Acne and Related Disorders — MCQs

On this page
An 18-year-old female presents with a complaint of recurrent acne on her face and neck. Which of the following is the preferred topical drug for treatment?
The condition seen in the illustration is:
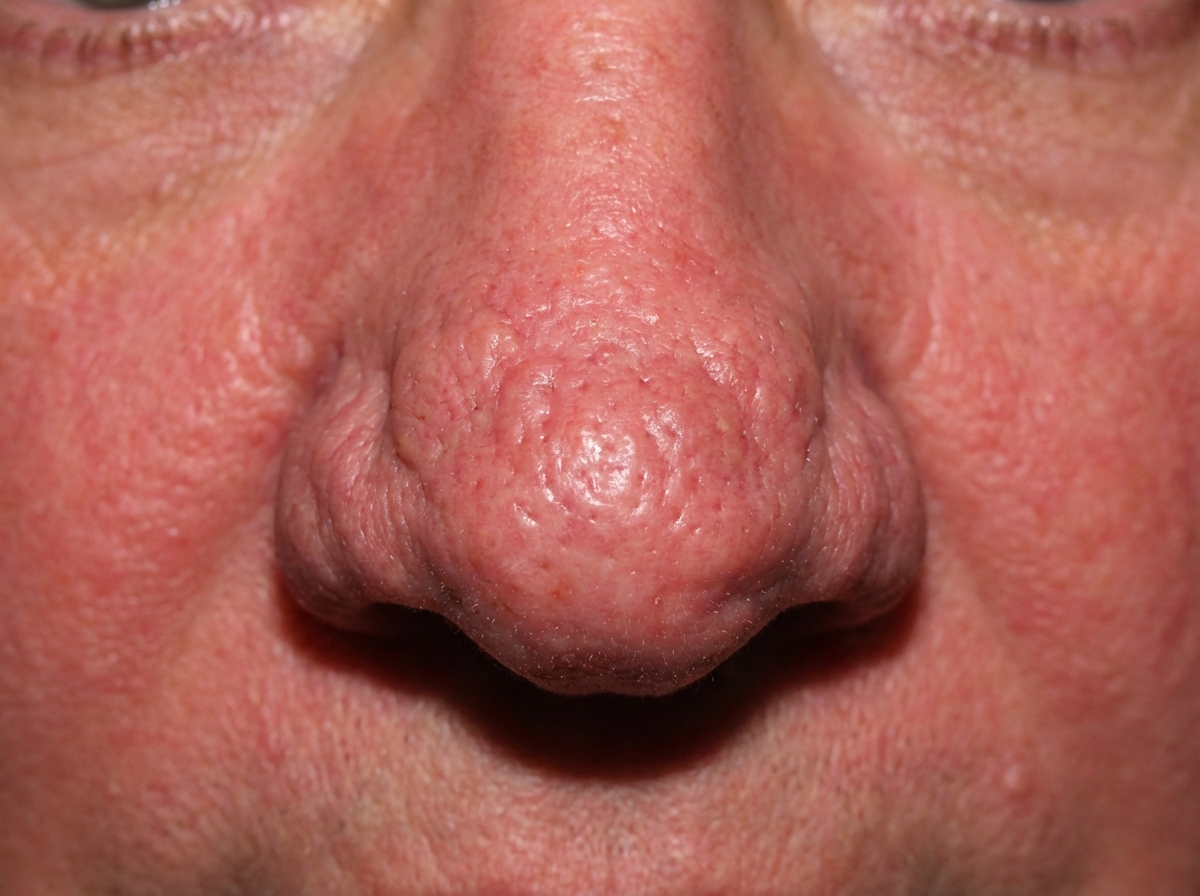
A patient presented with multiple nodulocystic lesions on the face. Which is the drug of choice for this condition?
A 50-year-old female presents with lesions on her cheek, chin, and forehead. On examination, the skin is erythematous with dilated blood vessels, nodules, and pustules, but no comedones. What is the most likely diagnosis?
A young person presents with comedones and papulo-pustular acne affecting the face, trunk, and back. What is the recommended management approach for this patient?
Which of the following is NOT a causative factor for acne?
Oral retinoid is indicated in the treatment of which condition?
A 17-year-old male is to be started on oral isotretinoin. What parameter should be measured before instituting therapy?
A teenage girl presented in OPD with moderate acne and a history of irregular menses. What treatment would you suggest?
Acne vulgaris primarily involves which structure?
Practice by Chapter
Acne Vulgaris: Pathophysiology
Practice Questions
Acne Vulgaris: Clinical Types
Practice Questions
Acne Vulgaris: Management
Practice Questions
Acne in Special Populations
Practice Questions
Rosacea
Practice Questions
Perioral Dermatitis
Practice Questions
Hidradenitis Suppurativa
Practice Questions
Acne Keloidalis Nuchae
Practice Questions
Acne Scarring and Its Management
Practice Questions
Psychological Aspects of Acne
Practice Questions
Diet and Acne
Practice Questions
Newer Therapies in Acne Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
