Acne and Related Disorders — MCQs

On this page
Acne vulgaris is caused by which of the following?
Collarette of scales is a characteristic feature of which of the following dermatological conditions?
Tricholemmoma are:
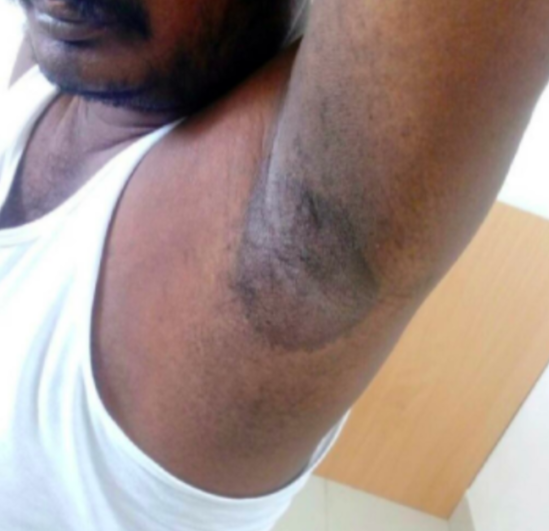
A 28-year-old female presents with a rash. Which of the following conditions is NOT associated with an increased risk of developing this rash?
Recalcitrant pustular acne is treated by which of the following?
All of the following are variants of Acne, EXCEPT:
Which of the following is NOT a component of SAPHO syndrome?
Which of the following is NOT a causative factor for acne vulgaris?
When a patient is on isotretinoin therapy, which of the following parameters should be monitored?
In sebaceous glands, what does the accumulation of sebum lead to?
Practice by Chapter
Acne Vulgaris: Pathophysiology
Practice Questions
Acne Vulgaris: Clinical Types
Practice Questions
Acne Vulgaris: Management
Practice Questions
Acne in Special Populations
Practice Questions
Rosacea
Practice Questions
Perioral Dermatitis
Practice Questions
Hidradenitis Suppurativa
Practice Questions
Acne Keloidalis Nuchae
Practice Questions
Acne Scarring and Its Management
Practice Questions
Psychological Aspects of Acne
Practice Questions
Diet and Acne
Practice Questions
Newer Therapies in Acne Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
