Diagnosis and Patch Testing — MCQs

A child has a rash. His family history is positive for asthma. What could be the most probable diagnosis?
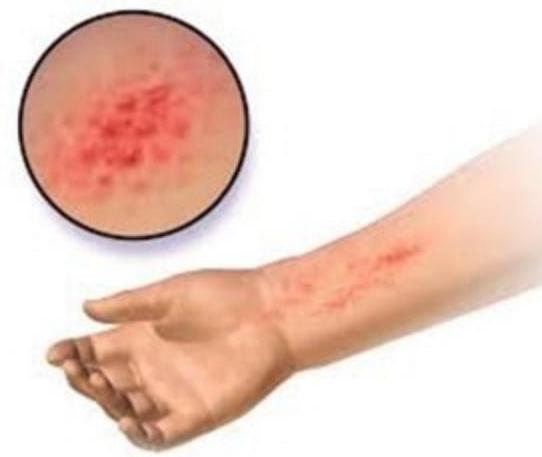
A patient comes to you with skin reactions after visiting the hair dresser. What will you do to confirm the diagnosis of contact dermatitis?
What is the diagnosis if a patient can only see 3 green dots on the Worth 4 Dot test?
Cover test and prism testing are used to diagnose which ocular condition?
Which test is essential in a patient with suspected Cushing's syndrome for diagnosis confirmation?
Most sensitive test for carpal tunnel syndrome -
A 52 year old lady presents with constant leakage of urine and dysuria two weeks after a complicated total abdominal hysterectomy. A diagnosis of Vesicovaginal fistula is suspected. The most important test for the diagnosis is:
Most sensitive test for myaesthenia gravis
A patient presents with fever and retro-orbital pain. Which investigation should be conducted next for confirmation of dengue fever?
Best provocative test for diagnosis of Gastrinoma is:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
