Metastatic Skin Tumors — MCQs

What is the most common primary source of metastatic bone tumors in males?
Which of the following statements about bone metastasis is false?
Clinical examination of a symptomatic patient shows a Sister Mary Joseph nodule. It is most commonly associated with which of the following?
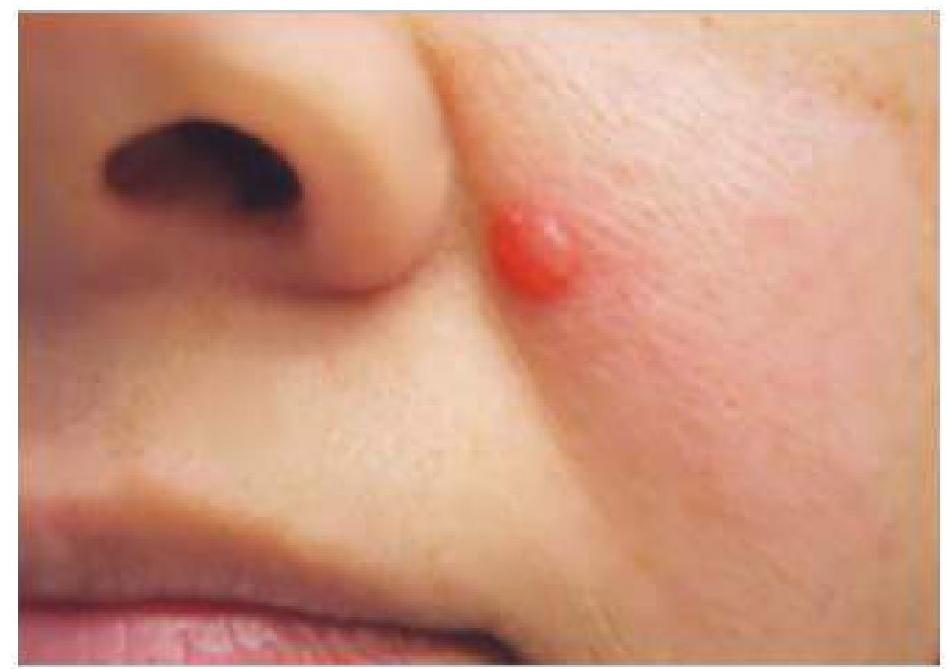
A male patient presented with a 0.3 cm nodule on the left nasolabial fold. A pathological examination revealed a basaloid appearance with peripheral palisading. What is the most likely diagnosis?
Statement 1 - A 59-year-old patient presents with flaccid bullae. Histopathology shows a suprabasal acantholytic split. Statement 2 - The row of tombstones appearance is diagnostic of Pemphigus vulgaris.
Mycosis fungoides primarily involves which type of immune cell?
A patient consults a dermatologist about a skin lesion on her neck. Examination reveals a 1-cm diameter, red, scaly plaque with a rough texture and irregular margins. Biopsy demonstrates epidermal and dermal cells with large, pleomorphic, hyperchromatic nuclei. Which of the following conditions would most likely predispose this patient to the development of this lesion?
All of the following statements are true for keloids EXCEPT:
Elderly man with a long-standing mole on his face that is increasing in size and showing an irregular border. Diagnosis:
Pautrier's microabscess is a histological feature of which disease?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
