Pigmentary Disorders — MCQs

On this page
A female presents with hypopigmented lesions on the central forehead. Which drug is responsible?
Vitiligo is commonly associated with which of the following conditions?
A large, dark brown patch is noted on the back. What is the most likely diagnosis?
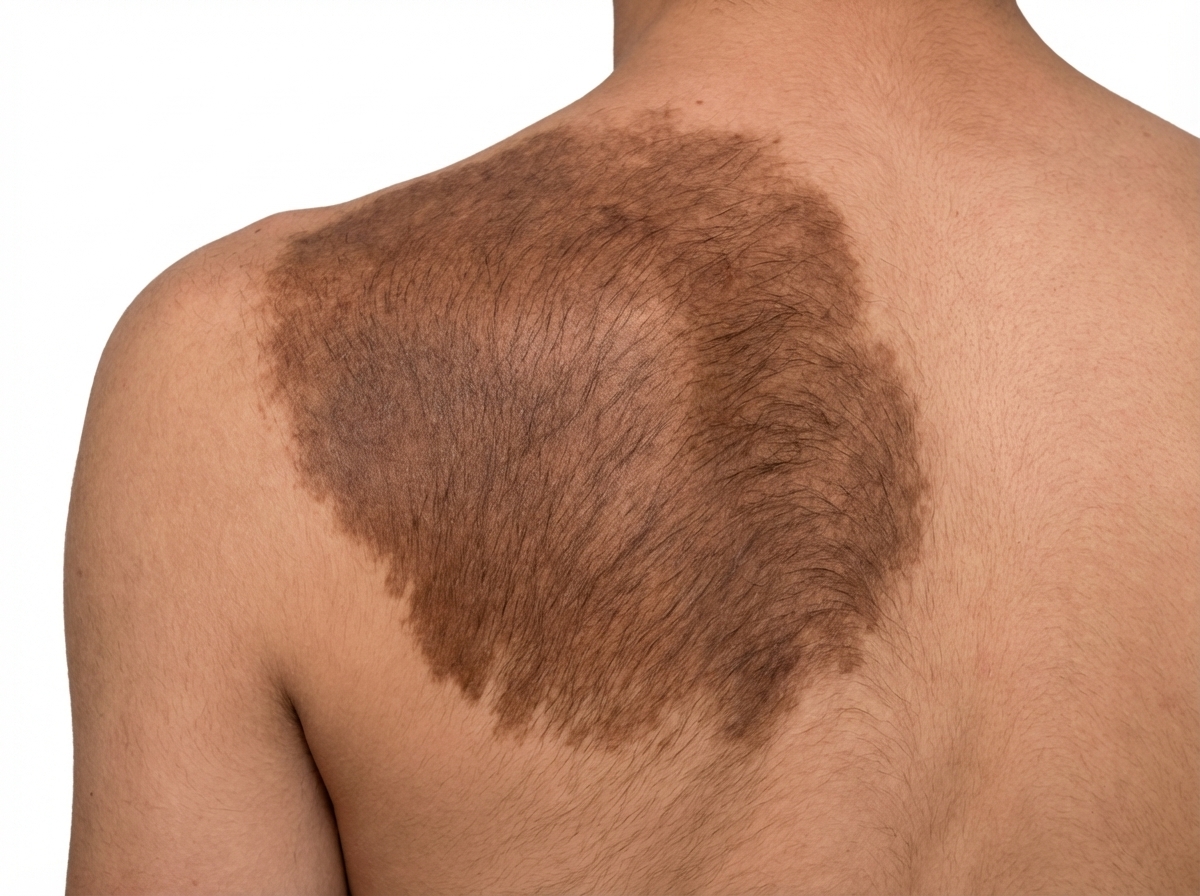
Which of the following conditions are associated with acanthosis nigricans?
Which is the characteristic lesion of pregnancy?
In an elderly patient, acanthosis nigricans usually indicates what?
What is the best treatment for vitiligo of the vulva?
A 28-year-old pregnant female presents with complaints of brownish pigmentation on the bridge of her nose and cheeks, noticed after returning from a beach vacation. There is no pain or itching at the affected site. What is your most likely diagnosis?
Cafe au lait macules are seen in which of the following conditions?
Which of the following conditions presents with hypopigmentation?
Practice by Chapter
Melanocyte Biology
Practice Questions
Vitiligo
Practice Questions
Melasma
Practice Questions
Post-inflammatory Hyperpigmentation
Practice Questions
Post-inflammatory Hypopigmentation
Practice Questions
Albinism
Practice Questions
Drug-Induced Pigmentary Changes
Practice Questions
Pityriasis Alba
Practice Questions
Pigmentary Demarcation Lines
Practice Questions
Nevi of Ota and Ito
Practice Questions
Management of Hyperpigmentation
Practice Questions
Management of Hypopigmentation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
