Pigmentary Disorders — MCQs

On this page
A 24-year-old male presents with a lesion at the site shown in the image for 4 years. He says it has increased in thickness over the years. Diagnosis is:
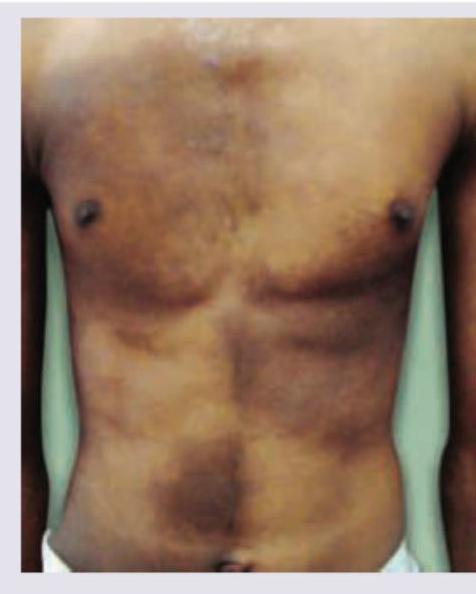
Which is not correct about the lesion shown below?
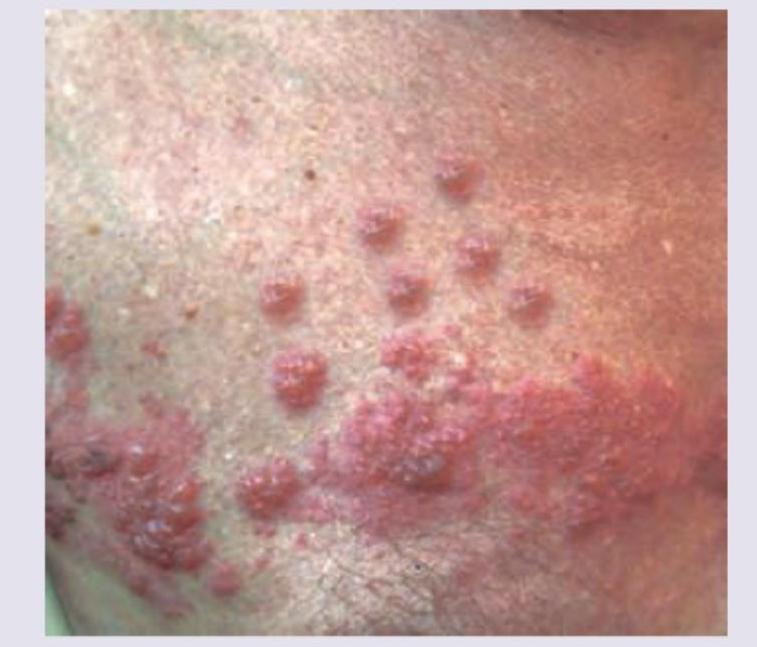
What is the best management of the case shown?
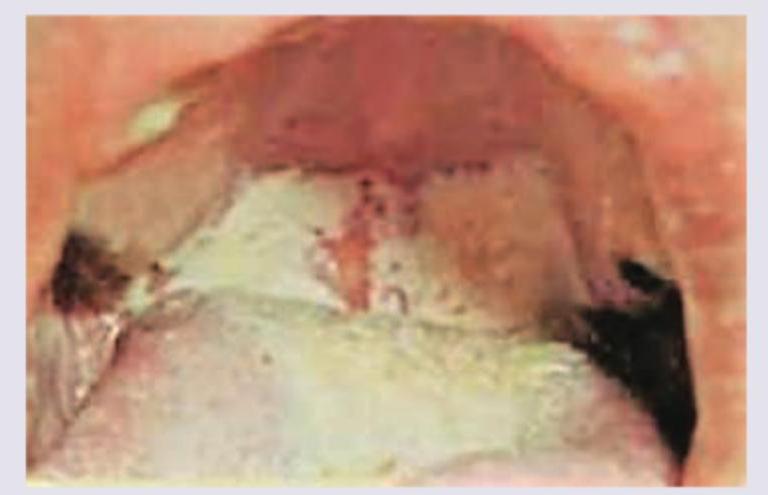
The image shows Bilateral Xanthelasma palpebrarum. Which of the following is the most common type of xanthoma?
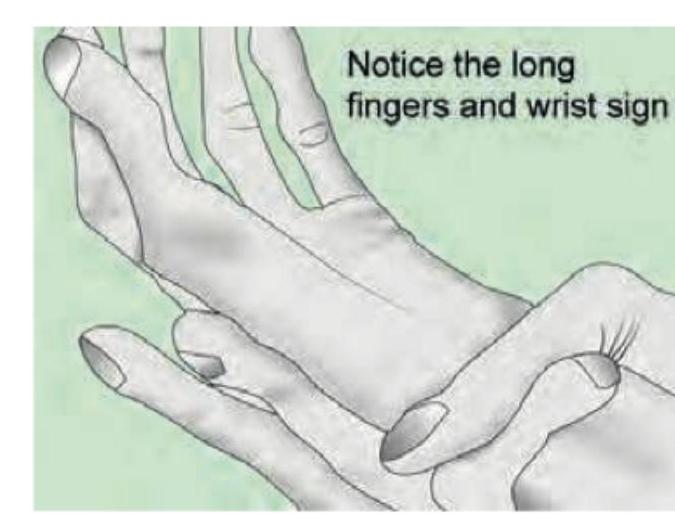
A 30-year-old male presents with joint pain and NSAIDs were prescribed. After one week, joint pain is persisting and he has developed brownish discoloration over nose as shown in the figure. This was due to: (AIIMS Nov 2017)
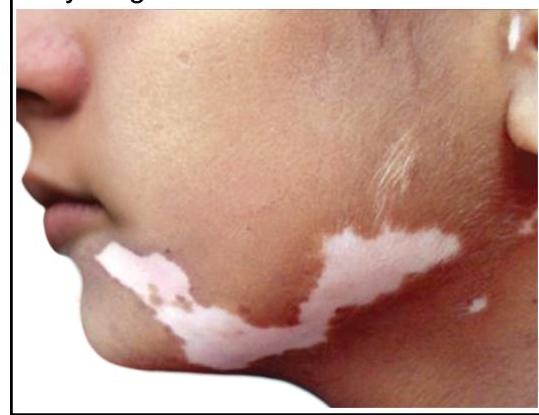
A young girl presents with leukotrichia and lesions as shown in the image. What is the most likely diagnosis?
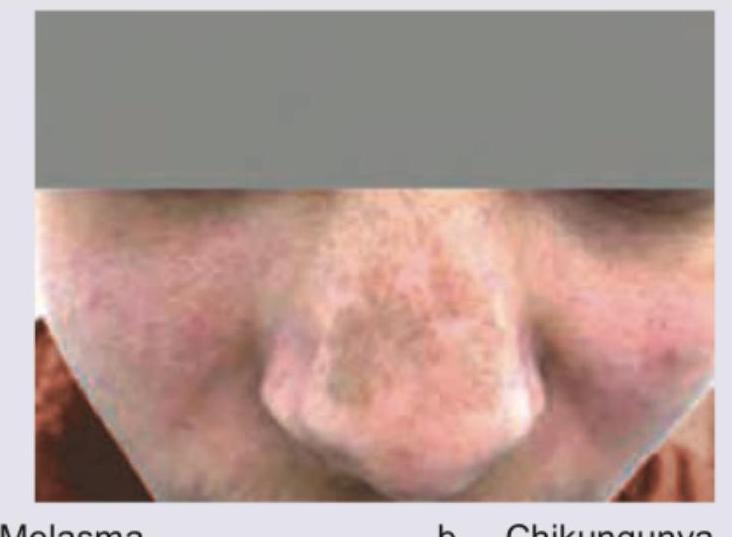
A 28-year-old woman presents with progressive darkening of her face that started during pregnancy. The pigmentation is symmetrical and primarily affects her cheeks and forehead. It became more prominent with sun exposure. Examination reveals bilateral, symmetrical brown patches on her face. Which of the following is the most appropriate initial management?
Which of the following chemical is responsible for the skin condition given below:

Which of the following is not true about hydroquinone?
False about melasma is?
Practice by Chapter
Melanocyte Biology
Practice Questions
Vitiligo
Practice Questions
Melasma
Practice Questions
Post-inflammatory Hyperpigmentation
Practice Questions
Post-inflammatory Hypopigmentation
Practice Questions
Albinism
Practice Questions
Drug-Induced Pigmentary Changes
Practice Questions
Pityriasis Alba
Practice Questions
Pigmentary Demarcation Lines
Practice Questions
Nevi of Ota and Ito
Practice Questions
Management of Hyperpigmentation
Practice Questions
Management of Hypopigmentation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
