Pigmentary Disorders — MCQs

On this page
A 13-year-old boy presents with patchy depigmented skin on the right flank and upper thigh in segmental distribution, as shown in the image. The depigmentation started 1 year back but has been static for last 4 months. Mother reports use of topical steroids which was ineffective. Diagnosis is?
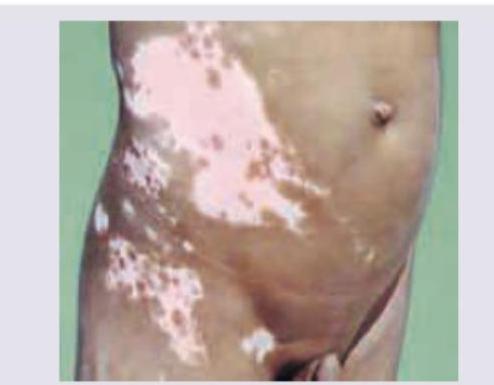
An 18-year-old female presents with hypo-pigmented patches on the dorsal aspect of the foot. Which of the following drugs should not be used in the treatment of this patient? (AIIMS May 2016)
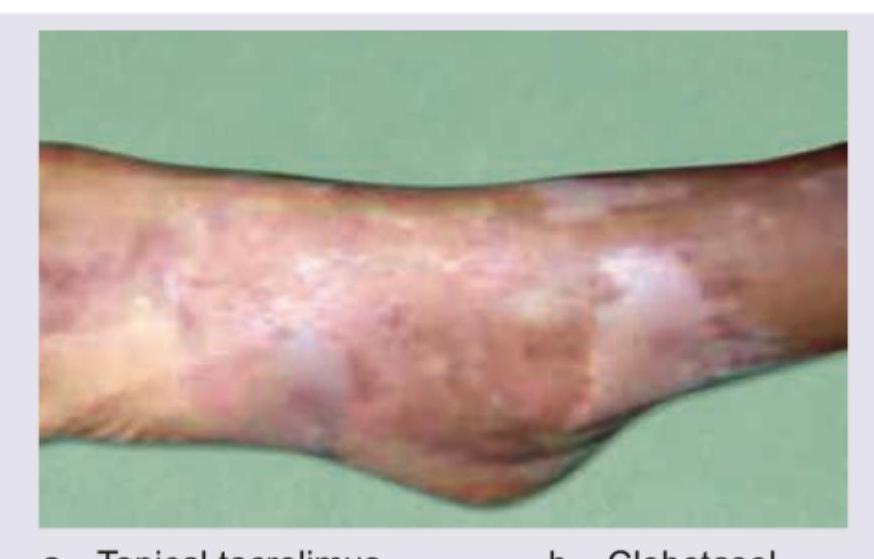
The following skin lesion can be seen in all except:
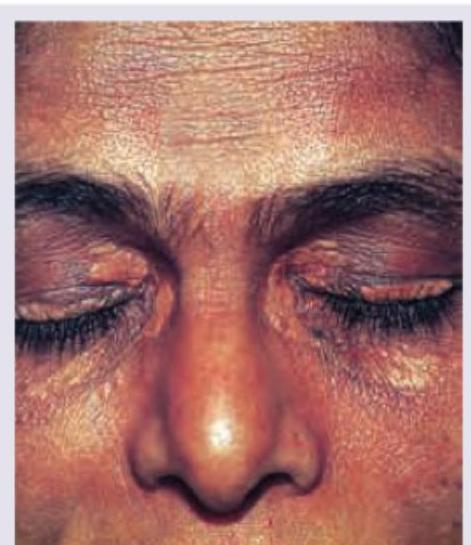
The given image shows:
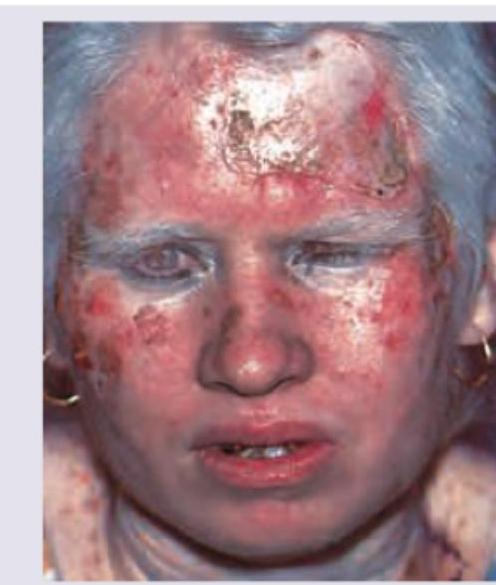
The image shows presence of:
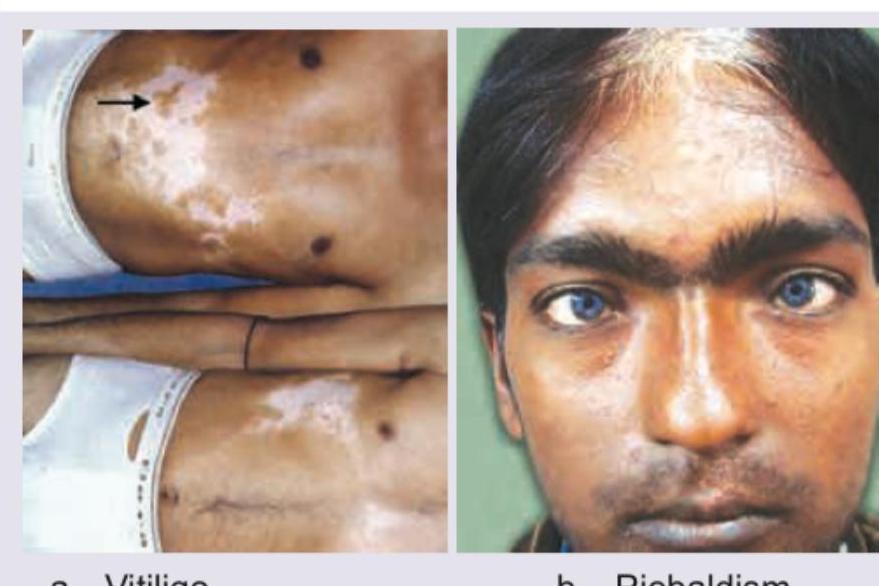
The image shows presence of:
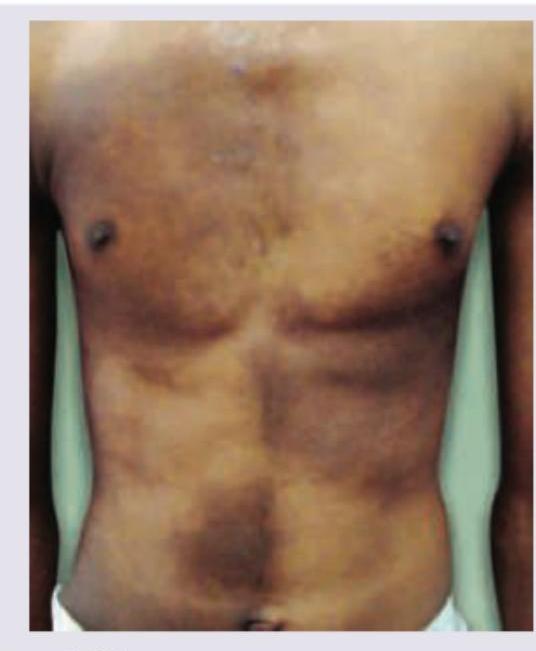
The image shows presence of:
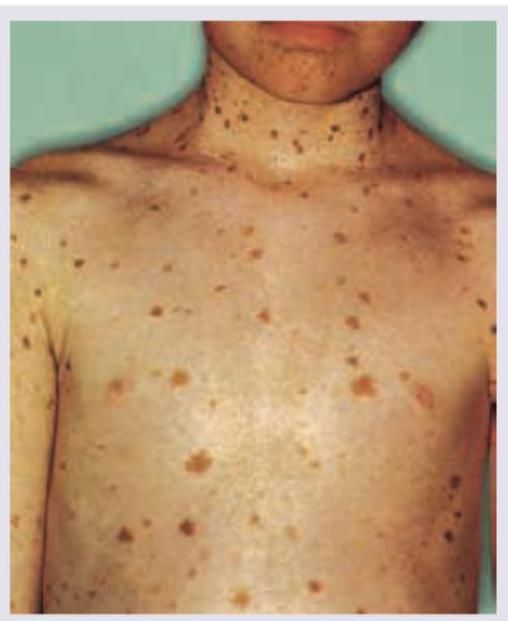
The image shows presence of:
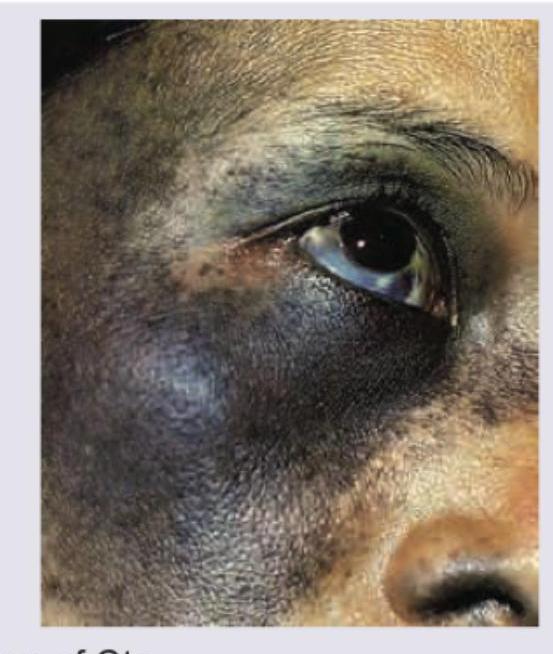
The lesion shown below is seen in:
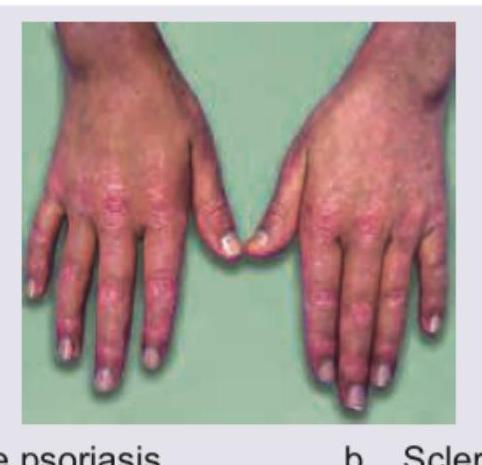
A patient with pancreatic tumor and impaired glucose tolerance is having these lesions on flexural areas. What is the diagnosis?
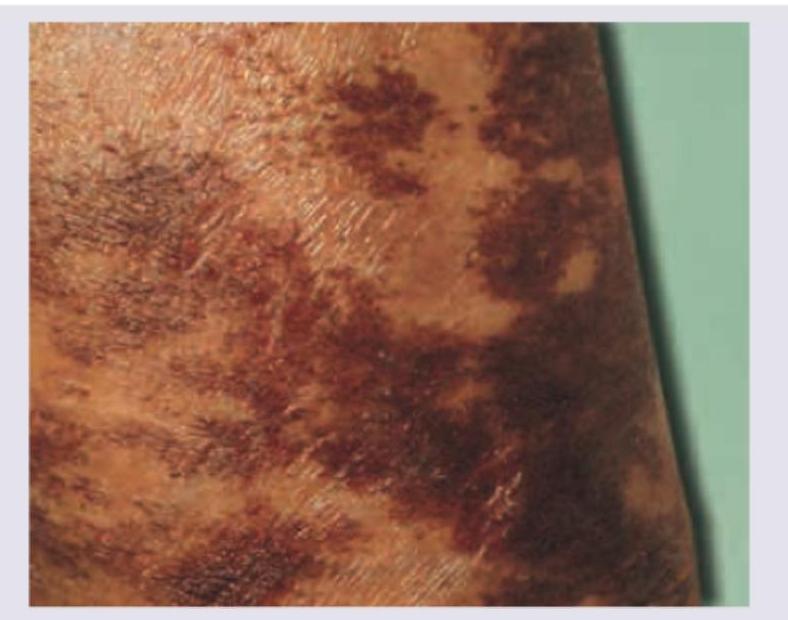
Practice by Chapter
Melanocyte Biology
Practice Questions
Vitiligo
Practice Questions
Melasma
Practice Questions
Post-inflammatory Hyperpigmentation
Practice Questions
Post-inflammatory Hypopigmentation
Practice Questions
Albinism
Practice Questions
Drug-Induced Pigmentary Changes
Practice Questions
Pityriasis Alba
Practice Questions
Pigmentary Demarcation Lines
Practice Questions
Nevi of Ota and Ito
Practice Questions
Management of Hyperpigmentation
Practice Questions
Management of Hypopigmentation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
