Hair and Nail Disorders — MCQs

On this page
What is the condition characterized by the sudden onset of hair turning white overnight?
A 30-year-old female presents with a painful, red, warm nail fold of 7 days duration. The patient has tried home remedies such as turmeric powder and warm saline compressions without relief. What is the most probable diagnosis?
Cicatricial alopecia is seen in all of the following conditions EXCEPT?
Which of the following statements is NOT true regarding the hair cycle?
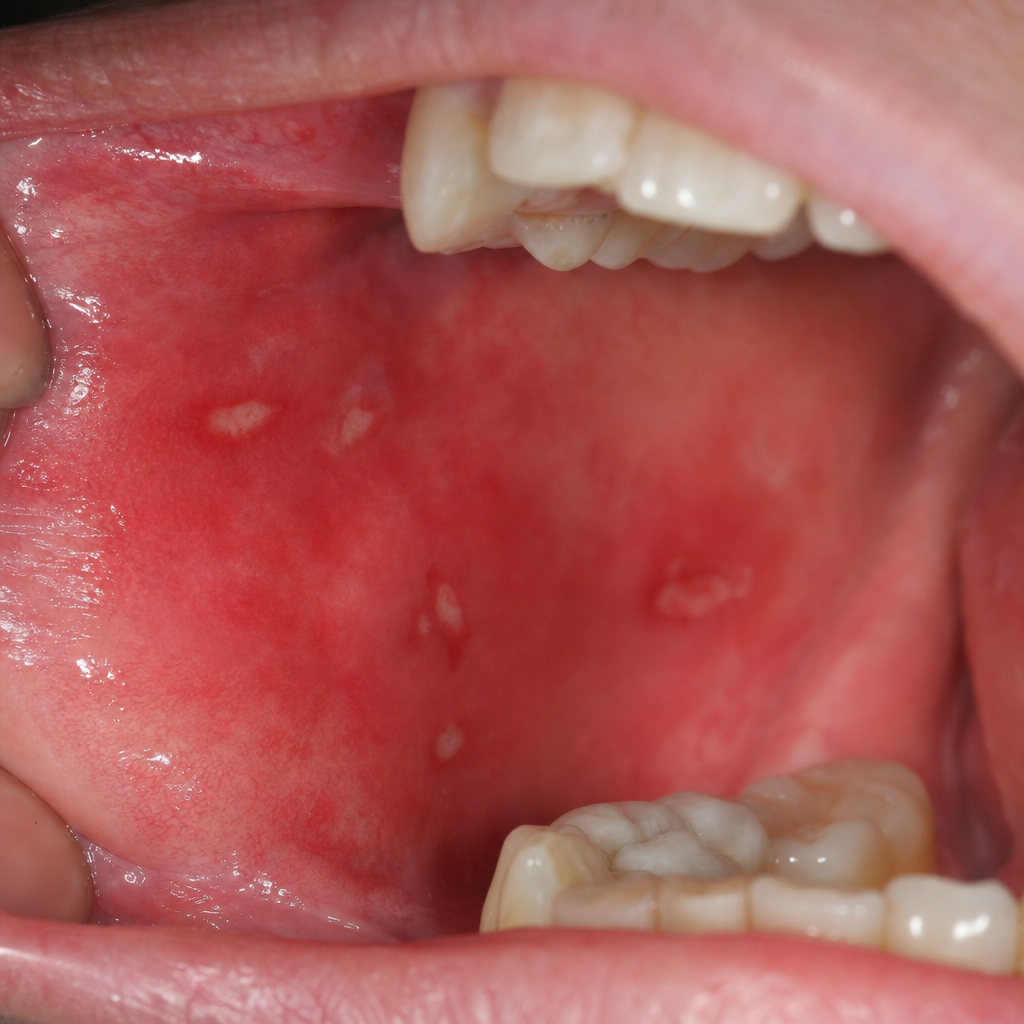
What is the most likely cause of this presentation?
The time period that elapses between physical or emotional stress and hair loss is approximately:
Coarse pitting of nails is seen in?
Cicatrising alopecia with perifollicular blue-gray patches of hyperpigmentation is most commonly associated with which of the following clinical findings?
Pterygium of the nail is seen in which of the following conditions?
Nail pitting is associated with all of the following conditions except?
Practice by Chapter
Hair Growth Cycle and Anatomy
Practice Questions
Alopecia Areata
Practice Questions
Androgenetic Alopecia
Practice Questions
Telogen Effluvium
Practice Questions
Scarring Alopecias
Practice Questions
Hair Shaft Abnormalities
Practice Questions
Hirsutism and Hypertrichosis
Practice Questions
Nail Anatomy and Growth
Practice Questions
Nail Infections
Practice Questions
Nail Psoriasis and Other Inflammatory Nail Disorders
Practice Questions
Nail Tumors
Practice Questions
Management of Hair and Nail Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
