Dermatological Pharmacology — MCQs

On this page
Which of the following anti-tuberculosis drugs can cause Stevens-Johnson syndrome?
Warfarin skin necrosis is caused by which of the following?
Which of the following is NOT a complication of TEN?
What is the most likely diagnosis in a woman who developed eosinophilia and a diffuse erythematous eruption while being treated with hydroxychloroquine for Sjogren's syndrome?
Recurrent lesions on the glans that heal with residual hyperpigmentation are suggestive of:
Pseudoporphyria can be induced by all except?
A 76-year-old lady with a history of a red facial rash and venous eczema of the legs, who was treated for acne rosacea by her GP, presented with bluish pigmentation on both legs on examination. What drug is likely to have caused this?
Annular herald patch is seen in:
What is the management for the given case?
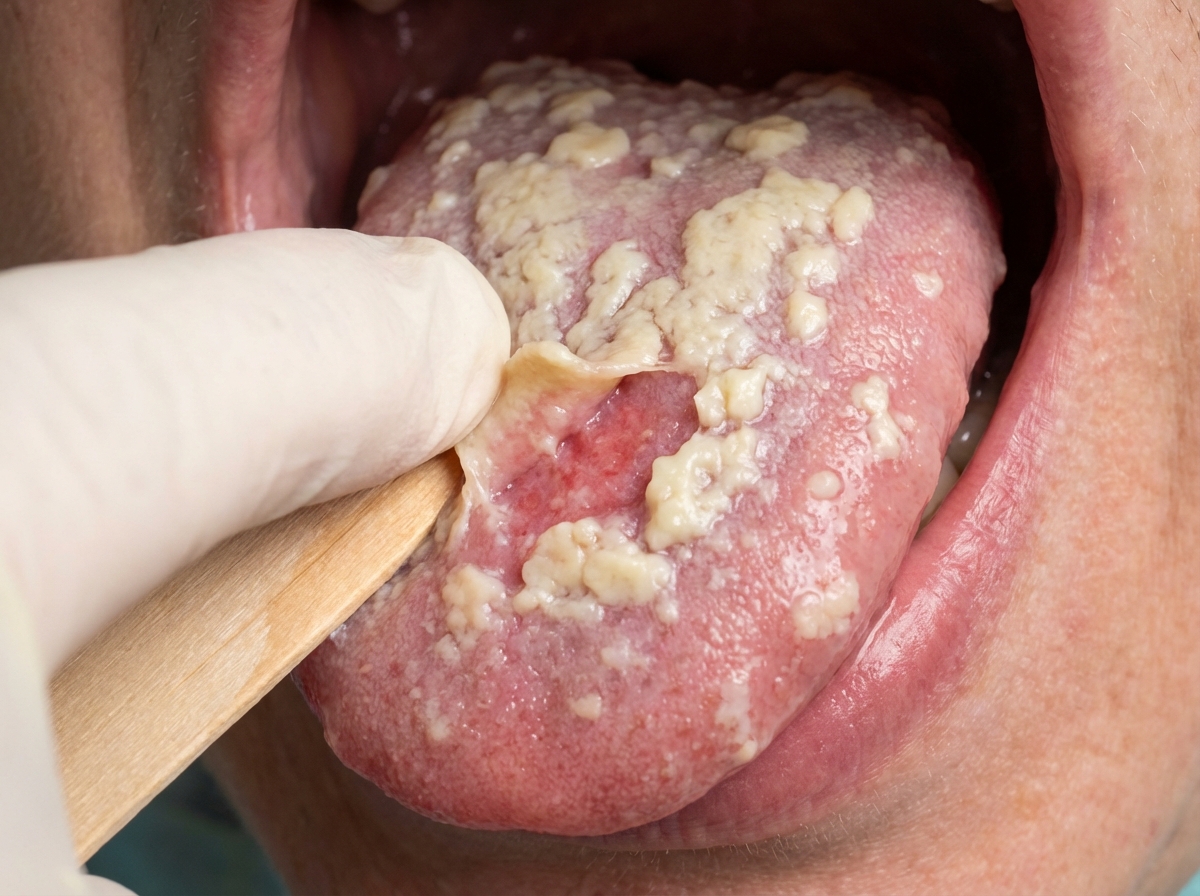
What is the drug of choice for dermatitis herpetiformis?
Practice by Chapter
Topical Corticosteroids
Practice Questions
Topical Antibiotics
Practice Questions
Topical Antifungals
Practice Questions
Topical Antivirals
Practice Questions
Topical Retinoids
Practice Questions
Systemic Retinoids
Practice Questions
Immunosuppressive Agents
Practice Questions
Antihistamines in Dermatology
Practice Questions
Biological Agents in Dermatology
Practice Questions
Dermatological Vehicles and Delivery Systems
Practice Questions
Phototherapeutic Agents
Practice Questions
Adverse Cutaneous Drug Reactions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
