Laser Therapy Basics — MCQs

What is the best range of UV light used for treatment of skin diseases?
Which of the following burn cases requires IMMEDIATE referral to a specialized burn center?
Which of the following events does NOT occur in rods in response to light
The most specific test to detect blood stains is:
Which of the following are correct for managing hypertrophic scars? 1. Silicone gel sheeting 2. Intralesional steroid injections 3. Vitamin A gel applications 4. Laser treatment Select the answer using the code given below.
What is the first-line treatment for melasma?
What is the best method to treat a large port-wine stain?
Which of the following statements about conjunctival lesions is NOT true?
A 40 year old man presented with a flat 1x1cm scaly, itchy black mole on the front of thigh. Examination did not reveal any inguinal lymphodenopathy. The best course of management would be:
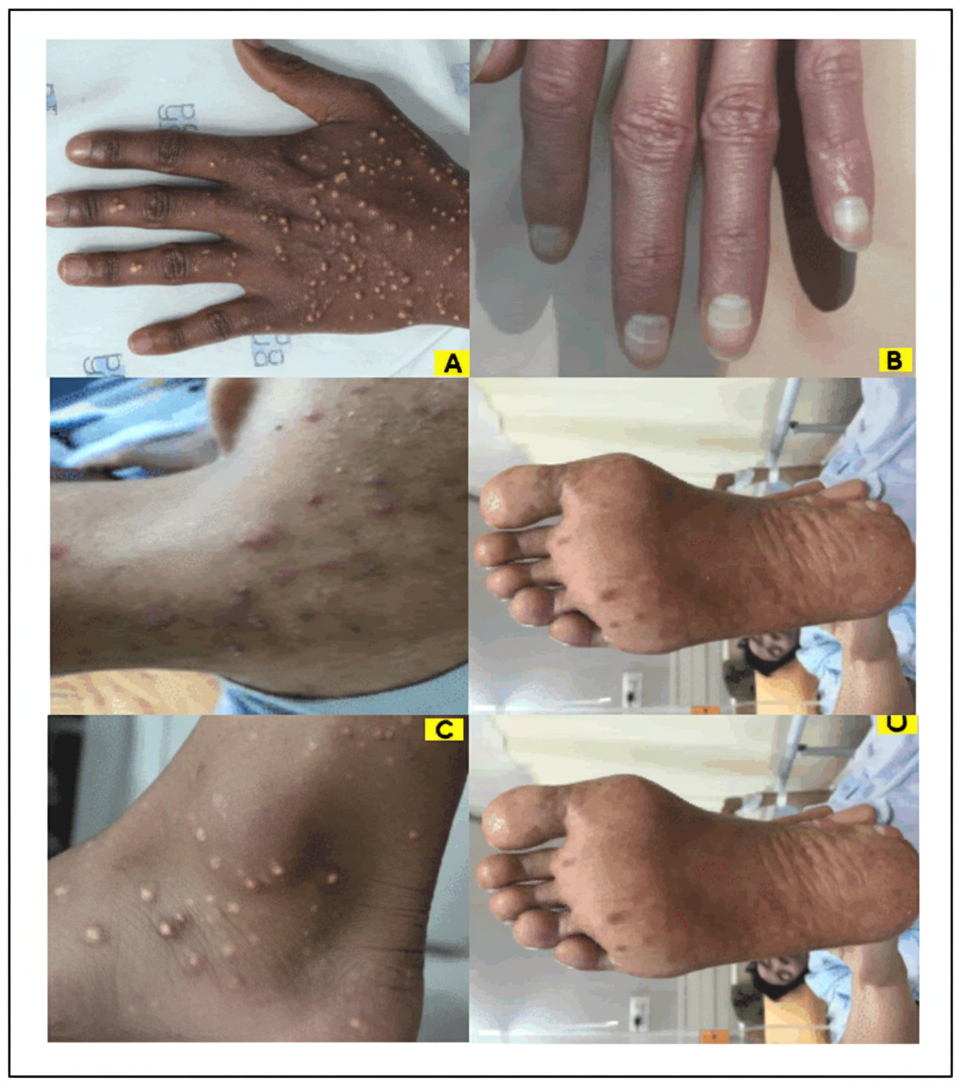
Comment on the image shown:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
