Basic Dermatology — MCQs

On this page
Which of the following are characteristic features of lichen planus?
A 38-year-old woman presented with a 2-week history of tender, swollen nodules on her lower legs. Her only current medication was a triphasic oral contraceptive. She denies any history of inflammatory bowel disease, sarcoidosis, or chronic infections. Physical examination revealed erythematous nodular swellings on the anterior lower legs. A punch biopsy specimen obtained from a lesion on the left anterior tibia reveals a septal inflammation of subcutaneous fat. What is the best description of this rash?
Thin zone of Grenz is seen in which of the following conditions?
A young lady presents with white lacy lesions in the oral cavity and her proximal nail fold has extended onto the nail bed. What is the likely diagnosis?
A patient presents with diffuse, nonencapsulated fatty deposits. Which of the following is the most likely associated history?
All are true about the features of erythromelalgia, EXCEPT:
A 40-year-old woman presents with a burning sensation in the mouth. Clinical examination reveals lesions consisting of radiating white striations in a retiform arrangement affecting the buccal mucosa, tongue, lips, and gingiva bilaterally. An incisional biopsy is suggestive of lichen planus. Which of the following is NOT a clinical form of Lichen Planus?
What is true about this condition?
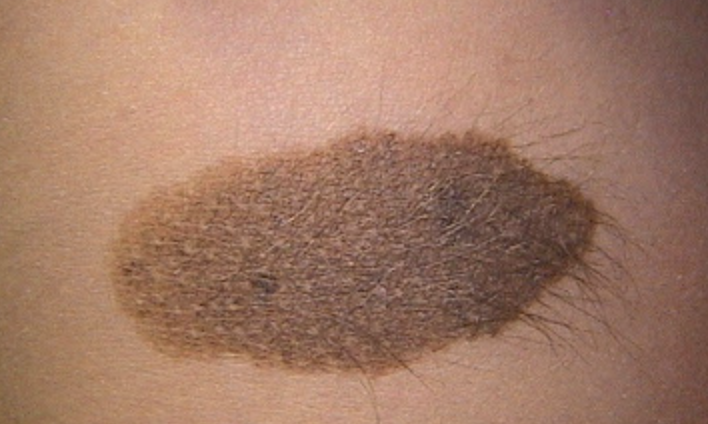
All of the following are primary cutaneous diseases except?
What is the characteristic histological feature of lichen planus?
Practice by Chapter
Structure and Function of Skin
Practice Questions
Cutaneous Histopathology
Practice Questions
Dermatological Examination
Practice Questions
Skin Lesions: Morphology and Description
Practice Questions
Principles of Diagnosis in Dermatology
Practice Questions
Dermatological Procedures
Practice Questions
Wound Healing
Practice Questions
Cutaneous Immunology
Practice Questions
Genetics in Dermatology
Practice Questions
Cutaneous Manifestations of Systemic Diseases
Practice Questions
Geriatric Dermatology
Practice Questions
Pediatric Dermatology Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
