Basic Dermatology — MCQs

On this page
A 28-year-old male presented with a rash on his arms, legs, and face, along with painful ulceration of his lips and mouth, and fever. He developed acute sore throat and conjunctivitis, leading to a diagnosis of acute pharyngitis. Oral penicillin was prescribed. Which of the following can be used in the treatment of the patient's condition, EXCEPT?
All of the following perforating disorders are associated with chronic renal failure EXCEPT:
Keloid formation is not typically seen over which of the following areas?
All of the following are primary lesions of the skin except:
Necrotic keratinocytes are typically seen in which of the following conditions?
The pustular, neutrophil-rich skin lesions that develop or worsen following intradermal trauma is called what?
What is the approximate number of bacteria per square centimeter of skin?
Blaschko's lines refers to lines of what developmental process?
Oral examination of a 57-year-old female reveals a white patch on the buccal mucosa that cannot be scraped off. She has no features suggestive of immunosuppression. What is the most likely diagnosis?
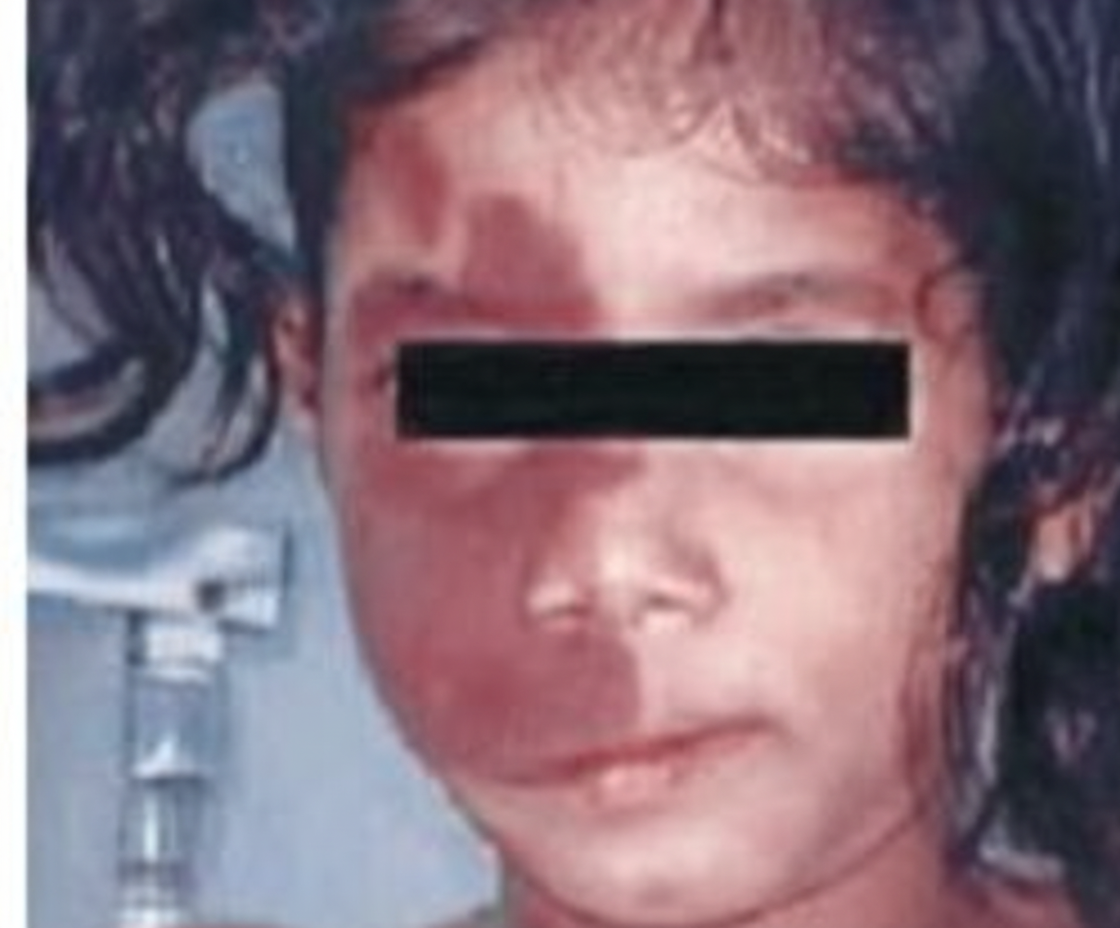
Which of the following conditions is characterized by the finding shown below?
Practice by Chapter
Structure and Function of Skin
Practice Questions
Cutaneous Histopathology
Practice Questions
Dermatological Examination
Practice Questions
Skin Lesions: Morphology and Description
Practice Questions
Principles of Diagnosis in Dermatology
Practice Questions
Dermatological Procedures
Practice Questions
Wound Healing
Practice Questions
Cutaneous Immunology
Practice Questions
Genetics in Dermatology
Practice Questions
Cutaneous Manifestations of Systemic Diseases
Practice Questions
Geriatric Dermatology
Practice Questions
Pediatric Dermatology Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
