Skin Tumors — MCQs

On this page
What is the most common type of nevus found in the oral cavity?
In the Clarke's levels of tumor invasion of malignant melanoma, level 3 refers to which layer of the skin?
All of the following statements regarding actinic keratosis are true, EXCEPT:
Most severe type of malignant melanoma most commonly arises from which of the following?
What is the vertical measurement in millimeters from the granular cell layer to the deepest part of a tumor used in melanoma for prognosis?
Which condition is characterized by the following lesion?
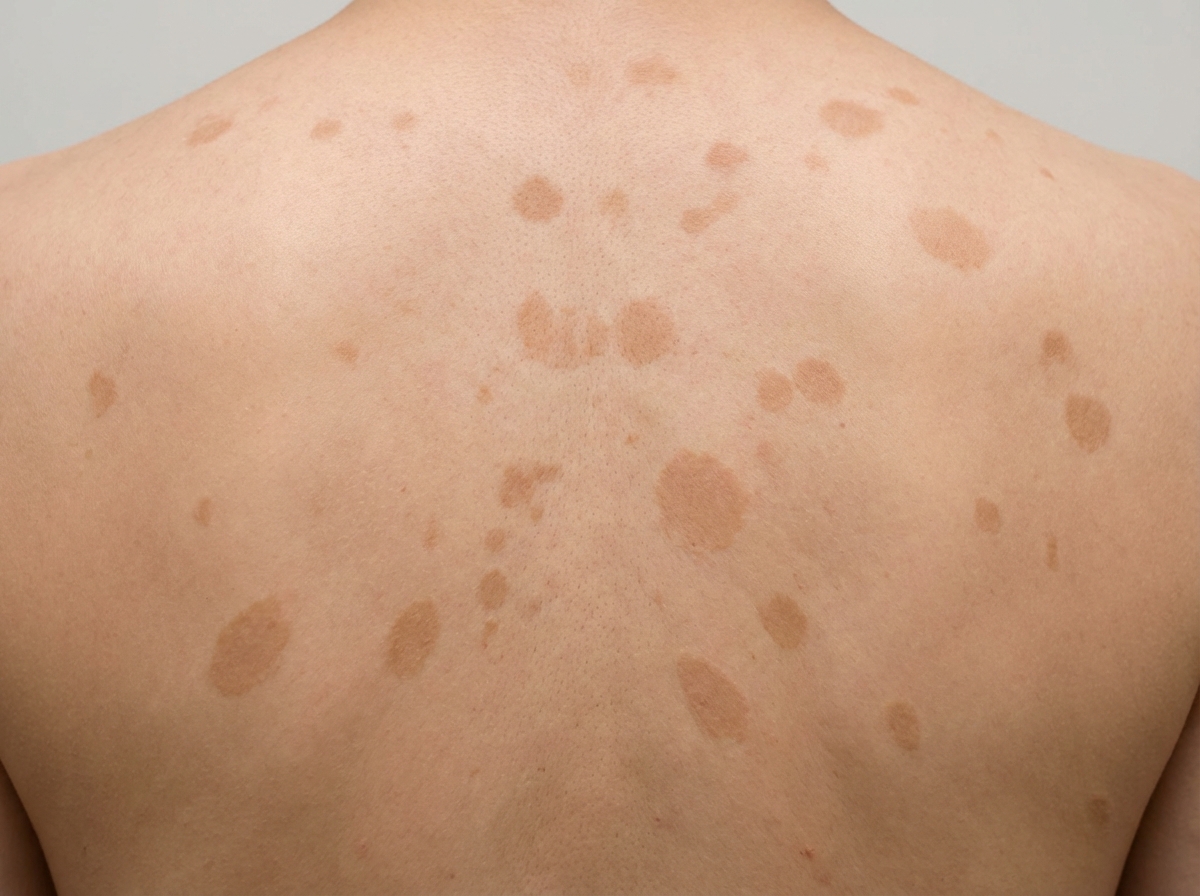
Actinic keratosis is a precursor to which of the following malignancies?
Mycosis fungoides is a type of:
Which of the following is considered the least malignant melanoma?
Acanthosis nigricans is a known paraneoplastic sign associated with which of the following conditions?
Practice by Chapter
Benign Epithelial Tumors
Practice Questions
Premalignant Epidermal Tumors
Practice Questions
Basal Cell Carcinoma
Practice Questions
Squamous Cell Carcinoma
Practice Questions
Melanocytic Nevi
Practice Questions
Melanoma
Practice Questions
Merkel Cell Carcinoma
Practice Questions
Vascular Tumors and Malformations
Practice Questions
Cutaneous Lymphomas
Practice Questions
Soft Tissue Tumors
Practice Questions
Metastatic Skin Tumors
Practice Questions
Skin Cancer Prevention and Screening
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
