Hair and Nail Disorders — MCQs

On this page
Nail involvement is seen in which of the following conditions?
A 35-year-old male presents with bald patches and no scars. The patches are well demarcated with broken hair at the edges. What is the diagnosis?
Which of the following drugs does NOT cause hirsutism?
Androgenic alopecia in females is caused by which of the following conditions?
Cicatricial alopecia is seen in which of the following conditions?
An elderly female undergoing chemotherapy for breast cancer is experiencing significant hair loss. What is the most likely cause of her condition?
Which of the following statements regarding the condition shown is false?
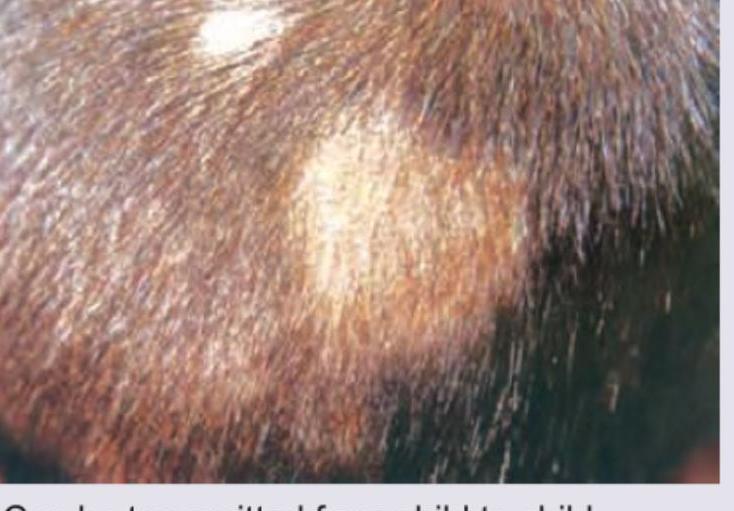
The image shows presence of:
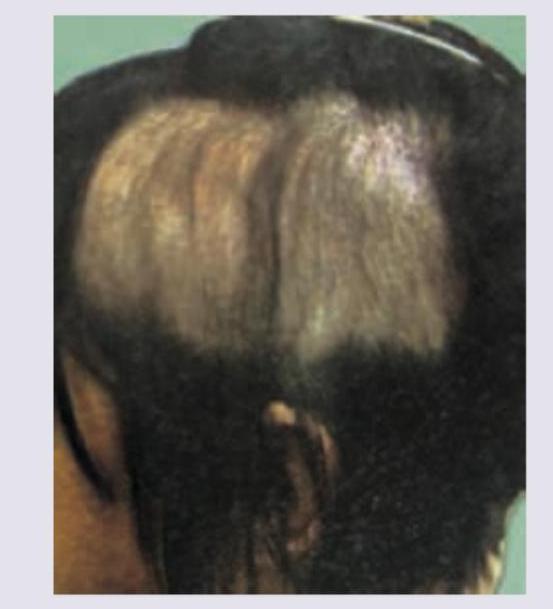
The following patient presented to the OPD with history of hair loss. There was no erythema, scarring or scratching. Diagnosis is:
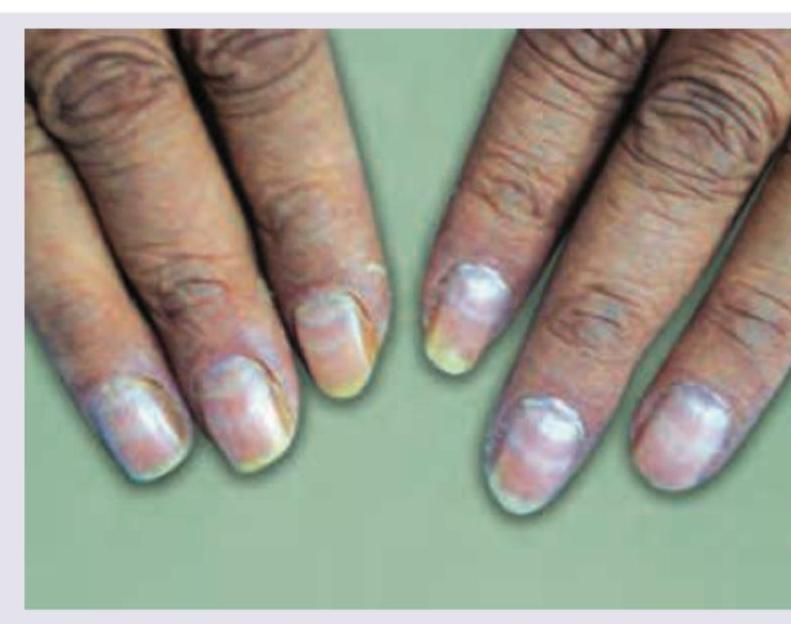
The nail lesion shown in the image is known as?
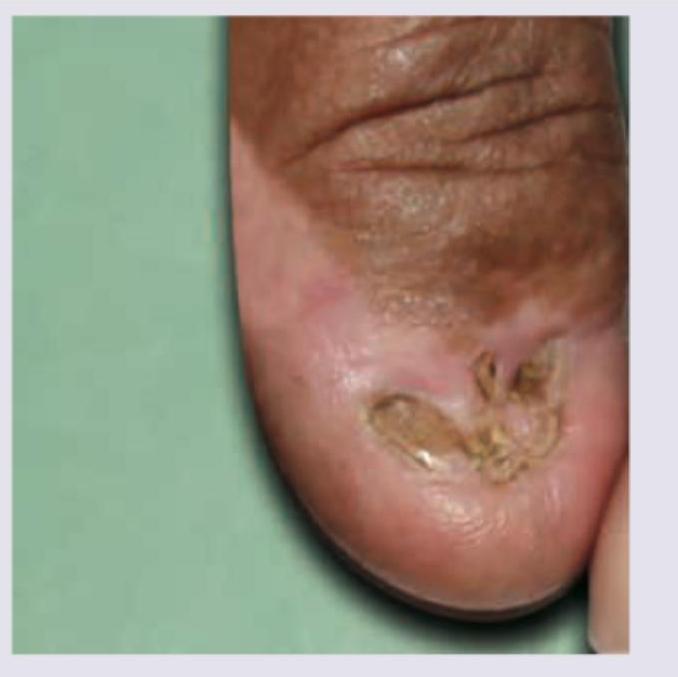
Practice by Chapter
Hair Growth Cycle and Anatomy
Practice Questions
Alopecia Areata
Practice Questions
Androgenetic Alopecia
Practice Questions
Telogen Effluvium
Practice Questions
Scarring Alopecias
Practice Questions
Hair Shaft Abnormalities
Practice Questions
Hirsutism and Hypertrichosis
Practice Questions
Nail Anatomy and Growth
Practice Questions
Nail Infections
Practice Questions
Nail Psoriasis and Other Inflammatory Nail Disorders
Practice Questions
Nail Tumors
Practice Questions
Management of Hair and Nail Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
