Skin Tumors — MCQs

On this page
Which of the following are premalignant conditions of the skin?
Which of the following conditions is related to sunlight exposure?
Ichthyosis may be associated with which of the following conditions?
A 22-year-old patient presents with multiple neural tumors, pigmented iris hamartomas, and numerous tan macules on his skin. His father, paternal uncle, and paternal grandfather had a similar condition. This patient likely suffers from which of the following?
What is the most common site for the acral lentigo subtype of malignant melanoma?
Which of the following best describes mycosis fungoides?
Skin cancers develop due to sunlight exposure induced by which type of radiation?
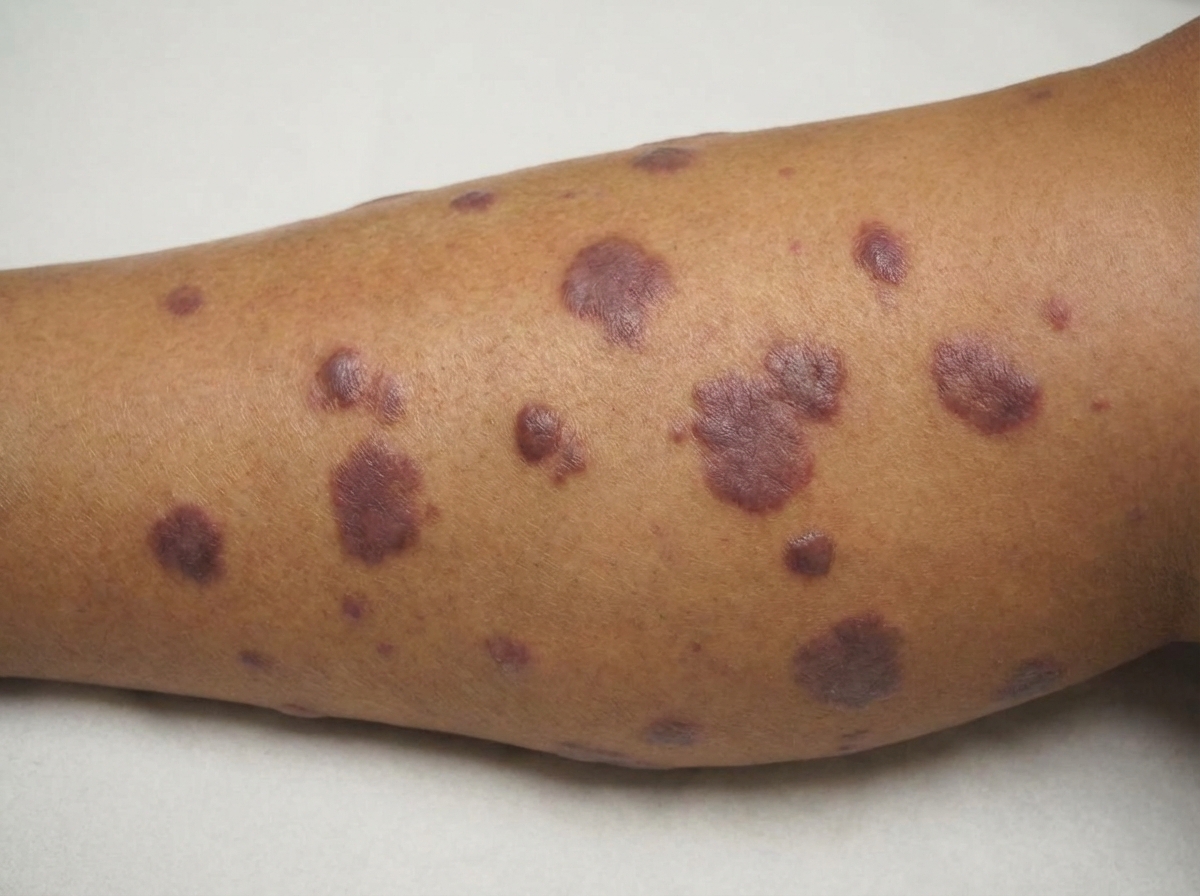
An HIV positive patient presented with the clinical condition as seen in the color plate. Which of the following is the most probable diagnosis?
What is the recommended treatment for Stage 1 cutaneous T-cell lymphoma?
A patient presents with pigmented macules on the palm. Histological examination reveals proliferating melanocytes at the dermoepidermal junction. What is the most likely diagnosis?
Practice by Chapter
Benign Epithelial Tumors
Practice Questions
Premalignant Epidermal Tumors
Practice Questions
Basal Cell Carcinoma
Practice Questions
Squamous Cell Carcinoma
Practice Questions
Melanocytic Nevi
Practice Questions
Melanoma
Practice Questions
Merkel Cell Carcinoma
Practice Questions
Vascular Tumors and Malformations
Practice Questions
Cutaneous Lymphomas
Practice Questions
Soft Tissue Tumors
Practice Questions
Metastatic Skin Tumors
Practice Questions
Skin Cancer Prevention and Screening
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
