Nutrition and Health — MCQs

On this page
What is the percentage of fiber in animal foods?
Parboiling of rice reduces the incidence of which deficiency disease?
Dietary Reference Intake recommendations include all of the following except:
What is the most immediate treatment for night blindness?
What is the pH at which the initiation of dental caries begins?
Which of the following statements is FALSE?
Second degree of undernutrition means?
Which of the following statements is true regarding the given program?
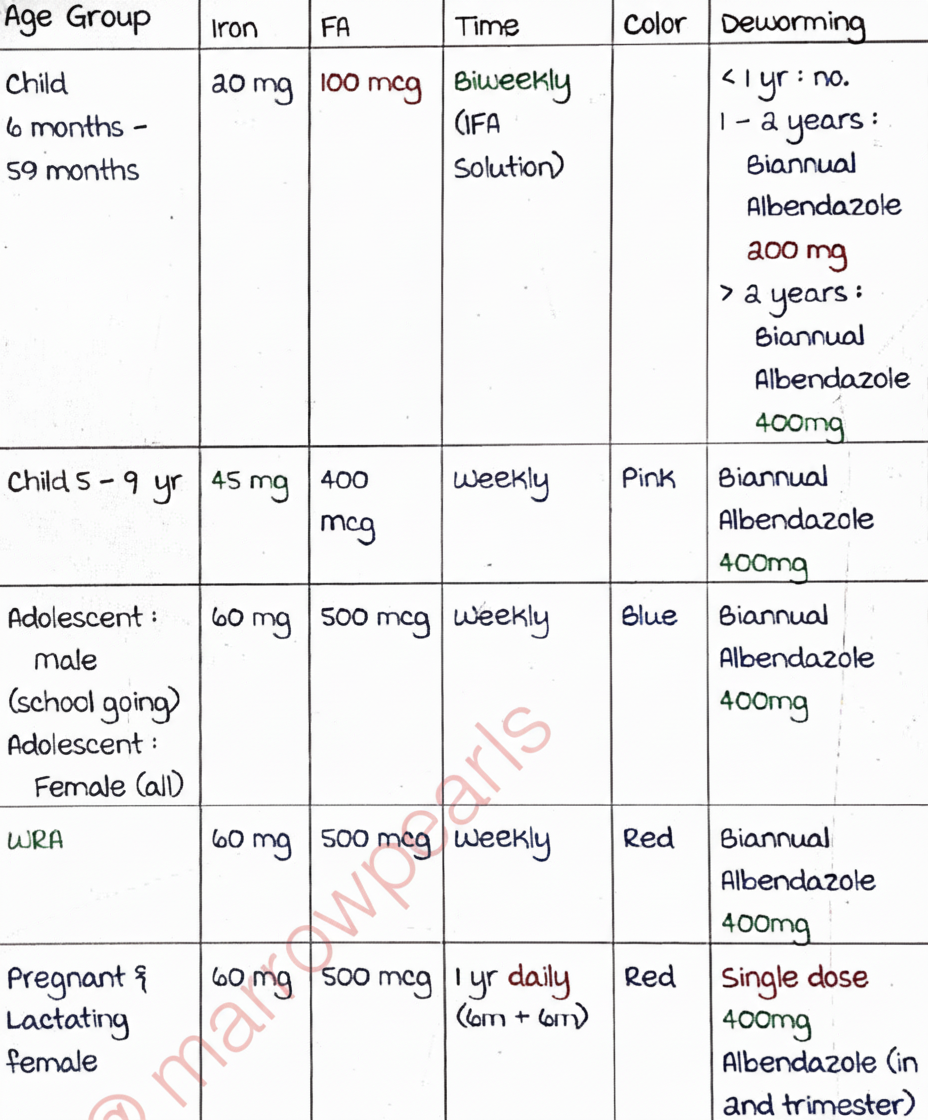
What is the recommended amount of cereal to be provided in the mid-day meal program?
Which of the following is NOT considered one of the three cardinal determinants of undernutrition?
Practice by Chapter
Basic Nutritional Requirements
Practice Questions
Assessment of Nutritional Status
Practice Questions
Protein-Energy Malnutrition
Practice Questions
Micronutrient Deficiencies
Practice Questions
Nutritional Programs in India
Practice Questions
Dietary Guidelines
Practice Questions
Food Safety and Security
Practice Questions
Diet and Non-Communicable Diseases
Practice Questions
Nutrition in Pregnancy and Lactation
Practice Questions
Infant and Young Child Nutrition
Practice Questions
Nutrition in Emergencies
Practice Questions
Food Fortification and Supplementation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
