Tropical Dermatology — MCQs

On this page
A 48-year-old male presents with a three-month history of non-itchy, generalized papulo-nodular lesions. Physical examination reveals no other abnormalities. Slit smear from a nodule is negative for acid-fast bacilli (AFB). Blood VDRL is reactive at a 1:2 dilution. What is the most likely diagnosis?
Erythema nodosum leprosum is seen in a 16-year-old boy. This is a feature of which of the following types of leprosy?
Which of the following statements about mycetoma is false?
A 27-year-old patient was diagnosed to have borderline leprosy and started on multidrug therapy for multibacillary leprosy. Six weeks later, he developed pain in the nerves and redness and swelling of the skin lesions. The management of his illness should include all of the following, except?
In Hansen's disease, which nerve is commonly affected at the elbow?
Which of the following are clinical features of lepromatous leprosy?
A patient with leprosy presents with clumsiness of the hand due to ulnar nerve involvement. Palsy of which muscle group would cause this clumsiness?
A 20-year-old male from Jaipur presents with an erythematous lesion on his cheek with central crusting. What is the likely diagnosis?
Which of the following is characteristic of donovanosis?
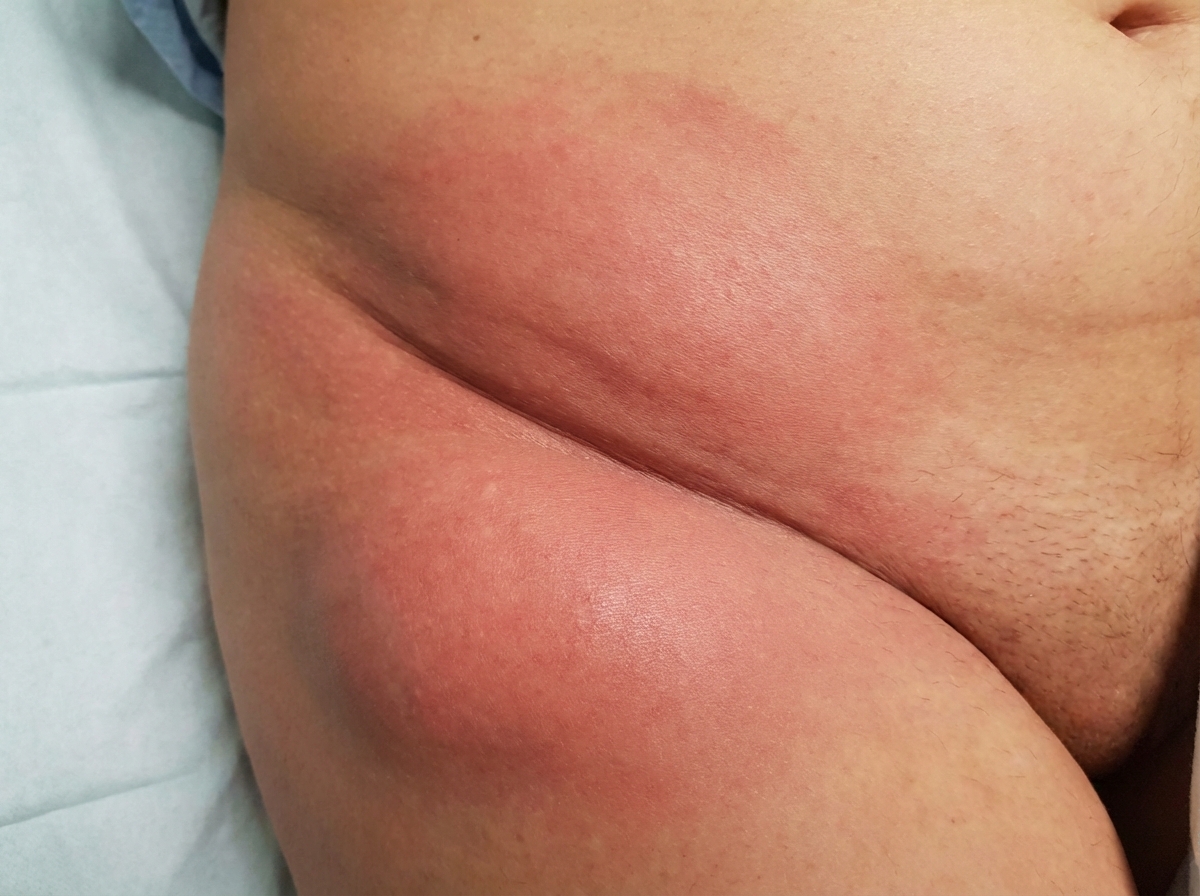
The inguinal region shown in the image is characteristic of which of the following conditions?
Practice by Chapter
Cutaneous Leishmaniasis
Practice Questions
Leprosy
Practice Questions
Tropical Ulcers
Practice Questions
Onchocerciasis
Practice Questions
Filariasis
Practice Questions
Tropical Mycoses
Practice Questions
Cutaneous Larva Migrans
Practice Questions
Tungiasis
Practice Questions
Myiasis
Practice Questions
Cutaneous Manifestations of Malaria
Practice Questions
Dengue and Other Viral Hemorrhagic Fevers
Practice Questions
Global Health Perspectives in Dermatology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
