Drug-Induced Pigmentary Changes — MCQs

All of the following drugs cause amorphous whorl like corneal deposits except:
Which drug is most likely to induce photosensitivity?
A 17 year old girl had been taking a drug for the treatment of acne for the last 2 years, which has led to pigmentation. Which drug could it be?
A patient with TB on DOTS develops orange-red discoloration of urine and tears. Which drug is responsible?
Krukenberg's spindle seen in patients with pigmentary glaucoma refers to deposition of pigment on
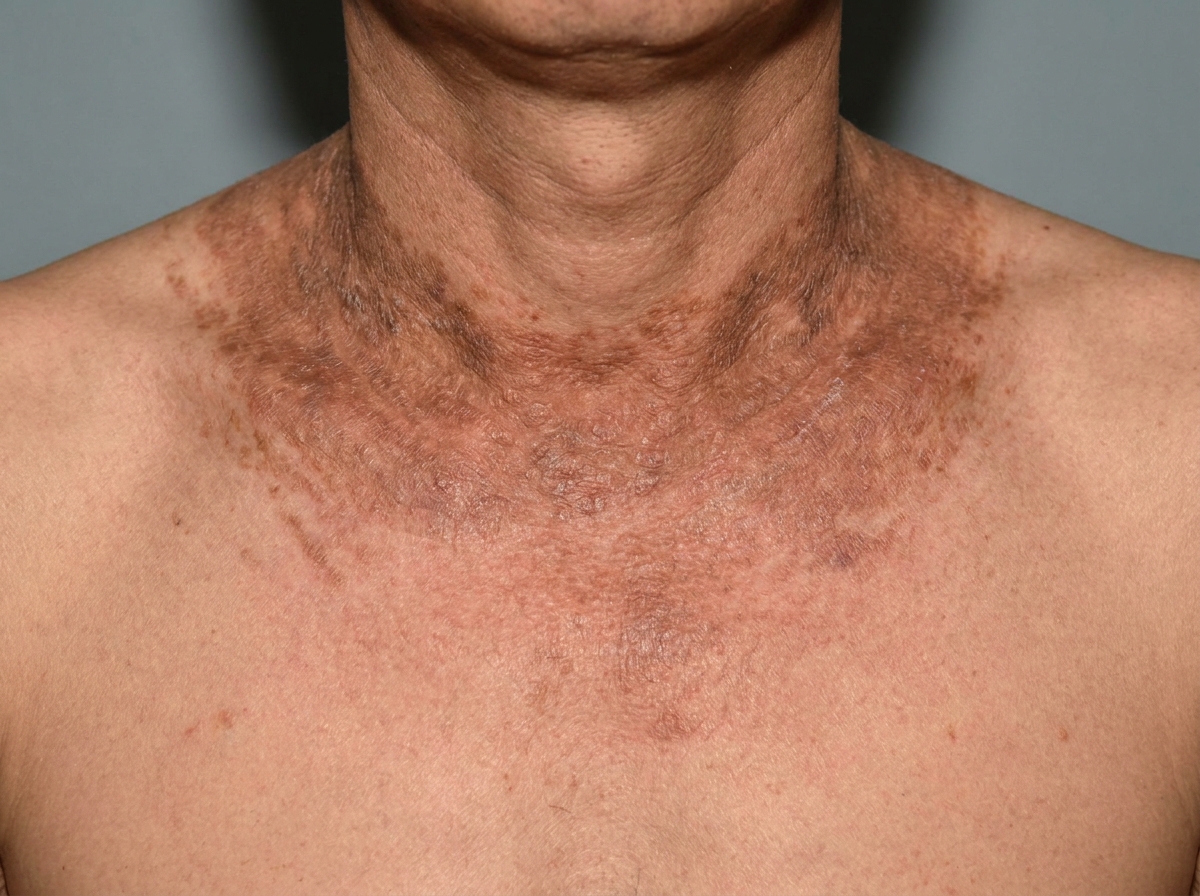
Dermatological manifestation of which of the following diseases?
Which of the following is not true about hydroquinone?
Cutis marmorata occurs due to exposure to –
A 50-year-old man with Fitzpatrick skin type V desires treatment for melasma. He was previously treated with triple combination cream with partial response. What would be the most evidence-based next step considering safety and efficacy?
What is the most common association with Acanthosis nigricans?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
