Pigmentary Disorders — MCQs

On this page
Which of the following is characteristic of Peibaldism?
Which of the following conditions does NOT cause diffuse hyperpigmentation?
Which of the following is the reason for the development of a simple lentigo?
Hypopigmented patches can be seen in which of the following conditions?
Sturge-Weber syndrome is associated with which of the following?
A female developed a brown macule on the cheek, forehead, and nose after exposure to light following delivery of a baby. What is the diagnosis?
Decreased number of melanocytes are seen in:
A 20-year-old patient presents with a non-progressive hypopigmented lesion on the trunk. On Wood's lamp examination, there is white accentuation. Diascopy is negative. What is the most likely diagnosis?
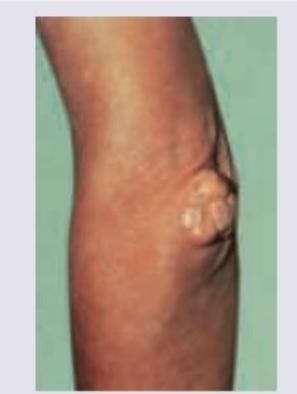
A 45-year-old patient with a history of elevated cholesterol levels presents with nodular swellings over the tendons. The lesion shown in the image is most likely:
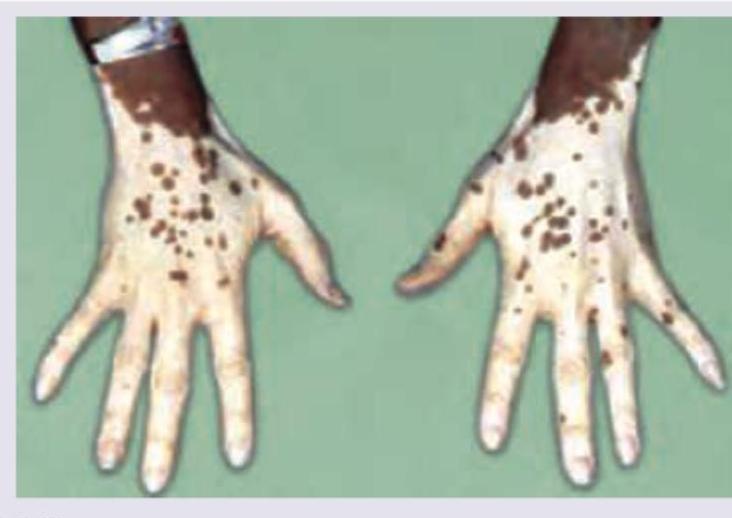
A patient presents with violaceous papules over the knuckles and mottled pigmentation on the dorsum of hands. Identify the lesion:
Practice by Chapter
Melanocyte Biology
Practice Questions
Vitiligo
Practice Questions
Melasma
Practice Questions
Post-inflammatory Hyperpigmentation
Practice Questions
Post-inflammatory Hypopigmentation
Practice Questions
Albinism
Practice Questions
Drug-Induced Pigmentary Changes
Practice Questions
Pityriasis Alba
Practice Questions
Pigmentary Demarcation Lines
Practice Questions
Nevi of Ota and Ito
Practice Questions
Management of Hyperpigmentation
Practice Questions
Management of Hypopigmentation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
