Post-inflammatory Hyperpigmentation — MCQs

Mycosis fungoides primarily involves which type of immune cell?
False about Tinea versicolor
Recalcitrant acne is treated by:
A 35 years old female presented with acne. She was treated for her acne but after the treatment, she developed pigmentation. Which drug is responsible for hyperpigmentation?
Dermatological manifestation of which of the following diseases?

Which of the following is not true about hydroquinone?
In a patient with the following lesion on scalp, what changes are seen in the nails?
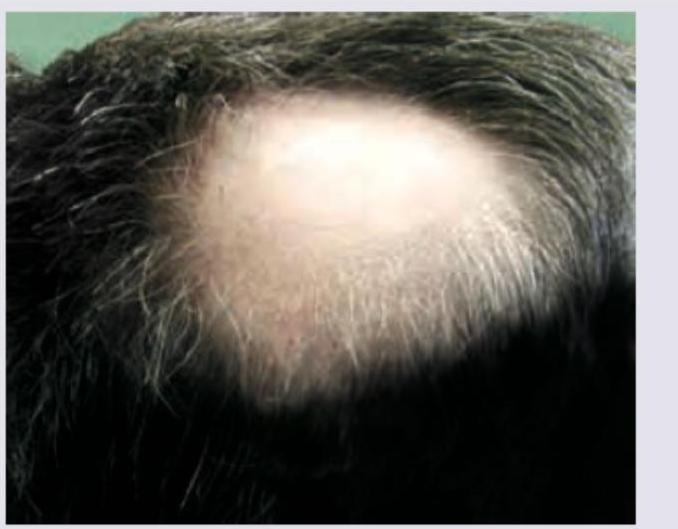
In which of the following conditions is the Koebner phenomenon most commonly observed?
What is the most common association with Acanthosis nigricans?
An increased incidence of vitiligo is found in association with which of the following conditions?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
