Skin Tumors — MCQs

On this page
Pilomatrixoma is:
What is the most common malignancy observed in individuals undergoing immunosuppressive therapy?
Which of the following melanomas does not have an in situ growth phase?
Which type of carcinoma characteristically shows no or minimal metastasis?
Prognosis of malignant melanoma depends on which of the following factors?
Which of the following features is most commonly seen?
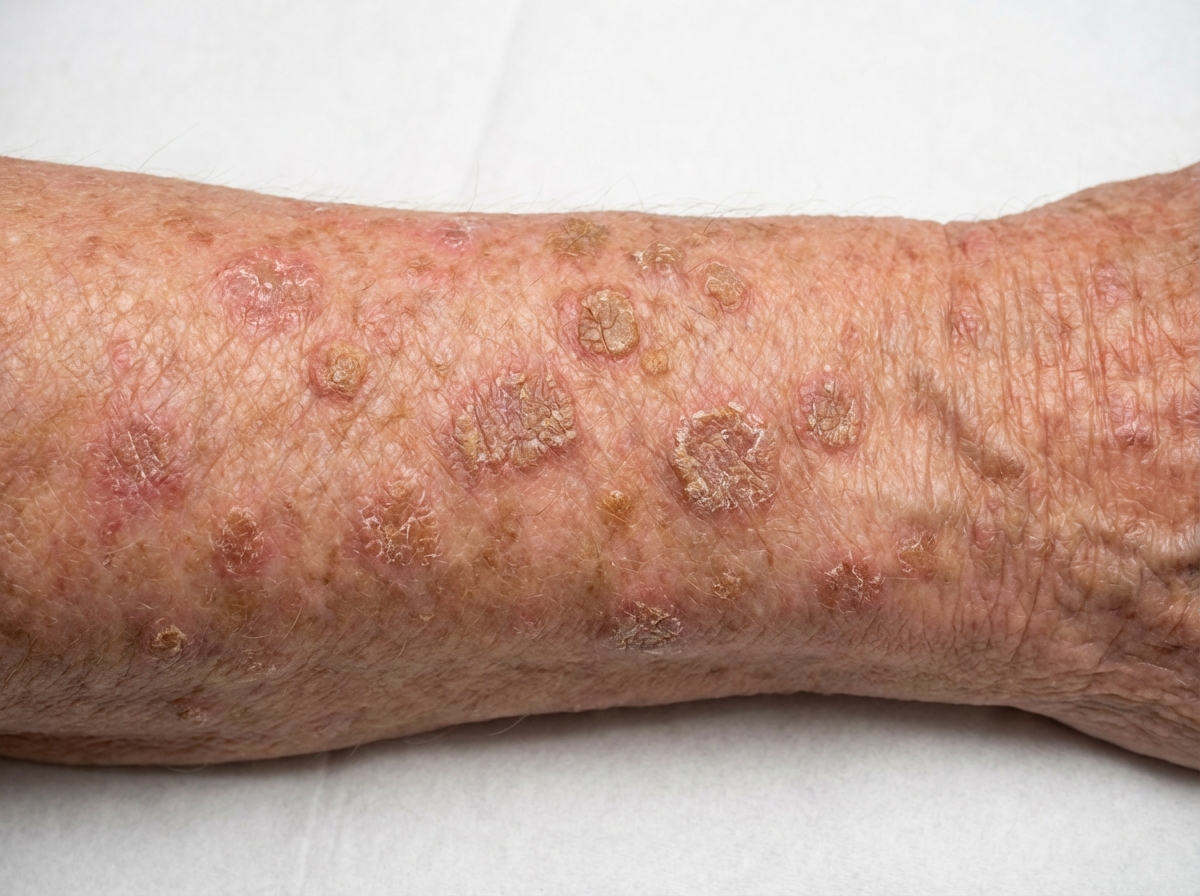
A 78-year-old woman has multiple long-standing lesions on her face and back. These well-circumscribed lesions are tan to brownish, slightly raised with a rough surface, and typically 0.5 to 1.5 cm in diameter. The clinician examining the patient is able to "peel away" parts of the lesion with the dull side of a scalpel blade. Which of the following diagnoses is most likely?
Which of the following cutaneous malignancies does not metastasize through the lymphatics?
An HIV-positive patient presents with a characteristic lesion on the leg and a history of HHV-8 infection. What is the most likely diagnosis?
Which is considered the most severe form of malignant melanoma?
Practice by Chapter
Benign Epithelial Tumors
Practice Questions
Premalignant Epidermal Tumors
Practice Questions
Basal Cell Carcinoma
Practice Questions
Squamous Cell Carcinoma
Practice Questions
Melanocytic Nevi
Practice Questions
Melanoma
Practice Questions
Merkel Cell Carcinoma
Practice Questions
Vascular Tumors and Malformations
Practice Questions
Cutaneous Lymphomas
Practice Questions
Soft Tissue Tumors
Practice Questions
Metastatic Skin Tumors
Practice Questions
Skin Cancer Prevention and Screening
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
