Skin Tumors — MCQs

On this page
An enlarging, conical cutaneous horn that has been present for more than a year projects 0.5 cm from a 0.7-cm base on the left lateral cheek of the face of a 58-year-old farmer. This lesion is excised, and microscopic examination shows basal cell hyperplasia. Some of the basal cells show nuclear atypicalities. This is associated with marked hyperkeratosis and parakeratosis. Which of the following lesions best accounts for these findings?
Which one of the following is not included in the treatment of malignant melanoma?
Carcinoma in situ of the skin is called as:
What is the treatment of choice in solar keratosis?
Increased incidence of squamous cell carcinoma of the skin is associated with all of the following factors except:
Mycosis fungoides affects which type of cells?
What is the most common type of this malignancy?
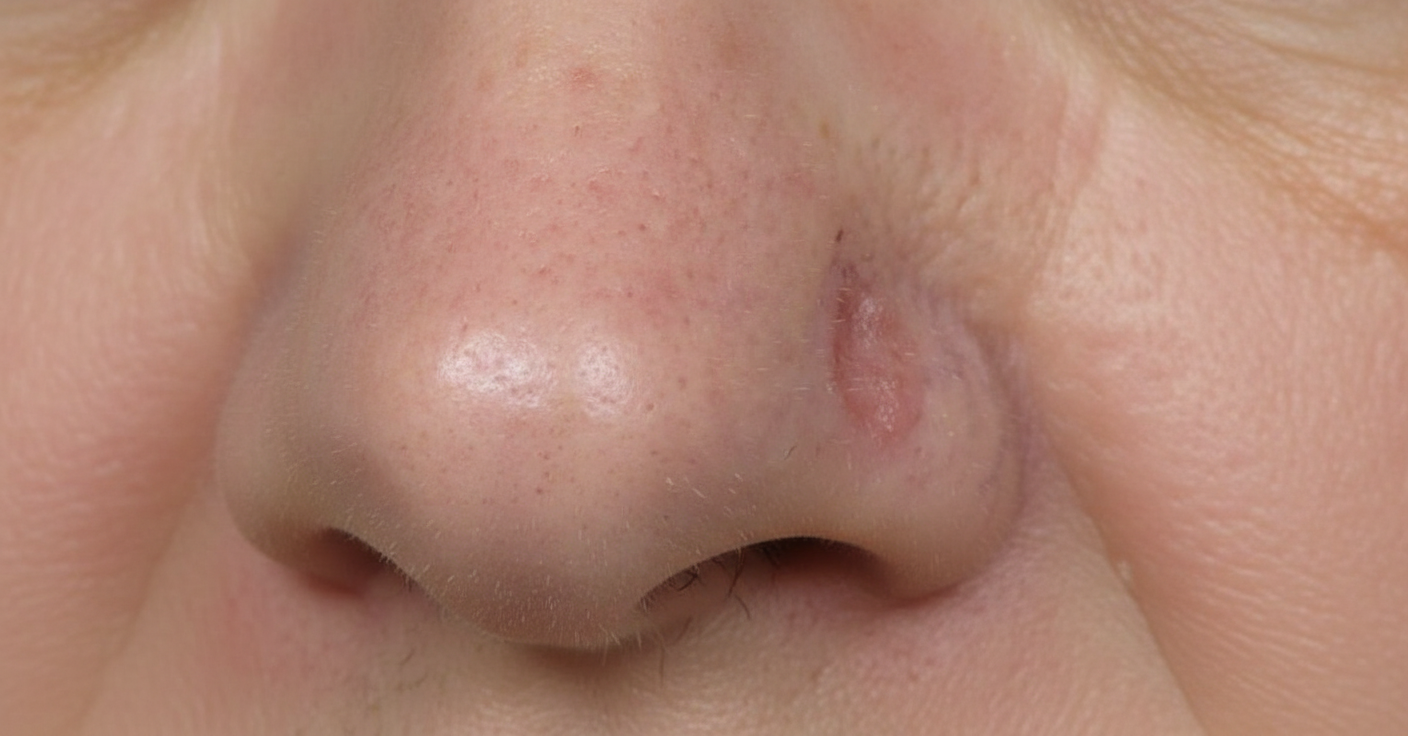
What is the most aggressive type of Basal cell carcinoma?
Which genodermal disease can cause skin malignancy?
A 40-year-old tobacco chewer presented for a routine oral examination. A non-scrapable white patch was noticed on the left buccal mucosa. What is the most likely diagnosis for this lesion?
Practice by Chapter
Benign Epithelial Tumors
Practice Questions
Premalignant Epidermal Tumors
Practice Questions
Basal Cell Carcinoma
Practice Questions
Squamous Cell Carcinoma
Practice Questions
Melanocytic Nevi
Practice Questions
Melanoma
Practice Questions
Merkel Cell Carcinoma
Practice Questions
Vascular Tumors and Malformations
Practice Questions
Cutaneous Lymphomas
Practice Questions
Soft Tissue Tumors
Practice Questions
Metastatic Skin Tumors
Practice Questions
Skin Cancer Prevention and Screening
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
