Immunobullous Disorders — MCQs

Which of the following is NOT a characteristic of pemphigus vulgaris?
A skin biopsy shows acantholysis with intraepidermal blistering. Which immunofluorescence pattern would confirm pemphigus vulgaris?
A 40 year old male reported with recurrent episodes of oral ulcers, large areas of denuded skin and flaccid vesiculo-bullous eruptions. Which is the most important bedside investigation helpful in establishing the diagnosis -
Which of the following statements about mucous membrane pemphigoid is correct?
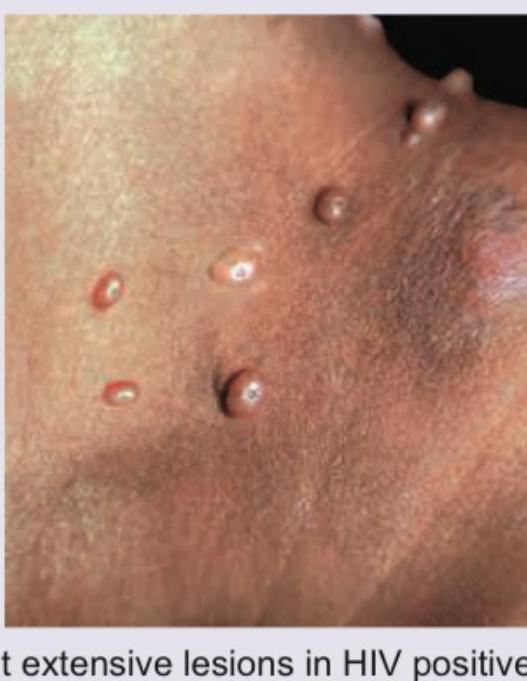
A patient presents with the skin lesions shown in the image. While evaluating for possible blistering disorders, all of the following conditions could present with similar morphology EXCEPT:
A child presents with grouped vesicles on an erythematous base on the buttocks. What is the most likely diagnosis?
A skin biopsy shows suprabasilar acantholysis with 'row of tombstones' appearance. Which immunofluorescence pattern would confirm pemphigus vulgaris?
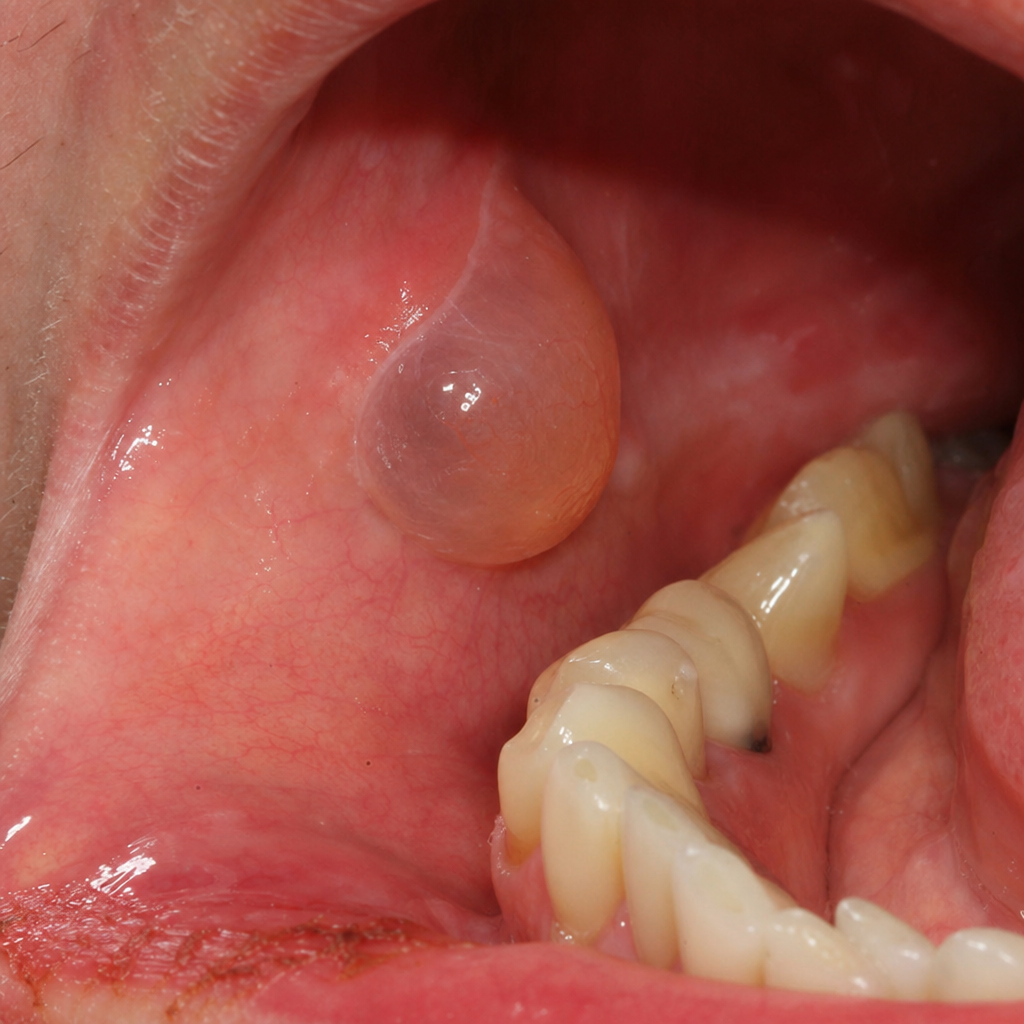
The following image shows a flaccid bulla. This finding is characteristically seen in:
Which of the following is NOT associated with erythema nodosum?
Acantholysis is seen in all except which of the following conditions?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
