Melasma — MCQs

Elderly man with a long-standing mole on his face that is increasing in size and showing an irregular border. Diagnosis:
All are predisposing factors of Deep Vein thrombosis, EXCEPT :
PUVA therapy is used in all except:
Which of the following is not true about hydroquinone?
Which of the following is an example of a barrier method of contraception?
A 15cm hyperpigmented macule on an adolescent male undergoes changes such as coarseness, growth of hair & acne. Diagnosis is?
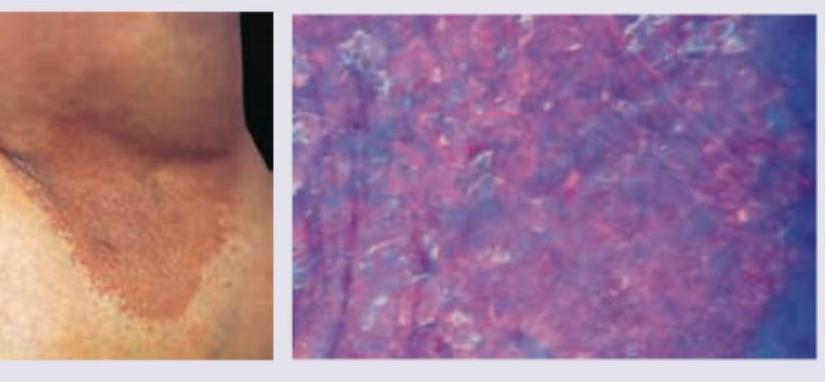
A 35-year-old obese woman presents with recurrent lesions in both axilla in summer season. Wood lamp examination is shown. The diagnosis is:
What is the most common association with Acanthosis nigricans?
An increased incidence of vitiligo is found in association with which of the following conditions?
A 'silver tattoo' is due to deposition of which substance in the oral mucosa?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
