Dermatological Pharmacology — MCQs

On this page
Which of the following treatments would you recommend for this patient?
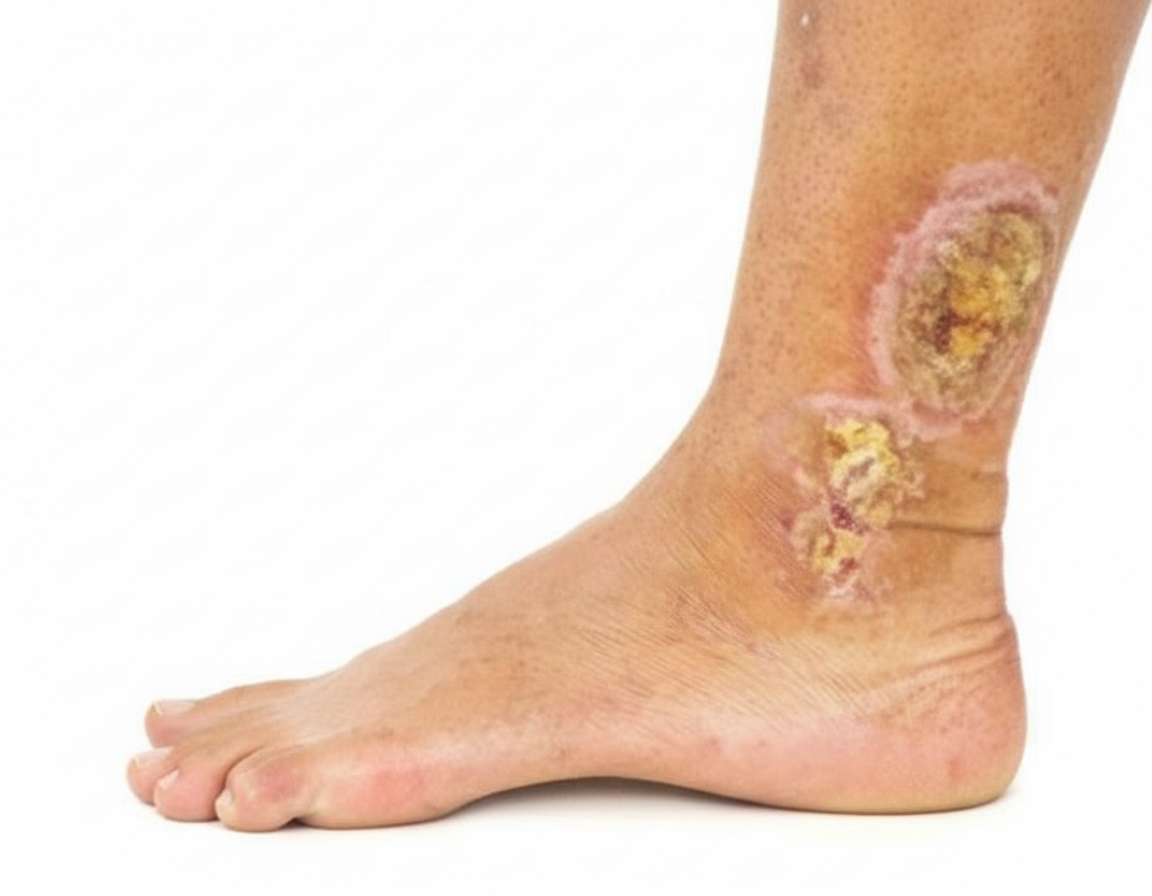
Steroids are contraindicated in all of the following conditions, EXCEPT:
Which drug is known to cause non-pigmenting fixed drug reactions?
What is the treatment of choice for Sweet's syndrome?
What is the most common drug-induced skin reaction?
Which drug is known to cause acanthosis nigricans?
Chloroquine is used in the treatment of which of the following dermatological conditions?
Which of the following conditions is treated with systemic corticosteroids?
Which of the following steroids is not used topically?
What is the most effective treatment for pruritus in uremia?
Practice by Chapter
Topical Corticosteroids
Practice Questions
Topical Antibiotics
Practice Questions
Topical Antifungals
Practice Questions
Topical Antivirals
Practice Questions
Topical Retinoids
Practice Questions
Systemic Retinoids
Practice Questions
Immunosuppressive Agents
Practice Questions
Antihistamines in Dermatology
Practice Questions
Biological Agents in Dermatology
Practice Questions
Dermatological Vehicles and Delivery Systems
Practice Questions
Phototherapeutic Agents
Practice Questions
Adverse Cutaneous Drug Reactions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
