Acne and Related Disorders — MCQs

On this page
Rhinophyma is a type of?
A 35-year-old woman presents with a history of erythematous papulopustular lesions on the face, with diffuse redness on her cheeks. What is the most likely diagnosis?
Physical examination on a 65-year-old man with mild congestive heart failure reveals varicose veins, ankle edema, and inflammation of much of the skin near the ankles of both legs. The affected skin exhibits edema, erythema, mild scaling, and brown discoloration. The edges of skin involvement are poorly defined. On one ankle, a one centimeter diameter ulcerated area is seen within the erythematous area. The patient says that his leg lesions look much worse than they feel. Which of the following is the most likely diagnosis?
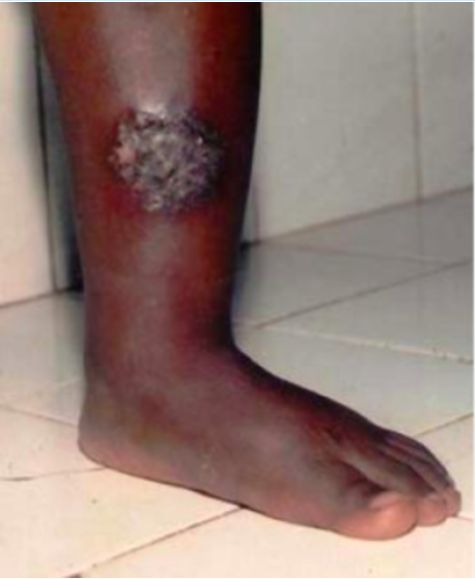
A farmer presents with a lesion on the leg. Which of the following is the most likely diagnosis?
A 58-year-old man complains of an enlarged, pitted nose, and a facial rash that flushes in response to drinking hot liquids or alcohol. The rash is on both cheeks and is red and flushed in appearance, with some telangiectasias and small papules. Which of the following is the most likely diagnosis?
The proportion of which of the acids is increased in acne comedones?
Rhinophyma is characterized by which of the following?
Rhinophyma is a complication of which of the following?
Treatment of acne vulgaris may include all except?
Hidradenitis suppurativa is commonly found in which of the following locations?
Practice by Chapter
Acne Vulgaris: Pathophysiology
Practice Questions
Acne Vulgaris: Clinical Types
Practice Questions
Acne Vulgaris: Management
Practice Questions
Acne in Special Populations
Practice Questions
Rosacea
Practice Questions
Perioral Dermatitis
Practice Questions
Hidradenitis Suppurativa
Practice Questions
Acne Keloidalis Nuchae
Practice Questions
Acne Scarring and Its Management
Practice Questions
Psychological Aspects of Acne
Practice Questions
Diet and Acne
Practice Questions
Newer Therapies in Acne Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
