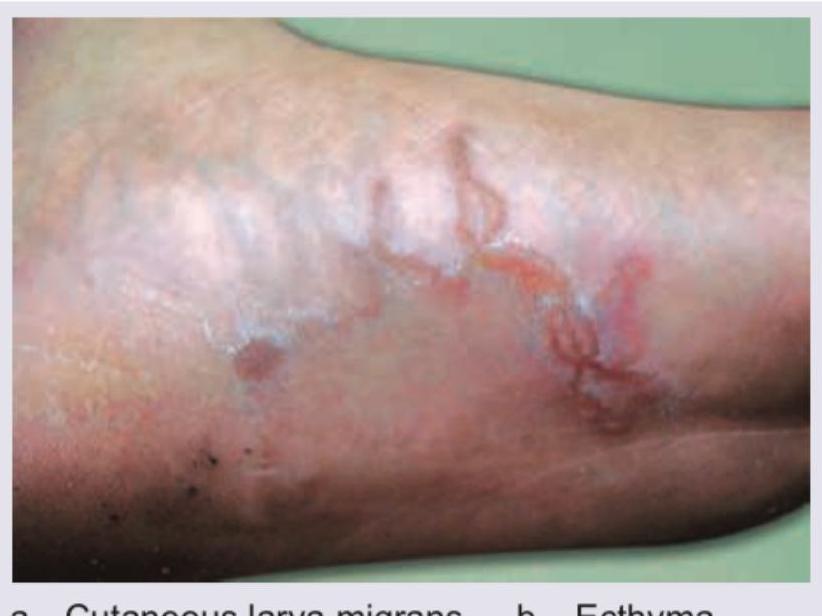
A 53 year-old male presented with erythematous, edematous plaques on his face over pre-existing hypoesthetic patches. He has been experiencing pain for the last 10 days and has been on multibacillary multidrug therapy (MBMDT) for leprosy for the past two months. What is the most likely diagnosis based on the image?
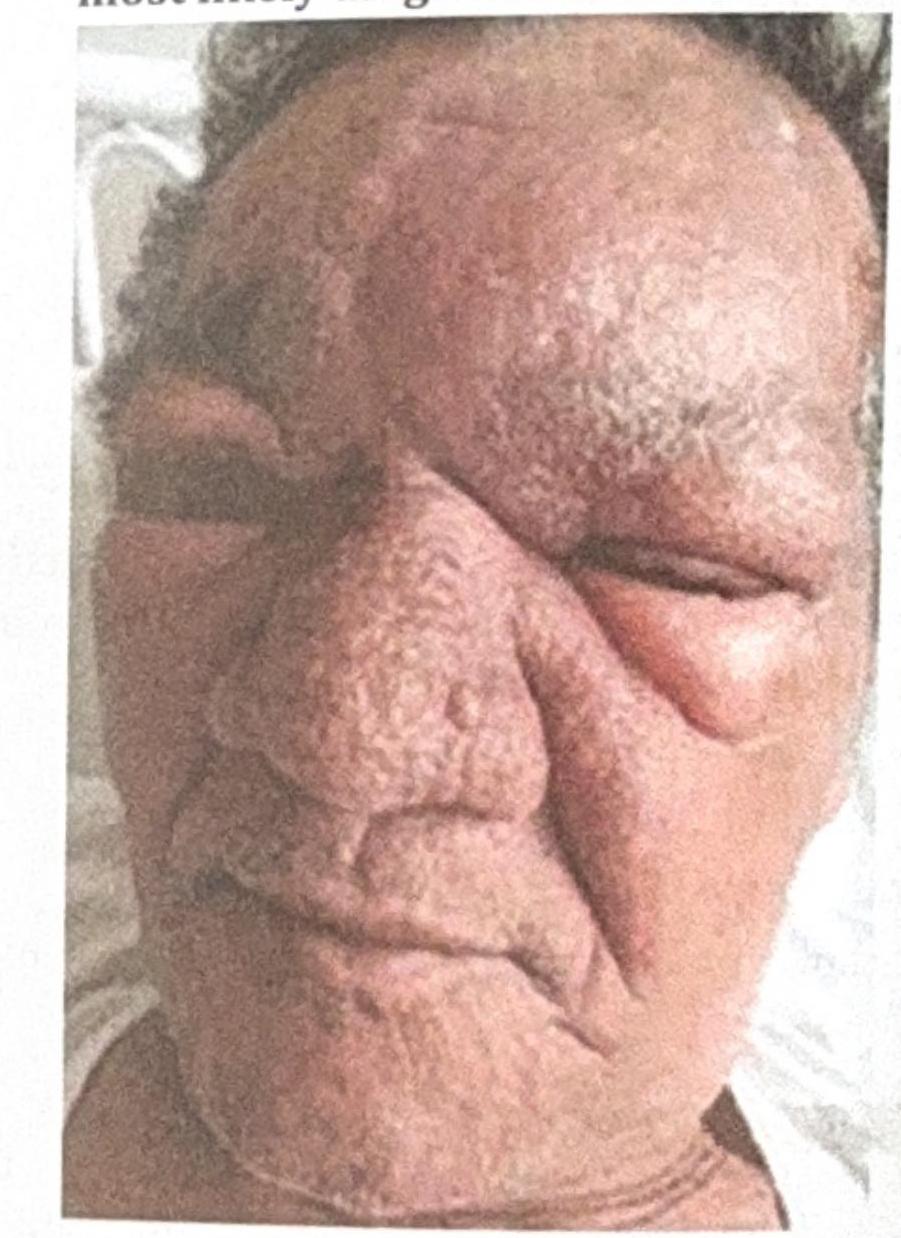
A 12-week pregnant woman on multidrug therapy for leprosy presents with type 2 lepra reaction. What is the treatment of choice for this patient?
Single skin lesion is seen in which type of leprosy -
Multiple hypoaesthetic, hypopigmented macules on right lateral forearm with numerous acid-fast bacilli is indicative of:
A 45-year-old male had multiple hypoesthetic, mildly erythematous large plaques with elevated margins on trunk and extremities. His ulnar and lateral popliteal nerves on both sides were enlarged. The most probable diagnosis is:
Punched out lesion or inverted saucer appearance are characteristic of which type of leprosy?
Practice by Chapter
Cutaneous Leishmaniasis
Practice Questions
Leprosy
Practice Questions
Tropical Ulcers
Practice Questions
Onchocerciasis
Practice Questions
Filariasis
Practice Questions
Tropical Mycoses
Practice Questions
Cutaneous Larva Migrans
Practice Questions
Tungiasis
Practice Questions
Myiasis
Practice Questions
Cutaneous Manifestations of Malaria
Practice Questions
Dengue and Other Viral Hemorrhagic Fevers
Practice Questions
Global Health Perspectives in Dermatology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
