Skin Tumors — MCQs

On this page
Necrobiosis lipoidica is a clinical finding associated with which of the following conditions?
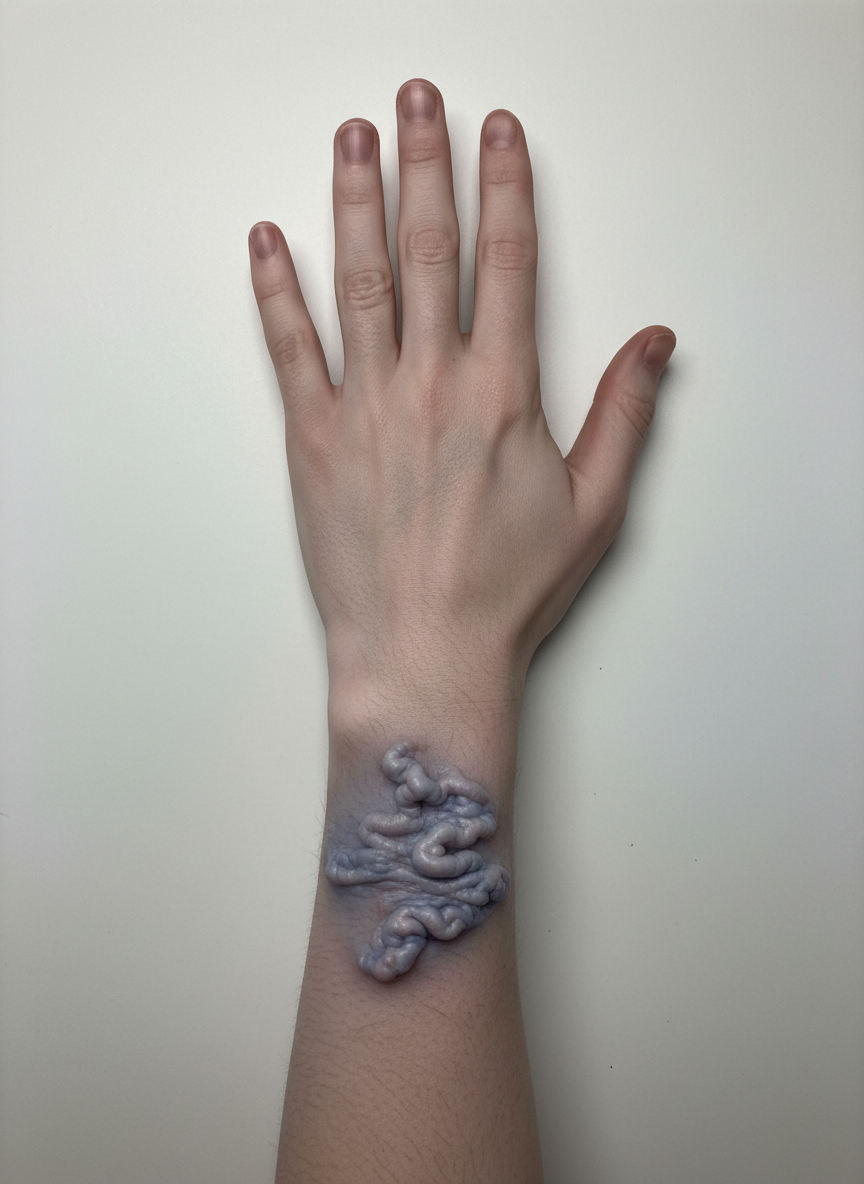
Which of the following conditions is depicted?
What is the most common origin of melanoma?
Prognosis of malignant melanoma depends upon:
Plexiform neurofibromatosis commonly affects which of the following nerves?
Which of the following is a slow-growing skin tumor that rarely metastasizes to lymph nodes?
Increased incidence of carcinoma is observed with which of the following conditions?
Regarding malignant melanoma, all the following are true EXCEPT?
What is the treatment for Stage I mycosis fungoides?
A 50-year-old male presented with a characteristic lesion on the face for 5 years which is slowly increasing in size and bleeds whenever it is scratched. The patient has a history of chronic sun exposure, and there is no evidence of pain or itching over the lesion. Biopsy from the lesion is performed. Which of the following drugs are approved for the above condition?
Practice by Chapter
Benign Epithelial Tumors
Practice Questions
Premalignant Epidermal Tumors
Practice Questions
Basal Cell Carcinoma
Practice Questions
Squamous Cell Carcinoma
Practice Questions
Melanocytic Nevi
Practice Questions
Melanoma
Practice Questions
Merkel Cell Carcinoma
Practice Questions
Vascular Tumors and Malformations
Practice Questions
Cutaneous Lymphomas
Practice Questions
Soft Tissue Tumors
Practice Questions
Metastatic Skin Tumors
Practice Questions
Skin Cancer Prevention and Screening
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
