Dermatological Pharmacology — MCQs

On this page
For how long before pregnancy should isotretinoin be stopped?
Corticosteroids are contraindicated in all of the following conditions except:
A patient presents to the dermatology clinic reporting recurrent skin lesions as seen on the image. He describes that these lesions emerge within hours each time he takes NSAIDs. What is the most likely diagnosis?
Which of the following are recognized side effects of topical corticosteroid use? a. Hypertrichosis b. Acneiform eruptions c. Skin atrophy d. Blue pigmentation of the skin
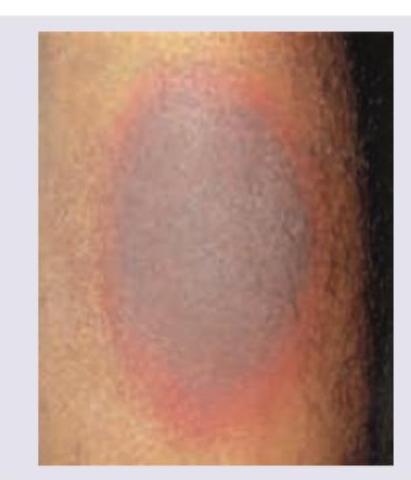
A 30-year-old woman with multiple episodes of GTCS was prescribed phenytoin by district hospital physician. After 7 days she presents with a single skin lesion on her arm as shown below. Which of the following will predispose to the condition shown here? (Recent NEET Pattern 2016-17)
A 40-year-old man with severe hidradenitis suppurativa on adalimumab develops new pustules and nodules despite compliance. Current weight is 120 kg. Most appropriate next step is:
Which of the following statements about biologics in psoriasis is FALSE?
Match the systemic medications with their most characteristic cutaneous adverse effects: 1. Hydroxyurea a. Acral erythema 2. Capecitabine b. Leg ulcers 3. EGFR inhibitors c. Acneiform eruption
A 50-year-old woman presents with a well-defined erythematous patch on her leg following the administration of an antibiotic. What is the most likely diagnosis?
Which is the first generation topical retinoid?
Practice by Chapter
Topical Corticosteroids
Practice Questions
Topical Antibiotics
Practice Questions
Topical Antifungals
Practice Questions
Topical Antivirals
Practice Questions
Topical Retinoids
Practice Questions
Systemic Retinoids
Practice Questions
Immunosuppressive Agents
Practice Questions
Antihistamines in Dermatology
Practice Questions
Biological Agents in Dermatology
Practice Questions
Dermatological Vehicles and Delivery Systems
Practice Questions
Phototherapeutic Agents
Practice Questions
Adverse Cutaneous Drug Reactions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
