Acne and Related Disorders — MCQs

On this page
What is the most appropriate treatment for severe acne?
An 18-year-old female patient comes with the following findings. Which of the following is pathognomonic of the primary stage of this disease?
Which of the following is the first-line topical treatment for mild to moderate acne vulgaris?
A 25-year-old girl presents with papules, erythema and telangiectasia over the face as shown below. She also gives a history of flushing and burning sensation on exposure to sun and on any emotional disturbance. The most likely diagnosis is? (AIIMS Nov 2016)
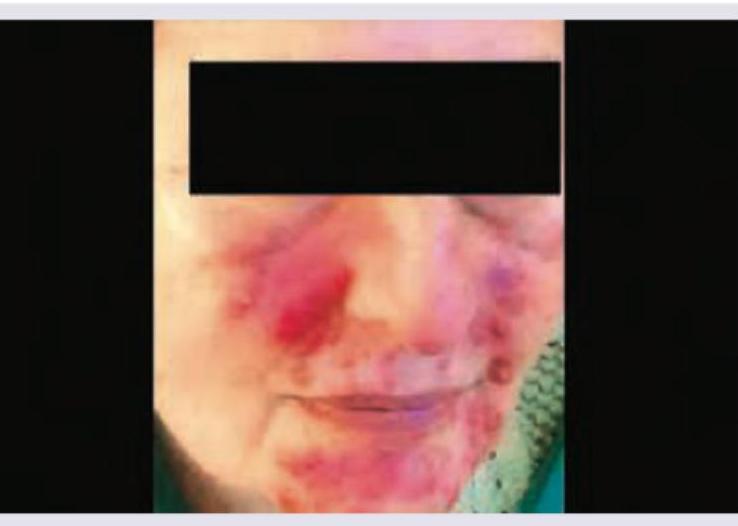
A young boy with oily skin presents with acne as shown. What is the appropriate treatment?

What does the given image show?
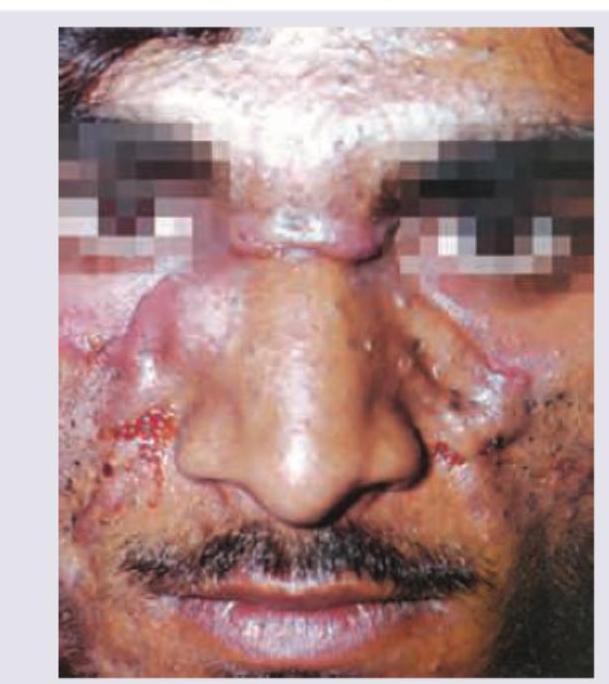
All are true about the condition shown in the figure except: (Recent NEET Pattern 2016-17)
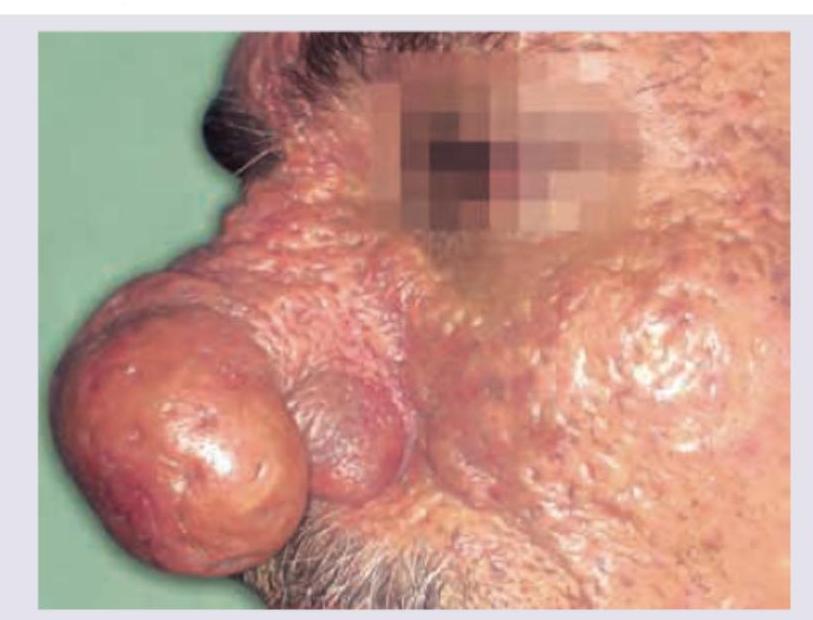
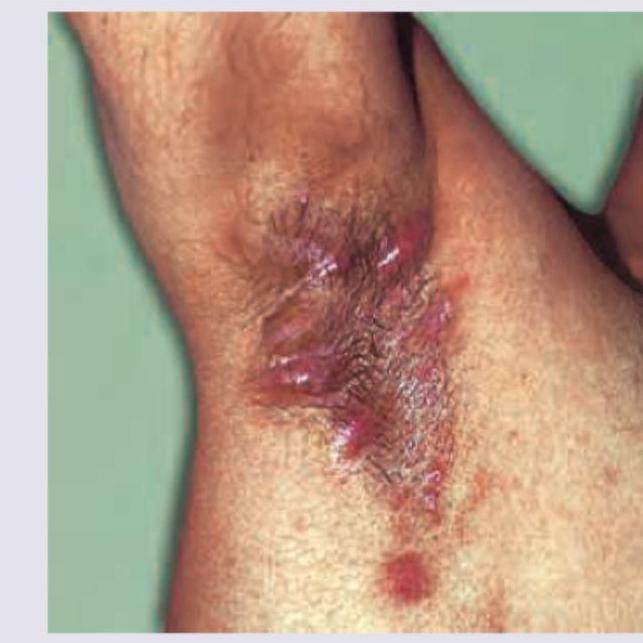
A 25-year-old female presents with the following lesions in the axilla, as shown by the arrow:
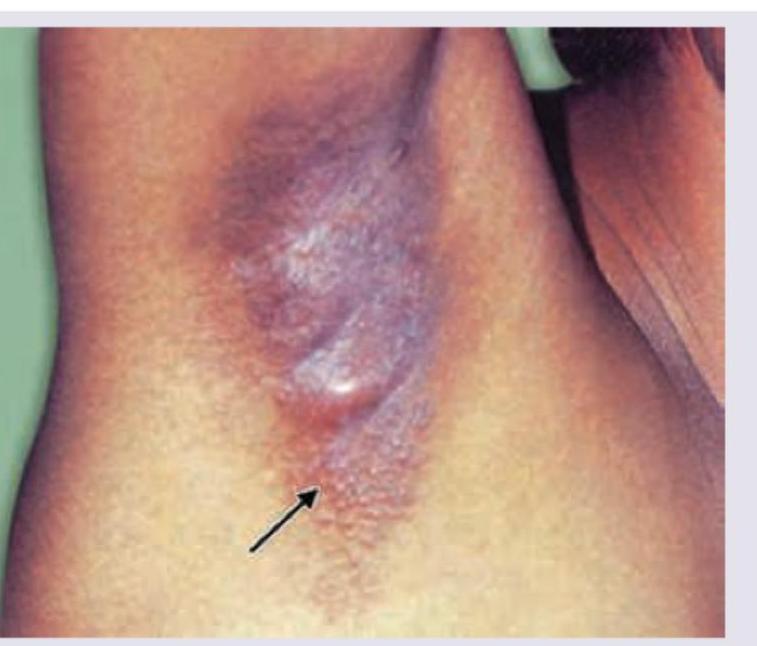
A young male smoker presents with long standing history of lesions in axilla. All are correct about the image shown below except:
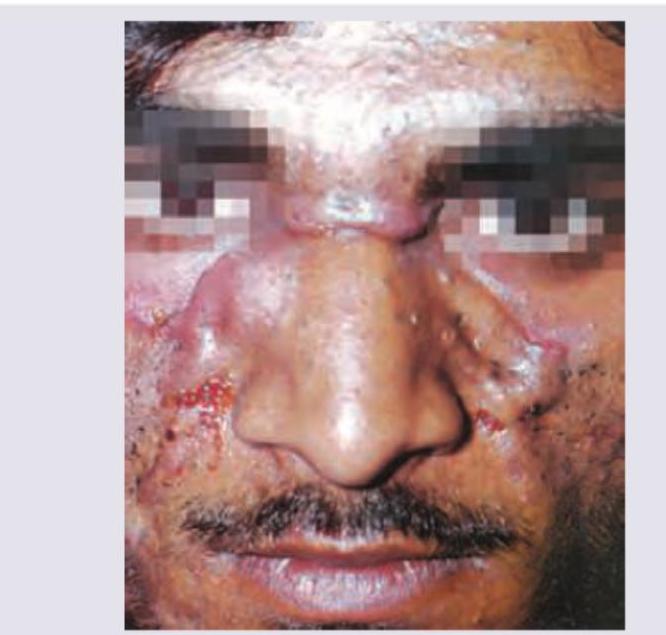
A patient presents with 1-year history of painful nodulocystic acne as shown in the image. Which of the following is the drug of choice for this case?
Practice by Chapter
Acne Vulgaris: Pathophysiology
Practice Questions
Acne Vulgaris: Clinical Types
Practice Questions
Acne Vulgaris: Management
Practice Questions
Acne in Special Populations
Practice Questions
Rosacea
Practice Questions
Perioral Dermatitis
Practice Questions
Hidradenitis Suppurativa
Practice Questions
Acne Keloidalis Nuchae
Practice Questions
Acne Scarring and Its Management
Practice Questions
Psychological Aspects of Acne
Practice Questions
Diet and Acne
Practice Questions
Newer Therapies in Acne Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
