Cutaneous Immunology — MCQs

What is the primary function of Langerhans' cells?
A 32 year old man presents with a 3-month history of weight loss, night sweats, a productive cough with blood-tinged sputum, anorexia, general malaise, and a low grade fever. A PPD skin test shows > 10 mm of induration. If the area of induration were biopsied, which of the following type of reactive cells would be found?
A 60-year-old female presents with eczematous itching lesions. Biopsy revealed a subepidermal cleft with Direct Immunofluorescence showing Linear C3 & IgG deposition along the basement membrane zone. What is the likely diagnosis?
Statement 1 - A 59-year-old patient presents with flaccid bullae. Histopathology shows a suprabasal acantholytic split. Statement 2 - The row of tombstones appearance is diagnostic of Pemphigus vulgaris.
Most common precipitant of contact dermatitis is?
In a patient with the following lesion on scalp, what changes are seen in the nails?
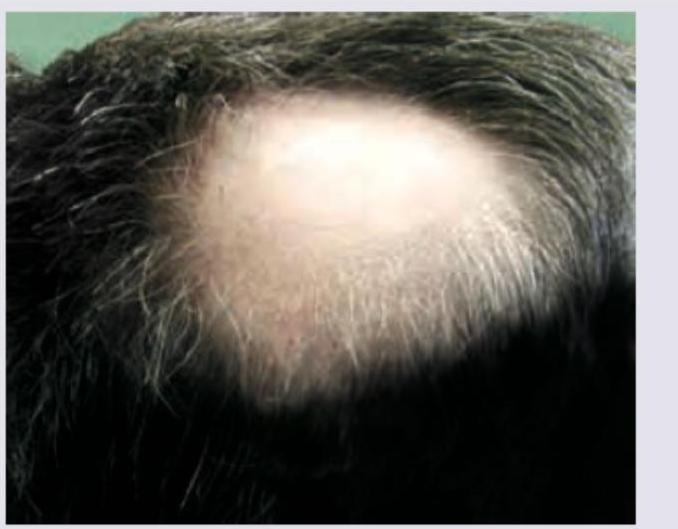
In which of the following conditions is the Koebner phenomenon most commonly observed?
Patient on anti-TB drugs develops tender nodules on shins. Most likely diagnosis is:
Lines of Blaschko are related to?
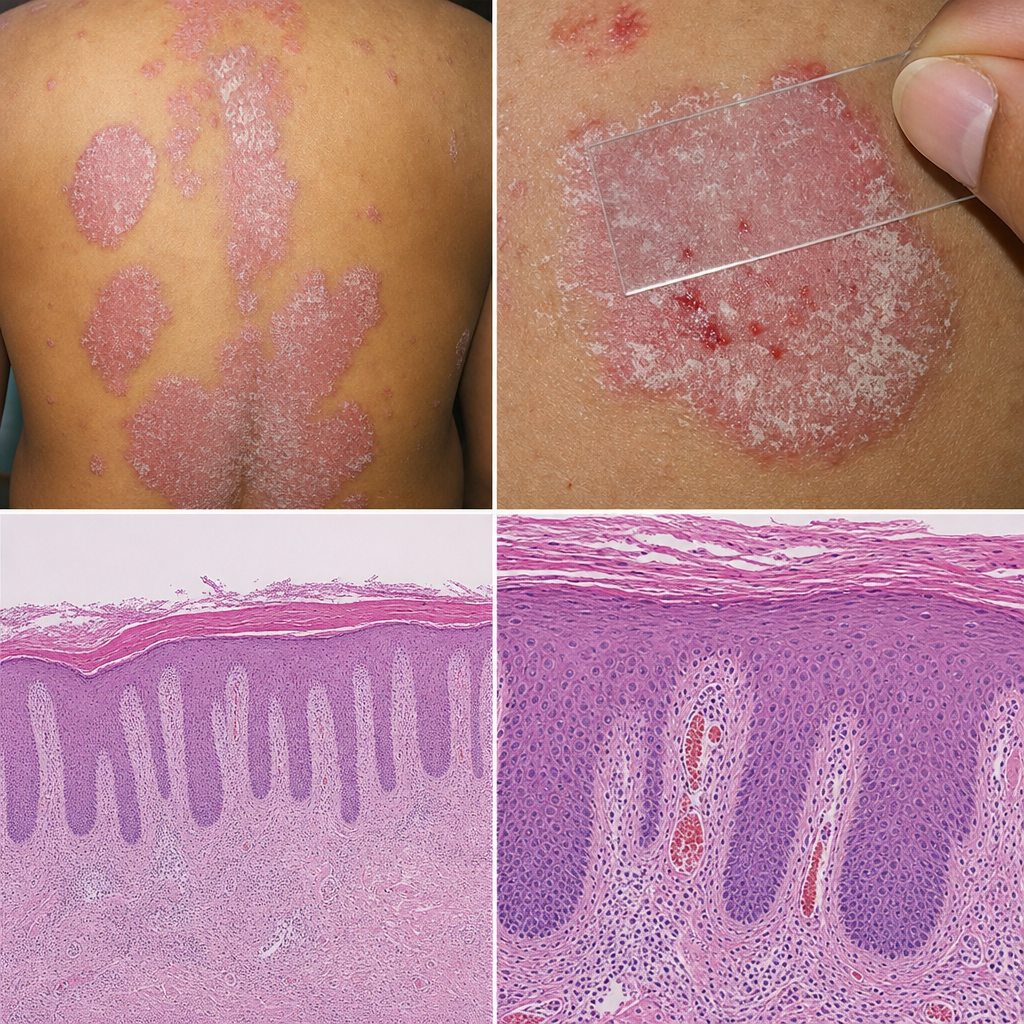
A 35-year-old man presents with a 2-year history of recurring itchy skin lesions that worsen in winter. His father had a similar condition. Examination reveals Auspitz sign on gentle scraping. The skin findings are shown in Image 1. Which of the following pathophysiological mechanisms is most directly responsible for the sign elicited on scraping in this patient?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
